INTRODUCTION
The incidence of nasopharyngeal carcinoma (NPC) is 15 to 50 cases per 100,000 annually in Southern China, Singapore, and Malaysia that vary with age, ethnicity, and geographical origin [1]. Radiotherapy (RT) is the standard treatment for NPC because of the anatomical location and the high radiosensitivity. Patients with locoregionally advanced (LA) NPC at diagnosis account for 60% to 70% of all NPC patients [2]. Intensity modulated radiation therapy (IMRT) has been used to improve locoregional control but provides little benefit for survival outcome and prevention of distant failure [3, 4]. According to meta-analyses of randomized studies, combination radiotherapy and chemotherapy reduces the risk of mortality by 18% and increases 5-year survival by 4% to 6% [5]. Concurrent chemoradiotherapy (CCRT) with or without adjuvant chemotherapy, which provides a benefit in overall survival, has become the standard treatment for LA NPC, although with acute toxicities [6-8]. A previous meta-analysis showed that compared with CCRT alone, addition of neoadjuvant chemotherapy (NAC) to CCRT reduces distant failure in LA NPC patients [9, 10], and another current meta-analysis confirmed that NAC followed by CCRT significantly improved progression-free survival (PFS) and overall survival (OS) [11]. However, the efficacy of the addition of NAC to CCRT in LA NPC patients remains controversial [12-14]. Considering these results, addition of NAC to CCRT has been a promising option for LA NPC patients in the era of IMRT. At present, the incidence of distant failure in LA NPC patients after combined treatment is more than 20% [15]. Therefore, new and effective regimens with tolerable toxicity for LA NPC are needed.
Overexpression of epidermal growth factor receptor (EGFR) is observed in many different cancers, including gliomas, sarcomas, and head and neck cancers [16]. Moreover, high EGFR expression is associated with poor prognosis [17, 18]. Several inhibitors of EGFR, such as cetuximab, panitumumab, erlotinib, and gefitinib, have shown favorable results in clinical trials [19, 20]. Cetuximab, the most commonly used anti-EGFR antibody, combined with radiotherapy (RT), has been shown to improve survival in patients with locoregionally advanced head and neck squamous cell carcinoma (LA HNSCC) [21]. In NPC, cetuximab with concurrent chemoradiotherapy is tolerable and has shown promising advantages for NPC prognosis [22]. However, the relatively high rate of mucositis and acne-like skin rash limit its clinical application [22, 23].
Nimotuzumab is a blocking anti-EGFR monoclonal antibody without intrinsic stimulating activity [24]. In the preclinical studies, nimotuzumab demonstrated antiproliferative, proapoptotic, and antiangiogenic activities [25], and nimotuzumab displayed a longer half-life and elevated area under the curve than cetuximab at the same dose level [26]. Nimotuzumab improves quality of life because it rarely causes severe dermatological toxicity, which is the most common adverse event resulting from cetuximab and panitumumab use [27].
Nimotuzumab has marketing approval for the treatment of LA NPC [28, 29]. However, the value of adding nimotuzumab to NAC followed by CCRT in LA NPC patients remains unclear. Therefore, we retrospectively investigated the safety and efficacy of nimotuzumab plus NAC followed by CCRT in LA NPC patients.
Results
Patient characteristics and completion of treatment
Between May 2008 and April 2014, the clinical data of 210 newly diagnosed LA NPC patients, who were initially treated with nimotuzumab plus NAC followed by CCRT in the Department of Radiation Oncology, Zhejiang Cancer Hospital (Hangzhou, People’s Republic of China), were collected and retrospectively reviewed. Basic characteristics of patients are summarized in Table 1. All patients completed a full course of radical IMRT and received 1 to 4 cycles of NAC, ≥ 1 cycle of concurrent chemotherapy (CC), and 3 to 17 weeks of nimotuzumab (Table 2). Among these patients, 95 (45.2%) received adjuvant chemotherapy (AC).
Table 1: Basic characteristic of 210 LA NPC patients
Characteristic |
N (%) |
Gender |
|
Male |
154 (73.3) |
Female |
56 (26.7) |
Age (years) |
|
Range |
13–72 |
Median |
46 |
<50 |
131 (62.4) |
≥ 50 |
35 (37.6) |
WHO pathology |
|
Type I |
9 (4.3) |
Type II |
3 (1.4) |
Type III |
198 (94.3) |
ECOG performance status |
|
0 |
168 (80.0) |
1 |
42 (20.0) |
T stage * |
|
T1 |
7 (3.3) |
T2 |
29 (13.8) |
T3 |
96 (45.7) |
T4 |
78 (37.2) |
N stage * |
|
N0 |
21 (10.0) |
N1 |
62 (29.5) |
N2 |
108 (51.4) |
N3 |
19 (9.1) |
Clinical stage * |
|
III |
117 (55.7) |
IVa |
75 (35.7) |
IVb |
18 (8.6) |
Comorbidity |
|
No |
154 (73.3) |
Yes |
56 (26.7) |
Abbreviations: WHO: World Health Organization. ECOG: Eastern Cooperative Oncology Group.
*The 7th AJCC/UICC staging system.
Table 2: Completion of treatment in 210 patients with LA NPC
Treatment |
N (%) |
NAC regimens |
|
TPF |
62 (29.5) |
TP |
64 (30.5) |
GP |
7 (3.3) |
FP |
73 (34.8) |
Other |
4 (1.9) |
Cycle of NAC |
|
1 |
40 (19.0) |
2 |
80 (38.1) |
3–4 |
90 (42.9) |
CC regimens |
|
Cisplatin |
198 (94.3) |
Non-cisplatin |
12 (5.7) |
Cycle of CC |
|
1 |
76 (36.2) |
2 |
120 (57.1) |
≥3 |
14 (6.7) |
Period of CC |
|
Weekly |
12 (5.7) |
3 weeks |
198 (94.3) |
AC |
|
No |
115 (54.8) |
Yes |
95 (45.2) |
Fractional dose of h-R3 |
|
100 mg |
23 (11.0) |
200 mg |
187 (89.0) |
Total dose of h-R3 |
|
< 1200 mg |
60 (28.6) |
≥ 1200 mg |
150 (71.4) |
Cycle of h-R3 |
|
< 6 weeks |
39 (18.6) |
≥ 6 weeks |
171 (81.4) |
Abbreviations: NAC: neoadjuvant chemotherapy. CC: concurrent chemotherapy. AC: adjuvant chemotherapy. h-R3: nimotuzumab.
Disease response
At the end of treatment, complete remission (CR) and partial remission (PR) for lesions of the nasopharynx in 210 LA NPC patients accounted for 83.8% (176/210) and 16.2% (34/210), respectively. For 189 patients with neck metastatic lymph nodes, CR and PR rates of cervical lymph nodes were 88.9% (168/189) and 11.1% (21/189), respectively.
Rates of local control and survival
The median follow-up time was 48 months (range, 13-75 months). The estimated 5-year local recurrence-free survival (LRFS), regional recurrence-free survival (RRFS), distant metastasis-free survival (DMFS), progression-free survival (PFS), and overall survival (OS) rates were 95.6%, 94.4%, 91.7%, 84.0%, and 88.7%, respectively (Figure 1). The 5-year OS rates were 100%, 90.1%, 91.0%, and 83.8% for patients with stage T1, T2, T3, and T4 disease, respectively (P = 0.080) (Figure 2A). However, the patients with stage T4 disease had poorer OS rates than those with stage T1-T3 disease (83.8% vs. 91.4%, P = 0.011) (Figure 2B). The 5-year OS and PFS rates were 92.7%, 83.2%, and 85.0% and 89.9%, 79.8%, and 64.2% for patients with stage III, stage IVa, and stage IVb, respectively (P = 0.020) (Figure 2C), (P = 0.012) (Figure 3A). The 5-year OS rate of patients treated with a CC regimen of cisplatin was higher than that of non-cisplatin CC regimens (89.9% vs. 69.4%) (P = 0.036) (Figure 2D). The 5-year PFS rates were 90.2%, 89.9%, 89.2%, and 78.2% for patients with stage N0, N1, N2, and N3 disease, respectively (P = 0.012) (Figure 3B). The 5-year PFS rates for patients with AC vs. without AC and CR patients vs. non-CR patients were 89.4% vs. 77.9% (P = 0.030) (Figure 3C) and 88.5% vs. 69.8% (P = 0.008) (Figure 3D), respectively.
Treatment failure occurred in 31 patients by the last follow-up. Local relapse occurred in 7 patients, regional relapse occurred in 8 patients, and locoregional relapse occurred in 1 patient. Distant failure was experienced by15 patients. Patterns of treatment failure in NPC patients are listed in Table 3.
Table 3: Patterns of treatment failure in nasopharyngeal carcinoma patients
Sites |
Number of patients (n = 31) |
Local relapse only |
7 |
Regional relapse only |
8 |
Local and regional failure |
1 |
Regional and distant failure |
2 |
Distant failure only |
13 |
Lung metastasis only |
3 |
Bone metastasis only |
2 |
Liver metastasis only |
2 |
Lung, liver, bone and other |
6 |
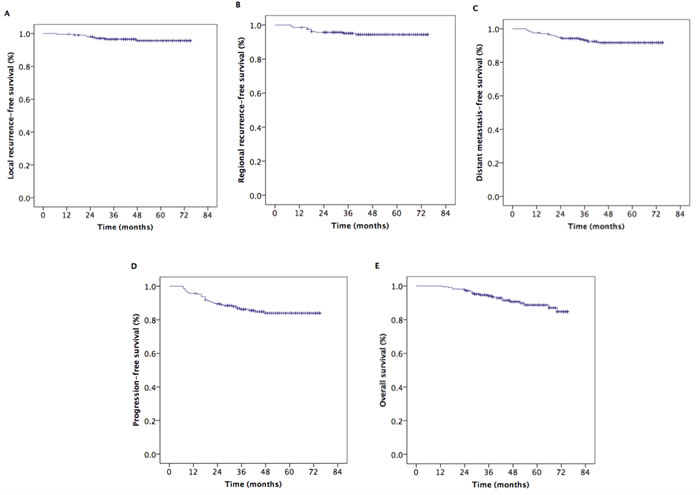
Figure 1: Kaplan–Meier estimates of the survival in patients with nasopharyngeal carcinoma. A. Local recurrence-free survival, B. regional recurrence-free survival, C. distance metastasis-free survival, D. progression-free survival, and E. overall survival.
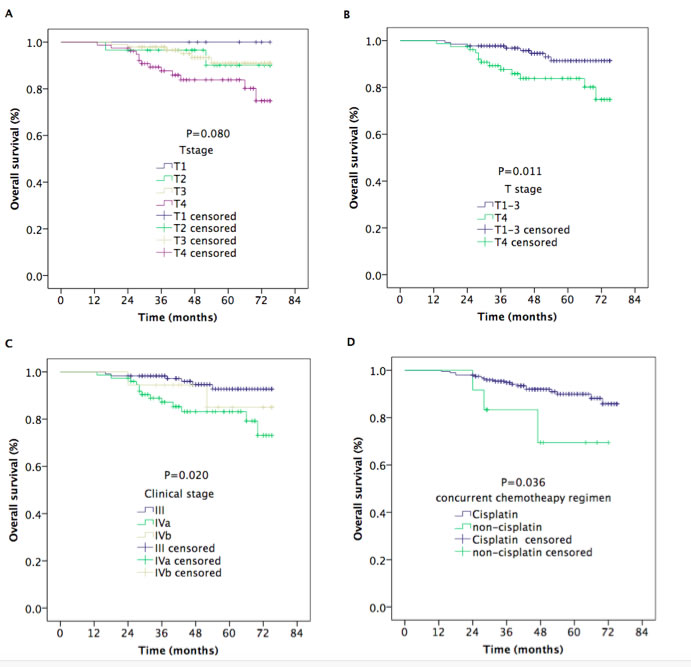
Figure 2: Kaplan–Meier estimates of the overall survival in nasopharyngeal carcinoma patients for different variable. A. Overall survival for T stages, B. overall survival for stage T4 vs. T1-T3, C. overall survival for clinical stage, and D. overall survival for concurrent chemotherapy regimens.
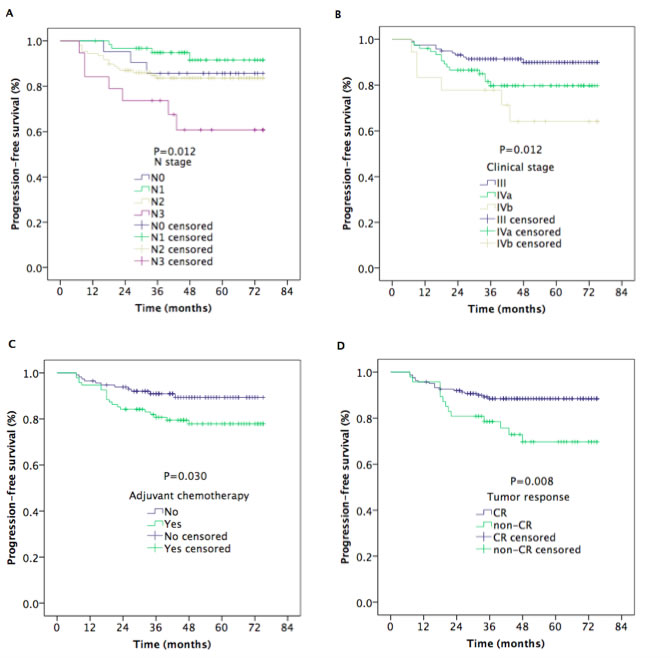
Figure 3: Kaplan–Meier estimates of the progression-free survival in nasopharyngeal carcinoma patients for univariate. A. Progression-free survival for N stages, B. progression-free survival for clinical stages, C. progression-free survival of patients with or without AC, and D. progression-free survival for tumor response.
Identification of prognostic factors
We evaluated the following potential prognostic factors: patient age, patient gender, clinical stage, adjusted tumor (T) and lymph node (N) stage, NAC, CCRT, AC, comorbidities, dose of nimotuzumab, and tumor response at the end of treatment. Univariate analysis revealed that clinical stage and CCRT regimens were significant prognostic factors for OS, and N stage, clinical stage, and tumor response at the end of treatment were significant prognostic factors for PFS (Table 4). In multivariate analysis, stage IV was a poorer prognostic factor for OS, PFS and DMFS, as were CC regimen of non-cisplatin for OS and DMFS and non-CR for OS and RRFS (Table 5).
Table 4: Univariate analysis of prognostic factors on OS and PFS in LA NPC patients
Characteristic |
N |
5-year OS (%) |
P |
5-year PFS (%) |
P |
Gender |
0.319 |
0.058 |
|||
Male |
154 |
86.6 |
80.7 |
||
Female |
17 |
94.0 |
92.6 |
||
Age (years) |
0.124 |
0.870 |
|||
<50 |
131 |
90.5 |
83.6 |
||
≥ 50 |
79 |
85.4 |
84.8 |
||
T stage * |
0.080 |
0.361 |
|||
T1 |
7 |
100.0 |
85.7 |
||
T2 |
29 |
90.1 |
81.4 |
||
T3 |
96 |
91.0 |
88.4 |
||
T4 |
78 |
83.8 |
79.3 |
||
N stage * |
0.884 |
0.012 |
|||
N0 |
21 |
90.2 |
85.7 |
||
N1 |
62 |
89.9 |
91.6 |
||
N2 |
108 |
89.2 |
83.6 |
||
N3 |
19 |
78.2 |
60.8 |
||
Clinical stage * |
0.012 |
0.012 |
|||
III |
117 |
92.7 |
89.9 |
||
IVA |
75 |
83.2 |
79.8 |
||
IVB |
18 |
85.0 |
64.2 |
||
Comorbidity |
0.193 |
0.640 |
|||
No |
154 |
89.5 |
83.2 |
||
Yes |
56 |
86.3 |
86.4 |
||
NAC regimens |
0.257 |
0.462 |
|||
TPF |
62 |
89.9 |
79.3 |
||
TP |
64 |
90.9 |
89.8 |
||
GP# |
7 |
- |
- |
||
FP |
73 |
83.3 |
82.1 |
||
Other |
4 |
100.0 |
|||
Cycle of NAC |
0.447 |
0.169 |
|||
1 |
40 |
84.8 |
74.9 |
||
2 |
80 |
89.3 |
85.2 |
||
3–4 |
90 |
89.8 |
87.0 |
||
Period of CC |
0.992 |
0.781 |
|||
Weekly |
12 |
85.7 |
84.1 |
||
3 weeks |
198 |
88.9 |
83.3 |
||
CC regimens |
0.036 |
0.230 |
|||
Cisplatin |
198 |
89.9 |
84.6 |
||
Non-cisplatin |
12 |
69.4 |
75.0 |
||
AC |
0.369 |
0.030 |
|||
No |
115 |
91.6 |
89.4 |
||
Yes |
95 |
86.3 |
77.9 |
||
Fractional dose of h-R3 |
0.966 |
0.896 |
|||
100 mg |
23 |
86.7 |
87.0 |
||
200 mg |
186 |
88.7 |
83.4 |
||
Total dose of h-R3 |
0.976 |
0.459 |
|||
< 1200 mg |
60 |
83.6 |
85.2 |
||
≥ 1200 mg |
120 |
84.3 |
90.0 |
||
Tumor response |
0.270 |
0.008 |
|||
CR |
163 |
90.8 |
88.5 |
||
Non-CR |
47 |
81.4 |
69.8 |
Abbreviations: NAC: neoadjuvant chemotherapy. CC: concurrent chemotherapy. AC: adjuvant chemotherapy. h-R3: nimotuzumab. CR: complete response.
*The 7th AJCC/UICC staging system. # Patients, who treated with GP, lived fewer than 5 years.
Table 5: Multivariate analysis of prognostic factors in LA NPC patients
Characteristic |
HR |
95% CI |
P-value |
|
OS |
CC regimen of cisplatin vs. non-cisplatin |
0.256 |
0.074–0.886 |
0.031 |
III vs. IV* |
0.291 |
0.113–0.754 |
0.011 |
|
PFS |
III vs. IV* |
0.438 |
0.213–0.899 |
0.024 |
CR vs. non-CR |
0.441 |
0.210–0.926 |
0.031 |
|
LRFS |
— |
— |
— |
— |
RRFS |
CR vs. non-CR |
0.300 |
0.091–0.994 |
0.049 |
With vs. without AC |
0.222 |
0.047–1.043 |
0.057 |
|
DMFS |
CC regimen of cisplatin vs. non-cisplatin |
0.207 |
0.058–0.734 |
0.015 |
III vs. IV* |
0.166 |
0.047–0.583 |
0.005 |
Abbreviations: OS: overall survival. PFS: progression-free survival. LRFS: local recurrence-free survival. RRFS: regional recurrence-free survival. DMFS: distant metastasis-free survival. CC: concurrent chemotherapy. AC: adjuvant chemotherapy.
*The 7th AJCC/UICC staging system.
Safety and toxicity
The most common treatment-related acute adverse events included hematologic and non- hematologic toxicity (Table 6). During the period of NAC, hematologic toxicity was reported as grade 3 and worse in severity in 45 patients (21.4%). Of these patients, 8 experienced neutropenic fever. The toxicities can be tolerated without delaying the chemotherapy and interrupting radiotherapy by GMSF treatment. The gastrointestinal toxicities were mild or moderate, and patients recovered rapidly with or without symptomatic medication. During the period of CCRT, the grade 3-4 hematologic toxicities and radiotherapy-related oral mucositis were reported in 14 patients (6.7%) and 9 patients (4.3%), respectively. Grade 3 dermatitis was observed in 5 patients within the RT field. No acneiform eruptions were found among these patients.
The most commonly observed late complication was xerostomia. However, the degree typically decreased over time. The degree of dry mouth in most patients was mild-to-moderate at the time of the last follow-up, and 123 patients did not complain of xerostomia. Finally, 79 patients developed either unilateral or bilateral hearing impairment, and 11 patients were found to have temporal lobe damage, which was diagnosed during follow-up based on magnetic resonance imaging.
Table 6: Toxicity of nimotuzumab plus NAC followed by CCRT with or without AC
Adverse events |
During the period of NAC |
During the period of CCRT |
||||||||
0 |
1 |
2 |
3 |
4 |
0 |
1 |
2 |
3 |
4 |
|
White blood cell |
63 |
57 |
45 |
35 |
10 |
131 |
36 |
29 |
9 |
5 |
Leukocytopenia |
72 |
52 |
41 |
32 |
13 |
132 |
34 |
31 |
10 |
3 |
Anemia |
180 |
22 |
6 |
2 |
0 |
109 |
55 |
39 |
7 |
0 |
Thrombocytopenia |
184 |
17 |
6 |
3 |
0 |
147 |
38 |
23 |
2 |
0 |
Liver function |
198 |
8 |
4 |
0 |
0 |
192 |
15 |
3 |
0 |
0 |
Renal function |
203 |
7 |
0 |
0 |
0 |
206 |
3 |
1 |
0 |
0 |
Mucositis |
175 |
27 |
8 |
0 |
0 |
44 |
84 |
73 |
7 |
2 |
Dermatitis |
210 |
0 |
0 |
0 |
0 |
0 |
138 |
67 |
5 |
0 |
Diarrhea |
197 |
9 |
3 |
1 |
0 |
202 |
6 |
2 |
0 |
0 |
Nausea/vomiting |
157 |
29 |
17 |
5 |
2 |
172 |
25 |
12 |
1 |
0 |
Abbreviations: NAC: neoadjuvant chemotherapy. CCRT: concurrent chemoradiotherapy.
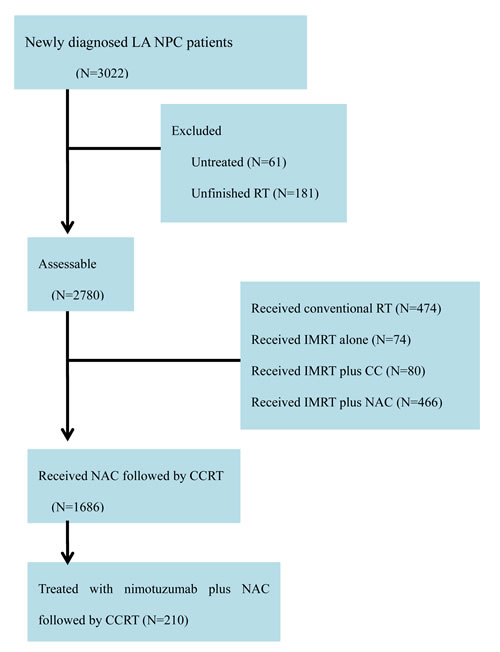
Figure 4: Flowchart of patients. Abbreviations: NPC: Nasopharyngeal carcinoma; RT: Radiotherapy.
Discussion
With further research on the molecular mechanism of tumorigenesis and tumor development, targeted molecular therapy in patients with NPC will become the research focus. Overexpression of EGFR was detected in 94% of patients with NPC [18]. Cetuximab is a common anti-EGFR monoclonal antibody drug. It has a good curative effect in the treatment of NPC, with a 2-year PFS of 86.5% to 89.3% and a 3-year OS of 90.9% [22], but severe oral mucositis and itchy acneiform rash limit its application in NPC. To minimize cetuximab-related toxicities, a novel EGFR-targeted agent without toxicities is warranted.
Nimotuzumab, a humanized immunoglobulin G1 (IgG1) isotype monoclonal antibody with a unique safety profile and low skin toxicity, has been approved for the treatment of non-NPC HNSCC [16, 30]. The advantage of the drug is that the affinity constant is lower than that of cetuximab, allowing for high tumor uptake and low normal-tissue uptake [31]. Nimotuzumab requires bivalent binding for stable attachment, which makes the agent selectively bind to tumors with moderate-to-high EGFR levels. When EGFR expression is low, as in tissue, cetuximab still has high binding ability because of its higher affinity constant [31]. Our experiment confirmed that nimotuzumab sensitizes nasopharyngeal carcinoma cell line CNE-2 in vitro to RT and can reduce cancer cell proliferation, induce cell apoptosis, and change cell cycle distribution [32]. All these effects indicate that nimotuzumab plus RT can be utilized in the design of the clinical trial of NPC.
To date, only four small-scale studies on adding nimotuzumab to RT or CCRT for NPC patients have been conducted. In a retrospective paired study by Li et al [33], the OS and PFS rates for the nimotuzumab/RT treatment group were lower than those for cisplatin/RT treatment group, but in the stage II or the older than 60 years subgroups, no significant differences were seen for OS and PFS. Zhai et al reported that the addition of nimotuzumab to IMRT showed promising locoregional control and survival outcomes for LA NPC patients [29]. Huang et al [34] and Liu et al [28] found that concurrent administration of nimotuzumab and CCRT yielded encouraging survival outcomes in LA NPC patients, with tolerable treatment-related toxicity. For the first two studies, because of the severe acute sequela of CCRT, nimotuzumab, as a preferred substrate for cisplatin, increased the quality of life in selected NPC patients, with similar treatment outcomes. However, in the last two studies, nimotuzumab added into the intensive modality of NAC followed by CCRT improved the survival of LA NPC patients but with normal-tissue damage. Those outcomes will be the direction of further research.
This study investigated the efficacy and safety of adding nimotuzumab to NAC followed by CCRT for LA NPC patients. The study showed promising clinical outcomes, with a 5-year LRFS of 95.6%, a 5-year RRFS of 94.4%, a 5-year DMFS of 91.7%, a 5-year PFS of 84.0%, and a 5-year OS of 88.7%. Univariate analysis revealed that clinical stage and CCRT regimens are significant prognostic factors for OS, and N stage, clinical stage, and tumor response at the end of treatment are significant prognostic factor for PFS. Multivariate analysis indicated that stage IV is a poorer prognostic factor for OS, PFS and DMFS, as stage N2 to N3 is for PFS and DMFS, a CCRT regimen of non-cisplatin is for OS and DMFS, and a non-CR is for OS and RRFS. Although 34.7% of patients experienced grade ≥3 hematologic toxicity and 12.0% experienced grade ≥3 radiotherapy-related oral mucositis, only 5 patients were observed with grade 3 dermatitis within the RT field. No acneiform eruptions were found among these patients.
We found that nimotuzumab plus NAC before CCRT with or without AC in the treatment of LA NPC patients is safe and effective. However, because of the retrospective nature of the study, our results should be regarded as preliminary.
Conclusion
We observed that the administration of nimotuzumab with NAC followed by CCRT in LA NPC patients was tolerated and showed promising clinic outcomes. Further randomized, controlled, multicenter phase III clinical trials are needed to confirm the therapeutic gain.
Patients and methods
Pretreatment
The patients enrolled into this study were hospitalized from May 2008 to April 2014 in the Department of Radiation Oncology, Zhejiang Cancer Hospital. The retrospective study was approved by the medical ethics committee of Zhejiang Cancer Hospital. The eligible patients met the following criteria: (i) histologically proven LA NPC, (ii) Eastern Cooperative Oncology Group performance status ≤ 1, (iii) completion of radical IMRT, (iv) received nimotuzumab plus NAC before CCRT, and (v) no previous anti-cancer treatment.
Patients had pretreatment evaluations that included complete histories, physical examinations, hematology and biochemistry profiles, chest radiographs, sonography of the abdomen, bone scans, magnetic response images of the nasopharynx, and nasopharyngoscopies. All patients were staged per the 2010 American Joint Committee on Cancer staging system. Tumor histology was classified per the World Health Organization classification.
The flowchart of patients is shown in Figure 4. A total of 3022 newly diagnosed LA NPC patients were registered at Zhejiang Cancer Hospital. A total of 210 NPC patients treated with nimotuzumab plus NAC followed by CCRT were enrolled into this study. All patients received definitive IMRT with or without AC.
Radiotherapy
All patients were immobilized in the supine position with thermoplastic masks. Computed tomography scans with intravenous contrast (2.5 mm slices from the head to 2 cm below the sternoclavicular joints) were performed for planning. All patients underwent radical IMRT with a simultaneous integrated boost technique that used 6-MV photons. The prescribed radiation doses were 69 Gy or 72 Gy to planning gross target volume (PGTV)nx, 66 Gy to 69 Gy to PGTVnd, 63 Gy to 66 Gy to planning target volume (PTV)nx, 60 Gy to 63 Gy to PTV1, and 51 Gy to 54 Gy to PTV2, delivered in 30 or 33 fractions. Radiation was delivered once daily, in five fractions per week, over 6 to 6.5 weeks for IMRT planning. The dose to organs at risk was limited based on the Radiation Therapy Oncology Group 0225 protocol.
Target treatment
Nimotuzumab was administered concomitantly with induction chemotherapy and /or RT at a dose of 100 mg or 200 mg weekly, which was diluted in 250 mL of saline to obtain a 100-mg or 200-mg suspension and intravenously infused over 1 hour. All patients received 3 to 17 weeks of nimotuzumab during the treatment.
Chemotherapy
All patients were given one to four cycles of platinum-based induction chemotherapy. The most common induction regimens included TPF (docetaxel 60 mg/m2/day on day 1, cisplatin 25 mg/m2/day on days 1 to 3, and 5-fluorouracil 500 mg/m2/day on days 1 to 3), TP (docetaxel 60 mg/m2/day on day 1, cisplatin 25 mg/m2/day on days 1 to 3), GP (gemcitabine 1,000 mg/m2/day on days 1 and 8, cisplatin 25 mg/m2/day on days 1 to 3), and FP (cisplatin 25 mg/m2/day on days 1 to 3, and 5-fluorouracil 500 mg/m2/day on days 1 to 3).
NPC patients underwent ≥1 cycle concurrent chemotherapy with cisplatin (80 mg /m2) for 3 days, and 95 patients received two to three courses of adjuvant chemotherapy with FP regimen 3 weeks after RT.
Patient evaluation and follow-up
The assessment of tumor response was performed thrice after the completion of induction chemotherapy, at the end of IMRT, and 3 months after irradiation, which was based on MRI and nasopharynx fiberscope per the Response Evaluation Criteria for Solid Tumors. Systemic chemotherapy adverse effects were graded per the National Cancer Institute Common Toxicity Criteria (NCI CTCAE, Version 3.0), and RT-induced toxicities were scored per the Acute and Late Radiation Morbidity Scoring Criteria of the Radiation Therapy Oncology Group.
All the subjects underwent weekly examinations for treatment response and toxicities during RT. Patients were followed every 3 months in the first 2 years, every 6 months from the third to the fifth year, and then annually. Each follow-up included careful examination of the nasopharynx and neck nodes by an experienced doctor. MRI scan of the nasopharynx, nasopharynx fiberscope, chest computed tomography radiograph, and ultrasound of abdomen were performed 3 months after the completion of RT and every 6 to 12 months thereafter. Additional examinations were performed when indicated to evaluate local relapse or distant metastasis.
Statistical analysis
Survival curves were generated by use of the Kaplan–Meier method. The curves were compared by use of log-rank tests. Multivariate analysis was performed by use of Cox regression models to identify significant prognostic factors. Hazard ratios (HRs) and 95% confidence intervals (CIs) were calculated for each prognostic factor. IBM SPSS Statistics Version 19.0 was used for all data analysis. A P < 0.05 was considered statistically significant. Survival time was calculated from the date of diagnosis to the most recent follow-up or to either the date of relapse (event-free, local recurrence-free, or distant metastasis-free) or death (overall survival). After recurrence or metastasis, patients were given salvage therapy as determined by their physicians.
funding
This study was supported by grants from the Medical Science Foundation of Zhejiang Health Bureau (No. 2013KYB033, No. 2009B026, No. 2006A016, No. 2005B012, No. 2004B014), National Natural Science Foundation of China (No. 81502646, No. 81502647).
Conflicts of interest
The authors declare that there are no conflicts of interest.
REFERENCES
1. Tang LL, Chen WQ, Xue WQ, He YQ, Zheng RS, Zeng YX, Jia WH. Global trends in incidence and mortality of nasopharyngeal carcinoma. Cancer Lett. 2016; 374:22–30.
2. Chen L, Mao YP, Xie FY, Liu LZ, Sun Y, Tian L, Tang LL, Lin AH, Li L, Ma J. The seventh edition of UICC/AJCC staging system for nasopharyngeal carcinoma is prognostically useful for patients treated with intensity-modulated radiotherapy from an endemic area in China. Radiother Oncol. 2012;104:331-337.
3. Wee J. Nasopharyngeal cancer: a promising future. Lancet Oncol. 2012; 13:116–18.
4. Lai SZ, Li WF, Chen L, Luo W, Chen YY, Liu LZ, Sun Y, Lin AH, Liu MZ, Ma J. How does intensity-modulated radiotherapy versus conventional two-dimensional radiotherapy influence the treatment results in nasopharyngeal carcinoma patients? Int J Radiat Oncol Biol Phys. 2011; 80:661–68.
5. Al-Sarraf M, Reddy MS. Nasopharyngeal carcinoma. Curr Treat Options Oncol. 2002; 3:21–32.
6. Al-Sarraf M, LeBlanc M, Giri PG, Fu KK, Cooper J, Vuong T, Forastiere AA, Adams G, Sakr WA, Schuller DE, Ensley JF. Chemoradiotherapy versus radiotherapy in patients with advanced nasopharyngeal cancer: phase III randomized Intergroup study 0099. J Clin Oncol. 1998; 16:1310–17.
7. Lee AW, Tung SY, Chua DT, Ngan RK, Chappell R, Tung R, Siu L, Ng WT, Sze WK, Au GK, Law SC, O’Sullivan B, Yau TK, et al. Randomized trial of radiotherapy plus concurrent-adjuvant chemotherapy vs radiotherapy alone for regionally advanced nasopharyngeal carcinoma. J Natl Cancer Inst. 2010; 102:1188–98.
8. Baujat B, Audry H, Bourhis J, Chan AT, Onat H, Chua DT, Kwong DL, Al-Sarraf M, Chi KH, Hareyama M, Leung SF, Thephamongkhol K, Pignon JP, and MAC-NPC Collaborative Group. Chemotherapy in locally advanced nasopharyngeal carcinoma: an individual patient data meta-analysis of eight randomized trials and 1753 patients. Int J Radiat Oncol Biol Phys. 2006; 64:47–56.
9. OuYang PY. Xie C, Mao YP, Zhang Y, Liang XX, Su Z, Liu Q, Xie FY. Significant efficacies of neoadjuvant chemotherapy and adjuvant chemotherapy for nasopharyngeal carcinoma by meta-analysis of published literature-based randomized, control trials. Ann Oncol. 2013; 24:2136–46.
10. Chen YP, Guo R, Liu N, Liu X, Mao YP, Tang LL, Zhou GQ, Lin AH, Sun Y, Ma J. Efficacy of the additional neoadjuvant chemotherapy to concurrent chemoradiotherapy for patients with locoregionally advanced nasopharyngeal carcinoma: a Bayesian network meta-analysis of randomized controlled trials. J Cancer. 2015; 6:883–92.
11. Wang M, Tian H, Li G, Ge T, Liu Y, Cui J, Han F. Significant benefits of adding neoadjuvant chemotherapy before concurrent chemoradiotherapy for locoregionally advanced nasopharyngeal carcinoma: a meta-analysis of randomized controlled trials. Oncotarget. 2016; 7:48375-48390. https://doi.org/10.18632/oncotarget.10237
12. Hui EP, Ma BB, Leung SF, King AD, Mo F, Kam MK, Yu BK, Chiu SK, Kwan WH, Ho R, Chan I, Ahuja AT, Zee BC, Chan AT. Randomized phase II trial of concurrent cisplatin-radiotherapy with or without neoadjuvant docetaxel and cisplatin in advanced nasopharyngeal carcinoma. J Clin Oncol. 2009; 27:242–49.
13. Fountzilas G, Ciuleanu E, Bobos M, Kalogera-Fountzila A, Eleftheraki AG, Karayannopoulou G, Zaramboukas T, Nikolaou A, Markou K, Resiga L, Dionysopoulos D, Samantas E, Athanassiou H, et al. Induction chemotherapy followed by concomitant radiotherapy and weekly cisplatin versus the same concomitant chemoradiotherapy in patients with nasopharyngeal carcinoma: a randomized phase II study conducted by the Hellenic Cooperative Oncology Group (HeCOG) with biomarker evaluation. Ann Oncol. 2012; 23:427–35.
14. Huang PY, Cao KJ, Guo X, Mo HY, Guo L, Xiang YQ, Deng MQ, Qiu F, Cao SM, Guo Y, Zhang L, Li NW, Sun R, et al. A randomized trial of induction chemotherapy plus concurrent chemoradiotherapy versus induction chemotherapy plus radiotherapy for locoregionally advanced nasopharyngeal carcinoma. Oral Oncol. 2012; 48:1038–44.
15. Wu F, Wang R, Lu H, Wei B, Feng G, Li G, Liu M, Yan H, Zhu J, Zhang Y, Hu K. Concurrent chemoradiotherapy in locoregionally advanced nasopharyngeal carcinoma: treatment outcomes of a prospective, multicentric clinical study. Radiother Oncol. 2014; 112:106–11.
16. Reddy BK, Lokesh V, Vidyasagar MS, Shenoy K, Babu KG, Shenoy A, Naveen T, Joseph B, Bonanthaya R, Nanjundappa, Bapsy PP, Loknatha, Shetty J, et al. Nimotuzumab provides survival benefit to patients with inoperable advanced squamous cell carcinoma of the head and neck: a randomized, open-label, phase IIb, 5-year study in Indian patients. Oral Oncol. 2014; 50:498–505.
17. Herbst RS, Shin DM. Monoclonal antibodies to target epidermal growth factor receptor-positive tumors: a new paradigm for cancer therapy. Cancer. 2002; 94:1593–611.
18. Chua DT, Nicholls JM, Sham JS, Au GK. Prognostic value of epidermal growth factor receptor expression in patients with advanced stage nasopharyngeal carcinoma treated with induction chemotherapy and radiotherapy. Int J Radiat Oncol Biol Phys. 2004; 59:11–20.
19. Köhler J, Schuler M. Afatinib, erlotinib and gefitinib in the first-line therapy of EGFR mutation-positive lung adenocarcinoma: a review. Onkologie. 2013; 36:510–18.
20. Yewale C, Baradia D, Vhora I, Patil S, Misra A. Epidermal growth factor receptor targeting in cancer: a review of trends and strategies. Biomaterials. 2013; 34:8690–707.
21. Bonner JA, Harari PM, Giralt J, Cohen RB, Jones CU, Sur RK, Raben D, Baselga J, Spencer SA, Zhu J, Youssoufian H, Rowinsky EK, Ang KK. Radiotherapy plus cetuximab for locoregionally advanced head and neck cancer: 5-year survival data from a phase 3 randomised trial, and relation between cetuximab-induced rash and survival. Lancet Oncol. 2010; 11:21–28.
22. Feng HX, Guo SP, Li GR, Zhong WH, Chen L, Huang LR, Qin HY, Baselga J, Spencer SA, Zhu J, Youssoufian H, Rowinsky EK, Ang KK. Toxicity of concurrent chemoradiotherapy with cetuximab for locoregionally advanced nasopharyngeal carcinoma. Med Oncol. 2014; 31:170–78.
23. He X, Xu J, Guo W, Jiang X, Wang X, Zong D. Cetuximab in combination with chemoradiation after induction chemotherapy of locoregionally advanced nasopharyngeal carcinoma: preliminary results. Future Oncol. 2013; 9:1459–67.
24. Talavera A, Friemann R, Gómez-Puerta S, Martinez-Fleites C, Garrido G, Rabasa A, López-Requena A, Pupo A, Johansen RF, Sánchez O, Krengel U, Moreno E. Nimotuzumab, an antitumor antibody that targets the epidermal growth factor receptor, blocks ligand binding while permitting the active receptor conformation. Cancer Res. 2009; 69:5851–59.
25. Crombet T, Osorio M, Cruz T, Roca C, del Castillo R, Mon R, Iznaga-Escobar N, Figueredo R, Koropatnick J, Renginfo E, Fernández E, Alvárez D, Torres O, et al. Use of the humanized anti-epidermal growth factor receptor monoclonal antibody h-R3 in combination with radiotherapy in the treatment of locally advanced head and neck cancer patients. J Clin Oncol. 2004; 22:1646–54.
26. Crombet T, Torres L, Neninger E, Catalá M, Solano ME, Perera A, Torres O, Iznaga N, Torres F, Pérez R, Lage A, Alvárez D, Torres O, et al. Pharmacological evaluation of humanized anti-epidermal growth factor receptor, monoclonal antibody h-R3, in patients with advanced epithelial-derived cancer. J Immunother. 2003; 26:139–48.
27. Du F, Zheng Z, Shi S, Jiang Z, Qu T, Yuan X, Sun Y, Song Y, Yang L, Zhao J, Wang J, Chi Y. S-1 and cisplatin with or without nimotuzumab for patients with untreated unresectable or metastatic gastric cancer: A randomized, open-label phase 2 trial. Medicine (Baltimore). 2015; 94:e958.
28. Liu ZG, Zhao Y, Tang J, Zhou YJ, Yang WJ, Qiu YF, Wang H. Nimotuzumab combined with concurrent chemoradiotherapy in locally advanced nasopharyngeal carcinoma: a retrospective analysis. Oncotarget. 2016; 7:24429-24435. https://doi.org/10.18632/oncotarget.8225.
29. Zhai RP, Ying HM, Kong FF, Du CR, Huang S, Zhou JJ, Hu CS. Experience with combination of nimotuzumab and intensity-modulated radiotherapy in patients with locoregionally advanced nasopharyngeal carcinoma. Onco Targets Ther. 2015; 8:3383–90.
30. Rodríguez MO, Rivero TC, del Castillo Bahi R, Muchuli CR, Bilbao MA, Vinageras EN, Alert J, Galainena JJ, Rodríguez E, Gracias E, Mulén B, Wilkinson B, de Armas EL, et al. Nimotuzumab plus radiotherapy for unresectable squamous-cell carcinoma of the head and neck. Cancer Biol Ther. 2010; 9:343–49.
31. Ramakrishnan MS, Eswaraiah A, Crombet T, Piedra P, Saurez G, Iyer H, Arvind AS, Arvind AS. Nimotuzumab, a promising therapeutic monoclonal for treatment of tumors of epithelial origin. MAbs. 2009; 1:41–48.
32. Hua YH, Ma SL. FU ZF, Hu QY, Du LB, Jiang H. Effect of nimotuzumab on the radiation sensitivity of nasopharyngeal carcinoma cell line CNE-2. Chin J Zhejiang Med. 2011; 33:836–39.
33. Li HM, Li P, Qian YJ, Wu X, Xie L, Wang F, Zhang H, Liu L. A retrospective paired study: efficacy and toxicity of nimotuzumab versus cisplatin concurrent with radiotherapy in nasopharyngeal carcinoma. BMC Cancer. 2016; 16:946–55.
34. Huang JF, Zhang FZ, Zou QZ, Zhou LY, Yang B, Chu JJ, Yu JH, Zhang HW, Yuan XP, Tai GM, Liu FJ, Ma CC. Induction chemotherapy followed by concurrent chemoradiation and nimotuzumab for locoregionally advanced nasopharyngeal carcinoma: preliminary results from a phase II clinical trial. Oncotarget. 2017; 8:2457-2465. https://doi.org/10.18632/oncotarget.13899.

