Estrogen receptor alpha drives mTORC1 inhibitor-induced feedback activation of PI3K/AKT in ER+ breast cancer
2019-05-08
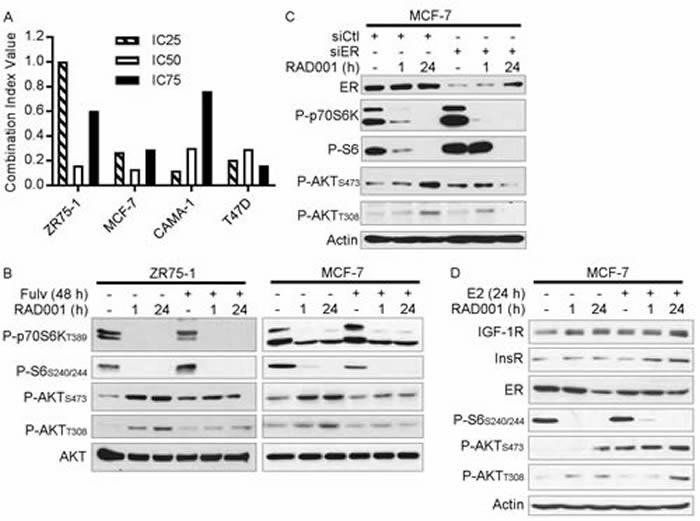
Researchers and authors from the Norris Cotton Cancer Center, Dartmouth-Hitchcock Medical Center, Geisel School of Medicine at Dartmouth, Lebanon, NH, USA hypothesized that mTORC1 inhibition activates the IGF-1R/Ins R/IRS-1/2 axis in an ER-dependent manner to drive PI3K/AKT and promote cancer cell survival, implicating ER in survival signaling induced by mTORC1 inhibition.
"Approximately 70% of primary breast tumors express estrogen receptor and/or progesterone receptor."
In patients with recurrent/metastatic ER+ breast cancer resistant to a non-steroidal AI, treatment with the steroidal AI exemestane plus the mTORC1 inhibitor everolimus significantly improved median progression-free survival compared to exemestane/placebo in the BOLERO-2 study.
Such findings supported the U.S. FDA approval of everolimus for use in combination with exemestane for patients with ER+ breast cancer resistant to a non-steroidal AI. However, the benefit of continued anti-estrogen therapy in the context of mTORC1 inhibition remains unproven; indeed, single-agent everolimus elicited clinical benefit in 6/22 patients with advanced ER+ breast cancer.
Preclinical data show that combined therapeutic targeting of ER and mTORC1 is more effective than single agents to inhibit growth and induce apoptosis of breast cancer cells and xenografts.
Herein, they demonstrated a role for ER in such feedback activation of survival pathways in breast cancer cell lines and human tumors, providing supportive rationale for using anti-estrogens to enhance the effects of mTORC1 inhibitors in ER+ breast cancer.
An exploratory subgroup analysis revealed that patients with cancer that had progressed during or within 12 months after the end of adjuvant AI therapy, rendering exemestane +/- everolimus the first-line therapy for their advanced disease, experienced even greater benefit from the addition of everolimus: exemestane/everolimus increased median PFS to 15.2 months from 4.2 months with exemestane/placebo.
Lingering questions remain regarding 1) the optimal time in the disease course to introduce everolimus, 2) the need for continued anti-estrogen therapy for anti-estrogen-resistant disease in the context of mTORC1 inhibition with everolimus, and 3) the clinical significance of mTORC1 inhibitor-induced feedback activation of upstream pathways.
Full text - https://www.oncotarget.com/article/24256/text/
Correspondence to - Todd W. Miller - [email protected]
Keywords - ER, mTOR, IGF-1R, feedback, everolimus
Copyright © 2026 Rapamycin Press LLC dba Impact Journals
Oncotarget ® is a registered trademark of Rapamycin Press LLC
Impact Journals ® is a registered trademark of Rapamycin Press LLC
RAPAMYCIN PRESS ® is a registered trademark of Rapamycin Press LLC




