Identification of somatic frameshift mutations in exon 9 of CALR in myeloproliferative neoplasms (MPNs) has provided a new molecular diagnostic marker in essential thrombocythemia (ET) and primary myelofibrosis (PMF), where is the second most common alteration after JAK2V617F [1]. There are two main types of CALR mutations and there is evidence about their distinct clinical/prognostic implications [2].
The most frequent mutations accounting for more than 80% of all, are type-1 variant, a 52 bp deletion (p.L367fs*46) and type-2, a 5bp TTGTC insertion (p.K385fs*47). Overall, type-1 is more frequent, but incidence of type-2 is higher in ET compared to PMF. Of the remaining, more than 50 different indels have been identified. First studies in MPNs showed that CALR compared to JAK2 mutants were associated with lower hemoglobin level and leukocyte count, higher platelets and longer overall survival [1]. In ET, further publications demonstrated that patients carrying CALR mutations had lower risk of thrombosis than JAK2/MPL-mutated but there was no association with survival [3, 4]. However, JAK2/CALR/MPL mutational status in PMF is prognostically informative and outcome is better in CALR-mutated and worse in JAK2-positive or triple-negative patients [5, 6].
Recent evidence suggests that favorable outcome might be restricted to type-1 alteration in PMF [2], which may indicate the necessity of different therapeutic approaches. All frameshift mutations reported in the literature result in a +1bp frameshift. Type-1 mutation eliminates almost all negative charged aminoacids of the C-terminal domain whereas type-2 retains approximately half of them [1]. Bioinformatic analyses suggest additional functionally relevant structural differences between type-1 and type-2 mutants [7]. This could explain the mutant type distribution in PMF and ET and also the phenotypic and clinical differences. Mutations other than type-1/2 but resulting in 52bp deletions or 5bp insertions, have been reported. In some cases, they produce the same altered protein but an alternative in others. We, for instance, have identified a 52 bp deletion in ET (Figure 1) that is not the common type-1 since it starts at c.1090 (p.E364fs*49) [8]. It seems reasonable that mutations other that type-1/2 but with the same or similar protein effect should be included in each group in terms of studying clinical associations. Few recent publications have attempted classifying the alternative mutants in type-1-like or type-2-like. A statistical approximation algorithm was applied to obtain a structural protein prediction for each mutant [9]. They classified as type-2- like those mutants with higher α-helix content (more similar to wild-type), and as type-1-like those with significantly lower α-helix content. Survival was shorter in PMF patients with type-2/type-2-like vs type-1/type-1-like mutations, meaning that clinical/prognostic advantages of type-1 are extended to type-1-like. Other study categorized alternative mutants according to the grade of conservation of negatively charged aminoacids divided in three stretches [10]. Thus, type-2/type-2-like conserved the three stretches, type-1/type-1-like conserved one stretch, and other mutants conserved 2 stretches. Type-1-like mutations were mainly associated with PMF and significantly higher risk of myelofibrotic transformation in ET. Type-2-like was preferentially related to ET phenotype, low risk of thrombosis despite very-high platelet counts and indolent clinical course. Also, PMF carrying type-1-like had better survival compared to those with JAK2V617F.
Hence, it seems that mutation characterization is critical to establish groups with specific clinical and prognostic features. There are several publications regarding methods for CALR mutation screening and some authors have suggested that fragment analysis determination may be sufficient for routine diagnostic purposes and even have developed real time PCR detection methods[11]. These screening techniques do not allow a precise characterization and sometimes it is not easy to determine the exact size of the insertion/deletion through fragment analysis. This is an important issue since we have found, as others, in-frame indel polymorphisms that could be misinterpreted as mutations if they are not properly characterized. We found a 9pb deletion at codon c.1177 of CALR in peripheral blood of a patient with polyglobulia and confirmed its germline nature by analyzing buccal swab DNA (Figure 1). We used high resolution melting as screening method because is a closed-tube technique, and its product can be directly used for subsequent sequencing [8]. Fragment analysis has the disadvantage that sequencing has to be performed from a new unlabeled PCR product, but mainly, it cannot discriminate point mutations. Although rare, nonsense mutations implying the loss of variable number of negatively charged amino acids of the C-terminus have been reported (i.e p.E374X, p.E380X, p.K391X) [12]. Besides, SNPs must be distinguished from mutations. We have also found in a patient with thrombocytosis, a nonsynonymous polymorphism, E380G (Figure 1), which has been previously characterized as a mutation [12]. However, we believe it may be most likely a polymorphism since it was a constitutional variant also detected in the oral mucosa and the thrombocytosis was transient.
According to recent studies, the C-terminus of type-1/2 mutants with its characteristic positive electrostatic charge has been shown to allow the association of mutant CALR with thrombopoietin receptor (c-MPL) and activate the JAK2 downstream pathway, whereas wild type and other mutants failed to interact with c-MPL [13, 14]. Therefore, clinical/biological implication of the point and nonsense variants remains to be determined as they may not contribute the same way as frameshift mutations.
On the other hand, either through fragment analysis or HRM as screening methods, we believe that sequencing is required since mutation characterization is essential to determine not only whether the alteration belongs to the clinically relevant types-1 or 2, or to the type-1/2-like but to distinguish polymorphisms from point/nonsense mutations that may be crucial for diagnosis.
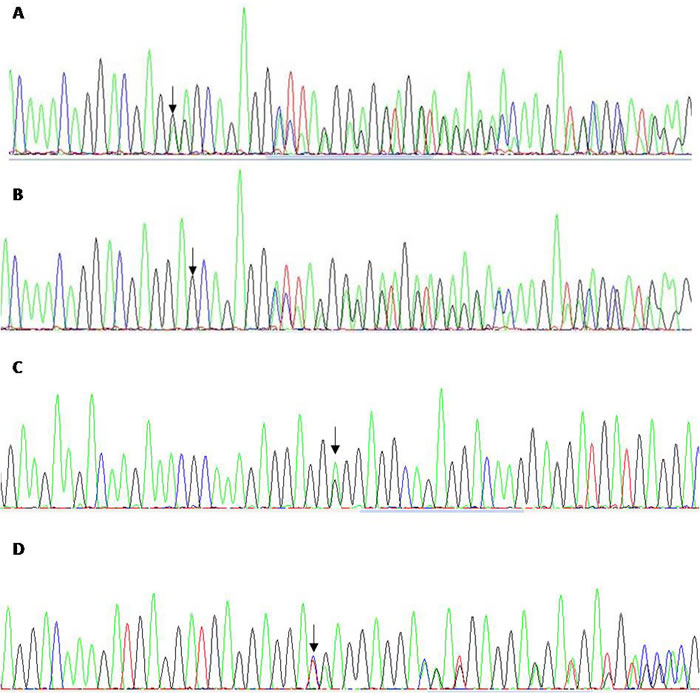
Figure 1: Sanger sequencing of CALR corresponding to a non classical 52 bp deletion c.1090_1141del from a patient with ET (A), the classical type 1 mutation from an ET case (B), a 9bp deletion c. 1177_1186del from oral mucosa of a patient with polyglobulia (C), an E380G variant in oral mucosa from a patient with transient thrombocytosis (D).
Conflicts of Interest
There is no conflict of interest.
Editorial note
This paper has been accepted based in part on peer-review conducted by another journal and the authors’ response and revisions as well as expedited peer-review in Oncotarget.
References
1. Klampfl T, Gisslinger H, Harutyunyan AS, Nivarthi H, Rumi E, Milosevic JD, Them NC, Berg T, Gisslinger B, Pietra D, Chen D, Vladimer GI, Bagienski K, et al. Somatic mutations of calreticulin in myeloproliferative neoplasms. The New England journal of medicine. 2013; 369:2379-2390. doi: 10.1056/NEJMoa1311347.
2. Tefferi A, Lasho TL, Finke C, Belachew AA, Wassie EA, Ketterling RP, Hanson CA and Pardanani A. Type 1 vs type 2 calreticulin mutations in primary myelofibrosis: differences in phenotype and prognostic impact. Leukemia. 2014; 28:1568-1570. doi: 10.1038/leu.2014.83.
3. Rotunno G, Mannarelli C, Guglielmelli P, Pacilli A, Pancrazzi A, Pieri L, Fanelli T, Bosi A and Vannucchi A. Impact of Calreticulin Mutations on Clinical and Hematological Phenotype and Outcome in Essential Thrombocythemia. Blood. 2014; 123:1552-1555. doi: blood-2013-11-538983.
4. Rumi E, Pietra D, Ferretti V, Klampfl T, Harutyunyan AS, Milosevic JD, Them NC, Berg T, Elena C, Casetti IC, Milanesi C, Sant’antonio E, Bellini M, et al. JAK2 or CALR mutation status defines subtypes of essential thrombocythemia with substantially different clinical course and outcomes. Blood. 2014; 123:1544-1551. doi: blood-2013-11-539098.
5. Tefferi A, Guglielmelli P, Larson DR, Finke C, Wassie EA, Pieri L, Gangat N, Fjerza R, Belachew AA, Lasho TL, Ketterling RP, Hanson CA, Rambaldi A, et al. Long-term survival and blast transformation in molecularly annotated essential thrombocythemia, polycythemia vera, and myelofibrosis. Blood. 2014; 124:2507-2513; quiz 2615. doi: 10.1182/blood-2014-05-579136.
6. Rumi E, Pietra D, Pascutto C, Guglielmelli P, Martinez-Trillos A, Casetti I, Colomer D, Pieri L, Pratcorona M, Rotunno G, Sant’Antonio E, Bellini M, Cavalloni C, et al. Clinical effect of driver mutations of JAK2, CALR, or MPL in primary myelofibrosis. Blood. 2014; 124:1062-1069. doi: 10.1182/blood-2014-05-578435.
7. Eder-Azanza L, Navarro D, Aranaz P, Novo FJ, Cross NC and Vizmanos JL. Bioinformatic analyses of CALR mutations in myeloproliferative neoplasms support a role in signaling. Leukemia. 2014; 28:2106-2109. doi: 10.1038/leu.2014.190.
8. Bilbao-Sieyro C, Santana G, Moreno M, Torres L, Santana-Lopez G, Rodriguez-Medina C, Perera M, Bellosillo B, de la Iglesia S, Molero T and Gomez-Casares MT. High resolution melting analysis: a rapid and accurate method to detect CALR mutations. PloS one. 2014; 9:e103511. doi: 10.1371/journal.pone.0103511.
9. Tefferi A, Lasho TL, Tischer A, Wassie EA, Finke CM, Belachew AA, Ketterling RP, Hanson CA and Pardanani AD. The prognostic advantage of calreticulin mutations in myelofibrosis might be confined to type 1 or type 1-like CALR variants. Blood. 2014; 124:2465-2466. doi: 10.1182/blood-2014-07-588426.
10. Pietra D, Rumi E, Ferretti VV, Buduo CA, Milanesi C, Cavalloni C, Sant’Antonio E, Abbonante V, Moccia F, Casetti IC, Bellini M, Renna MC, Roncoroni E, et al. Differential clinical effects of different mutation subtypes in CALR-mutant myeloproliferative neoplasms. Leukemia. 2016; 30:431-438. doi: 10.1038/leu.2015.277.
11. Jones AV, Ward D, Lyon M, Leung W, Callaway A, Chase A, Dent CL, White HE, Drexler HG, Nangalia J, Mattocks C and Cross NC. Evaluation of methods to detect CALR mutations in myeloproliferative neoplasms. Leukemia research. 2015; 39:82-87. doi: 10.1016/j.leukres.2014.11.019.
12. Lim KH, Chang YC, Gon-Shen Chen C, Lin HC, Wang WT, Chiang YH, Cheng HI, Su NW, Lin J, Chang YF, Chang MC, Hsieh RK, Kuo YY, et al. Frequent CALR exon 9 alterations in JAK2 V617F- mutated essential thrombocythemia detected by high-resolution melting analysis. Blood cancer journal. 2015; 5:e295. doi: 10.1038/bcj.2015.21.
13. Araki M, Yang Y, Masubuchi N, Hironaka Y, Takei H, Morishita S, Mizukami Y, Kan S, Shirane S, Edahiro Y, Sunami Y, Ohsaka A and Komatsu N. Activation of the thrombopoietin receptor by mutant calreticulin in CALR-mutant myeloproliferative neoplasms. Blood. 2016; 127:1307-1316. doi: 10.1182/blood-2015-09-671172.
14. Elf S, Abdelfattah NS, Chen E, Perales-Paton J, Rosen EA, Ko A, Peisker F, Florescu N, Giannini S, Wolach O, Morgan EA, Tothova Z, Losman JA, et al. Mutant Calreticulin Requires Both Its Mutant C-terminus and the Thrombopoietin Receptor for Oncogenic Transformation. Cancer discovery. 2016; 6:368-381. doi: 10.1158/2159-8290.cd-15-1434.

