INTRODUCTION
Autoimmune liver diseases (AILD) cover a spectrum of primary biliary cirrhosis (PBC), primary sclerosing cholangitis (PSC), autoimmune hepatitis (AIH) and immunoglobulin G4 (IgG4) related cholangitis. These are all relatively rare diseases but result in significant morbidity and mortality. A considerable proportion of patients with AILD eventually progress to end-stage liver disease. In Europe, AILD represent a major indication for liver transplantation. As complex disorders, AILD develop from the interactions between a variety of genetic and environmental factors [1–3]. Until now, the pathogenesis of PBC, PSC, AIH or IgG4 related cholangitis has not been fully elaborated.
Previous epidemiological studies have reported that the incidence of AILD varies over time and space [4]. It is widely accepted that, in genetically susceptible individuals, environmental risk factors might contribute to the onset of disease [2]. The rapid economical development of society leads to changes in lifestyle, hygienic and psychosocial conditions. The influence of the socioeconomic status on the incidence of AILD has never been studied. Herein, we systematically reviewed epidemiological studies of AILD from all over the world, and explored the relationship between the AILD incidence and the socioeconomic status. In this study, the human development index (HDI) was applied as an indicator to reflect socioeconomic status. We are convinced that this study might provide additional insight into the pathogenesis and etiology of these diseases.
RESULTS
Study characteristics
Among the 43 enrolled studies, 22 reported the incidence of PBC [5–26], while 13 were relevant for PSC [13-14, 17, 27-36], and 14 provided information about epidemiology of AIH [4, 13-14, 17, 37-46]. No studies mentioned the population incidence of IgG4 related cholangitis, presumably because it is relatively rare as a new disease entity.
Primary characteristics of the enrolled studies including first author, publication year, research period, country, continent, criteria of disease identification, incidence (per 100,000 per year) and HDI were summarized in Table 1. A majority of the studies (29 of 42) were conducted in Europe, while six studies were conducted in North America, six and two were conducted in Asia and Australia, respectively.
Table 1: Primary characteristics of the included studies
Study |
Publication year |
Disease |
Disease identification |
Country |
Continent |
Research period |
Incidence per 100,000 per year |
HDI |
|---|---|---|---|---|---|---|---|---|
Triger8 |
1980 |
PBC |
Cholestasis; AMA |
United Kingdom |
Europe |
1977-1979 |
0.58 |
0.735 |
Eriksson9 |
1984 |
PBC |
Cholestasis; AMA |
Sweden |
Europe |
1973-1982 |
1.37 |
0.776 |
Borda10 |
1989 |
PBC |
Cholestasis; AMA |
Spain |
Europe |
1974-1987 |
1974: 0.41 |
1974: NA |
Myszor11 |
1990 |
PBC |
Cholestasis; AMA; liver biopsy |
United Kingdom |
Europe |
1965-1987 |
1987: 1.98 |
1987: 0.768 |
Danielsson12 |
1990 |
PBC |
(Cholestasis + AMA) or liver biopsy |
Sweden |
Europe |
1973-1982 |
1.33 |
0.776 |
Almdal13 |
1991 |
PBC |
Registry-based |
Denmark |
Europe |
1981-1985 |
0.90 |
0.788 |
Remmel14 |
1995 |
PBC |
(Cholestasis + AMA) or liver biopsy |
Estonia |
Europe |
1973-1992 |
0.23 |
0.684 |
Metcalf 15 |
1997 |
PBC |
2 of 3: AMA positive; abnormal liver function; liver biopsy |
United Kingdom |
Europe |
1987-1994 |
2.20 |
0.839 |
Berdal16 |
1998 |
PBC |
Cholestasis; AMA; liver biopsy |
Norway |
Europe |
1985-1994 |
1.20 |
0.843 |
Berdal16 |
1998 |
PSC |
Cholangiography; exclusion of alternatives |
Norway |
Europe |
1985-1994 |
0.70 |
0.843 |
Berdal16 |
1998 |
AIH |
Original IAHG criteria6 |
Norway |
Europe |
1985-1994 |
1.60 |
0.843 |
Boberg17 |
1998 |
PBC |
Cholestasis; AMA; liver biopsy |
Norway |
Europe |
1986-1995 |
1.62 |
0.849 |
Boberg17 |
1998 |
PSC |
Cholestasis; Cholangiography; liver biopsy |
Norway |
Europe |
1986-1995 |
1.31 |
0.849 |
Boberg17 |
1998 |
AIH |
Original IAHG criteria6 |
Norway |
Europe |
1986-1995 |
1.90 |
0.849 |
James18 |
1999 |
PBC |
2 of 3: AMA positive; abnormal liver function; liver biopsy |
United Kingdom |
Europe |
1987-1994 |
1987: 2.30 |
1987: 0.758 |
Kim19 |
2000 |
PBC |
(Cholestasis + AMA) or liver biopsy |
USA |
North America |
1975-1995 |
2.70 |
0.847 |
Whalley20 |
2007 |
PBC |
Cholestasis; AMA |
United Kingdom |
Europe |
2003-2004 |
3.50 |
0.881 |
Whalley20 |
2007 |
PSC |
Cholangiography |
United Kingdom |
Europe |
2003-2004 |
2.00 |
0.881 |
Whalley20 |
2007 |
AIH |
Abnormal liver function; presence of autoantibodies |
United Kingdom |
Europe |
2003-2004 |
3.00 |
0.881 |
Rautiainen21 |
2007 |
PBC |
2 of 3: Cholestasis; AMA positive; liver biopsy |
Finland |
Europe |
1988-1999 |
1988: 1.20 |
1988: 0.784 |
Pla22 |
2007 |
PBC |
2 of 3: Cholestasis; AMA positive; liver biopsy |
Spain |
Europe |
1990-2002 |
1.72 |
0.794 |
Myers23 |
2009 |
PBC |
Cholestasis; AMA |
Canada |
North America |
1996-2002 |
3.03 |
0.868 |
Chong24 |
2010 |
PBC |
2 of 3: Cholestasis; AMA positive; liver biopsy |
Brunei |
Asia |
2007 |
1.03 |
0.841 |
Delgado25 |
2012 |
PBC |
2 of 3: Cholestasis; AMA positive; liver biopsy |
Israel |
Asia |
1990-2010 |
1990-1999: 1.00 |
1990-1999: 0.814 |
Baldursdottir26 |
2012 |
PBC |
2 of 3: Cholestasis; AMA positive; liver biopsy |
Iceland |
Europe |
1991-2010 |
1991-2000: 2.00 |
1991-2000: 0.829 |
Ngu27 |
2012 |
PBC |
2 of 3: Cholestasis; AMA positive; liver biopsy |
New Zealand |
Australia |
2008 |
0.80 |
0.899 |
Koulentaki28 |
2014 |
PBC |
2 of 3: Cholestasis; AMA positive; liver biopsy |
Greece |
Europe |
1990-2010 |
2.09 |
0.803 |
Boonstra29 |
2014 |
PBC |
2 of 3: Cholestasis; AMA positive; liver biopsy |
Netherlands |
Europe |
2000-2007 |
1.10 |
0.885 |
Escorsell30 |
1994 |
PSC |
Cholangiography |
Spain |
Europe |
1984-1988 |
0.04 |
0.733 |
Hurlburt31 |
2002 |
PSC |
Cholangiography |
USA |
North America |
1984-2000 |
0 |
0.861 |
Ang32 |
2002 |
PSC |
Cholangiography; exclusion of alternatives |
Singapore |
Asia |
1989-1998 |
1.33 |
0.767 |
Bambha33 |
2003 |
PSC |
Cholestasis; Cholangiography or liver biopsy; exclusion of alternatives |
USA |
North America |
1976-2000 |
0.90 |
0.854 |
Kingham34 |
2004 |
PSC |
Abnormal liver function; Cholangiography; liver biopsy |
United Kingdom |
Europe |
1984-2003 |
0.91 |
0.813 |
Kaplan35 |
2007 |
PSC |
Abnormal liver function; Cholangiography or liver biopsy; exclusion of alternatives |
Canada |
North America |
2000-2005 |
0.92 |
0.880 |
Card36 |
2008 |
PSC |
Registry-based |
United Kingdom |
Europe |
1990-2001 |
0.41 |
0.876 |
Lindkvist37 |
2010 |
PSC |
Cholestasis; Cholangiography or liver biopsy; exclusion of alternatives |
Sweden |
Europe |
1992-2005 |
1.22 |
0.855 |
Toy38 |
2011 |
PSC |
Cholangiography or liver biopsy |
USA |
North America |
2000-2006 |
0.41 |
0.897 |
Boonstra39 |
2013 |
PSC |
Cholestasis; Cholangiography or liver biopsy; exclusion of alternatives |
Netherlands |
Europe |
2000-2007 |
0.50 |
0.885 |
Ritland40 |
1985 |
AIH |
Abnormal liver function; presence of autoantibodies; exclusion of alternatives |
Norway |
Europe |
1981 |
1.19 |
0.798 |
Tanner41 |
1989 |
AIH |
Abnormal liver function; liver biopsy; exclusion of alternatives |
United Kingdom |
Europe |
1971-1987 |
0.42 |
0.735 |
Lee42 |
2001 |
AIH |
Original IAHG criteria6 |
Singapore |
Asia |
1990-1996 |
0.60 |
0.761 |
Primo43 |
2004 |
AIH |
Original6, revised7, or simplified criteria5 |
Spain |
Europe |
1990-2003 |
0.83 |
0.796 |
Werner44 |
2008 |
AIH |
Revised IAHG criteria7 |
Sweden |
Europe |
1990-2003 |
0.85 |
0.848 |
Primo45 |
2009 |
AIH |
Revised IAHG criteria7 |
Spain |
Europe |
2003 |
1.07 |
0.837 |
Ngu46 |
2010 |
AIH |
Revised7 or simplified criteria5 |
New Zealand |
Austrilia |
2008 |
1.70 |
0.899 |
Delgado4 |
2013 |
AIH |
Simplified criteria5 |
Israel |
Asia |
1995-2010 |
0.67 |
0.849 |
Grønbæk47 |
2014 |
AIH |
Registry-based |
Denmark |
Europe |
1994-2012 |
1.68 |
0.864 |
Van Gerven48 |
2014 |
AIH |
Revised7 or simplified criteria5 |
Netherlands |
Europe |
2000-2010 |
1.10 |
0.889 |
Yoshizawa49 |
2015 |
AIH |
Revised IAHG criteria |
Japan |
Asia |
2004-2014 |
1.52 |
0.882 |
HDI: human development index; PBC: primary biliary cirrhosis; PSC: primary sclerosing cholangitis; AIH: autoimmune hepatitis; AMA: anti-mitochondrial antibodies; IAHG: international autoimmune hepatitis group; NA: not available.
The national incidence of AILD varied among the studies performed in different countries or during different study periods. A relatively higher incidence of disease was associated with a higher national HDI. However, the included studies were generally conducted in countries with higher socioeconomic development. A total of 28 studies were performed in countries with very high HDI, 14 in high HDI countries, and one in medium HDI country. Few studies investigated the incidence of AILD in less developed countries with medium or low HDI.
PBC incidence and HDI
The incidence of PBC was positively correlated with the national HDI according to Pearson correlation and linear regression analysis, but there was no statistical significance [β = 5.582 ± 6.343 (95% CI), r = 0.348, P = 0.082] (Figure 1a, Table 2). We noticed that the incidence of PBC in New Zealand, Australia was particularly low compared to those reported in other locations for a similar period.[24] After removing the study by Ngu et al.,[24] a significantly positive correlation between HDI and PBC incidence was observed [β = 7.645 ± 6.320 (95% CI), r = 0.463, P = 0.020] (Figure 1b).
Table 2: Correlation between AILD incidence and HDI, along with its three dimensions
Disease |
Parameters |
HDI |
Health Index |
Education index |
Income Index |
|---|---|---|---|---|---|
PBC |
R |
0.348 |
0.422 |
-0.650 |
-0.284 |
β |
5.582 |
2.193 |
-2.370 |
-0.131 |
|
95% CI of β |
[-0.761, 1.925] |
[0.159, 4.227] |
[-3.565, -1.175] |
[-0.316, 0.055] |
|
P |
0.082 |
0.036 |
< 0.01 |
0.159 |
|
PSC |
R |
0.116 |
0.180 |
0.235 |
0.599 |
β |
1.355 |
2.605 |
0.761 |
5.285 |
|
95% CI of β |
[-6.346, 9.055] |
[-6.838, 12.049] |
[-1.325, 2.847] |
[0.594, 9.976] |
|
P |
0.706 |
0.556 |
0.439 |
0.031 |
|
AIH |
R |
0.638 |
0.187 |
0.219 |
0.649 |
β |
8.784 |
2.165 |
0.916 |
7.575 |
|
95% CI of β |
[2.116, 15.452] |
[-4.972, 9.302] |
[-1.656, 3.488] |
[1.987, 13.164] |
|
P |
0.014 |
0.521 |
0.453 |
0.012 |
AILD: autoimmune liver disease; HDI: human development index; PBC: primary biliary cirrhosis; PSC: primary sclerosing cholangitis; AIH: autoimmune hepatitis; CI: confidence interval.
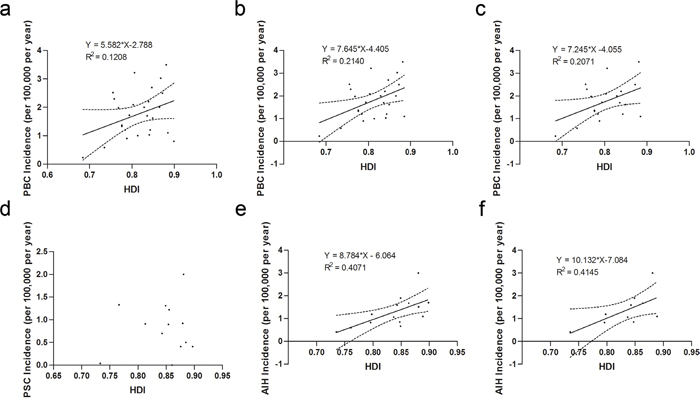
Figure 1: National incidence of autoimmune liver diseases and human development index. a. Overall incidence of PBC (r = 0.348, P = 0.082); b. Incidence of PBC after exclusion of the study conducted in New Zealand (r = 0.463, P = 0.020); c. Incidence of PBC in Europe (r = 0.455, P = 0.044); d. Incidence of PSC (r = 0.116, P = 0.706); e. Overall incidence of AIH (r = 0.638, P= 0.019); f. Incidence of AIH in Europe (r = 0.644, P = 0.045). Best-fit lines (solid) and the 95% confidence band of the best-fit line (dashed) by linear regression are indicated.
In subgroup analysis for geographic location (continent), Figure 1c demonstrated that the PBC incidence in Europe was statistically, positively correlated with the national HDI [β = 7.245 ± 7.021 (95% CI), r = 0.455, P = 0.044]. The relationship between the HDI and PBC incidence in Asia, North America or Australia was impossible to be identified due to the limited number of studies involved.
PSC incidence and HDI
There was no correlation between the PSC incidence and the national HDI (r = 0.116, P = 0.706) (Figure 1d, Table 2). Subsequent subgroup analysis for geographic location (continent) indicated no correlation between the incidence of PSC and HDI in Europe (r = 0.508, P = 0.198) or in North America (r = -0.030, P = 0.970).
AIH incidence and HDI
We found a significantly positive correlation between the national HDI and AIH incidence [β = 8.784 ± 6.668 (95% CI), r = 0.638, P = 0.014] (Figure 1e, Table 2). In Europe, the national incidence of AIH was positively correlated with the HDI [β = 10.132 ± 9.817 (95% CI), r = 0.644, P = 0.045] (Figure 1f). Limited data prevented further analysis about this relationship in other continents.
Disease incidence in countries with different HDIs
Studies investigating the PBC incidence were classified into three groups based on the fact if they were conducted in very high, high or medium HDI countries. ANOVA analysis revealed no significant difference among the groups (P = 0.074) (Figure 2a). Countries with a very high HDIs presented a mean PBC incidence of 1.981 per 100,000 per year (Standard deviation (SD): 0.842), while high HDI countries had a mean PBC incidence of 1.544 per 100,000 per year (SD: 0.641). Similarly, we removed the study conducted in New Zealand, Australia by Ngu et al.,[24] and found that PBC was significantly more prevalent in countries with higher HDIs (P = 0.045 by ANOVA).
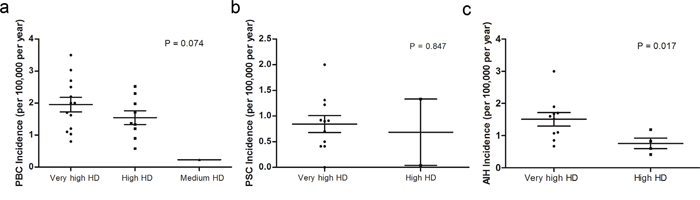
Figure 2: National incidence of autoimmune liver diseases in countries with different development levels. a. Incidence of PBC; b. Incidence of PSC; c. Incidence of AIH. One-way analysis of variance or unpaired t test was conducted in the comparison.
Compared to countries with very high HDIs (mean incidence: 0.844 per 100,000 per year, SD: 0.542), high HDI countries had no difference of PSC incidence (mean incidence: 0.685 per 100,000 per year, SD: 0.912) (P = 0.847 by unpaired t test) (Figure 2b).
Very high HDI countries had a mean AIH incidence of 1.509 per 100,000 per year (SD: 0.662), significantly higher than in countries with high HDIs (mean incidence: 0.760 per 100,000 per year, SD: 0.332) (P = 0.017 by unpaired t test) (Figure 2c).
Disease incidence with three dimensions of HDI
We further evaluated the correlations between the incidence of AILD and the three dimensions of HDI (Table 2). Interestingly, the incidence of PBC was positively correlated with life expectancy at birth (health index) [β = 2.193 ± 2.034 (95% CI), r = 0.422, P = 0.036], but showed a negative correlation with the education index [β = -2.370 ± 1.195 (95% CI), r = -0.650, P < 0.01]. There was a positive correlation between the PSC incidence and the income index [β = 5.285 ± 4.691 (95% CI), r = 0.599, P = 0.031]. In terms of AIH, the incidence also presented a positive correlation with the income index [β = 7.575 ± 5.589 (95% CI), r = 0.649, P = 0.012].
DISCUSSION
This study revealed that socioeconomic development, as indicated by the HDI, might have a positive correlation with the incidence of PBC and AIH. Countries with very high HDI tended to have a higher incidence of PBC and AIH compared to countries with high or medium HDI. In addition, the economic status, as indicated by GNI per capita (income index of HDI), had a positive correlation with the incidence of PSC and AIH. We additionally found some association between national incidence of AILD and the socioeconomic status.
It has been commonly recognized that AILD, mainly consisted of PBC, PSC and AIH, develops as a result from the influence of multiple genes in combination with currently undefined environmental factors. Environmental risk factors might be very complex, but are regarded to trigger the disease onset. PBC is a female predominant liver disease. A controlled interview-based study in the United States revealed that a history of urinary tract infections, cigarette smoking, use of hormone replacement therapies, or frequent use of nail polish were associated with an increased risk for PBC [47]. On the other hand, PSC is a progressive cholestatic liver disease, which is strongly associated with inflammatory bowel disease. A case-control study in the Netherlands has demonstrated that smoking has a protective effect for developing PSC [1]. In terms of AIH, it is mentioned that alcohol drinking and living in a childhood home with wood heating are protective factors against the development of AIH [2]. Other putative environmental factors of AILD include keeping pets, type of housing, number of siblings and family manners. An unidentified agent (i.e., toxin/microbe) might be involved in the development of AILD [3]. Tenca et al. have confirmed that close contact with a pet (especially a cat) during childhood increase the risk of AILD [3]. All these environmental factors as mentioned above might be related to the development of socioeconomic status and subsequent lifestyle changes. Based on this correlation, we made a hypothesis that the incidence of AILD might have a causal relationship with human socioeconomic development.
In this study, a comprehensive review is presented, covering all available relevant studies that report the incidence of AILD without restriction of geographic region or language. On a global level, there was a positive but not significant correlation between PBC incidence and HDI. When excluding the study by Ngu et al conducted in New Zealand [24], whose PBC incidence was especially low compared to other locations in a similar research period, the incidence of PBC demonstrated a positive correlation with HDI. In addition, the PBC incidence in Europe correlated positively with HDI. We found a similar positive correlation in regard to the AIH incidence and the HDI, both worldwide and in Europe. However, we failed to get the similar result in terms of PSC.
A deep analysis on the three dimensions of HDI has been performed. Interestingly, a high GNI per capita had a close association with PSC and AIH prevalence. Furthermore, a higher PBC incidence was related with a higher life expectancy at birth and a lower mean and expected years of schooling. These results summarized in our study might offer clues to the pathogenesis of AILD.
It is the first time a research was conducted, investigating the relationship between the AILD incidence and socioeconomic development. The HDI was selected as the measurement tool because of its worldwide acceptance in international comparisons of development levels. Another strength of this study is that we set up rigorous inclusion criteria, including only population-based studies with definite diagnosis of AILD. Population-based surveys have higher validity because everyone in the at-risk population, or a random sample of the population, is accounted for.
Nevertheless, a few limitations of this study must be taken into consideration. First of all, the review of AILD epidemiology was confined to Europe, North America, Asia and Australia, due to limited data in Africa and Oceania. Secondly, different areas within a country usually have different development levels. However, HDI is the summary of the average socioeconomic status of a country. Moreover, some studies were conducted in a specific region or a single province of a country, which resulted in an uneven distribution of incidence data. Thirdly, we failed to make subgroup analyses according to gender, ethnicity or region (rural/urban gap), on account of the insufficient data. In some way, different populations in an area might have variations in the disease incident rates.
In summary, we have demonstrated a potentially positive relationship between the national incidence of AILD and HDI. This study provides for the first time the evidence that in areas with higher development levels, AILD might be more prevalent, and offers a distinctive perspective on the global epidemiological status of AILD. A more robust and comprehensive analysis is required for further more epidemiological investigations in other continents and based on more detailed information.
MATERIALS AND METHODS
Diagnosis of autoimmune liver diseases
For the purpose of this paper, only studies were included with definite criteria for the diagnosis of autoimmune liver disease. The diagnostic criteria for PBC included: (i) clinical presentation; (ii) elevated serum level of alkaline phosphatase of liver origin for more than 6 months; (iii) presence of serum anti-mitochondrial antibodies (≥1:40); (iv) histological characteristics of florid bile duct lesions. Criteria (ii) and (iii) were diagnostic for PBC, and criteria (iv) confirmed the diagnosis.
The identification of PSC was based on increased serum levels of alkaline phosphatase and γ-glutamyltranspeptidase not otherwise explained, when magnetic resonance cholangiography (MRC) or endoscopic retrograde cholangiography (ERC) demonstrated bile duct changes with multifocal strictures and segmental dilatations. Secondary causes of sclerosing cholangitis and other cholestatic disorders were excluded.
AIH was diagnosed based on the combination of clinical, biochemical (e.g. presence of autoantibodies, elevated immunoglobulin G level) and histological conditions according to the reported criteria [48–50].
Definition and calculation of HDI
The HDI is a compound measure of average achievement in three key dimensions of human development: a long and healthy life (health index: life expectancy at birth), being knowledgeable (education index: mean and expected years of schooling) and having a decent standard of living (income index: gross national income (GNI) per capita).
The HDI data were obtained from the United Nations Development Programme database (http://hdr.undp.org/en/data). The average HDI over the research period was calculated, and was defined as the HDI for each study. We hypothesized that HDI progressed linearly in a short period of time and estimated the missing HDI data based on the available data. According to the 2014 Human Development Report (HDR 2014), quartiles of HDI distribution were defined as follows: very high human development (HDI ≥ 0.800), high human development (0.700 ≤ HDI< 0.800), medium human development (0.550 ≤HDI< 0.700), and low human development (HDI < 0.550).
Search strategy and literature evaluation
Literature was searched using PubMed from inception to January 2016 to identify relevant national epidemiological studies of autoimmune liver disease. No language restriction was imposed. Search terms were as follows: (“Liver Cirrhosis, Biliary/epidemiology”[Mesh] OR “primary biliary cirrhosis” OR “primary biliary cholangitis” OR “Cholangitis, Sclerosing/epidemiology”[Mesh] OR “primary sclerosing cholangitis” OR “primary sclerotic cholangitis” OR “Hepatitis, Autoimmune/epidemiology”[Mesh] OR “autoimmune hepatitis” OR “G4 related cholangitis” OR “G4 associated cholangitis”) AND (prevalence OR incidence OR epidemic OR morbidity).
Only studies that present incidence of PBC, PSC or AIH with a definite diagnosis in an adult population were included. Non population-based surveys were disqualified, such as those only enrolled patients in a particular hospital or participants taking part in a particular health plan.
Two investigators independently completed eligibility evaluation and data extraction. Disagreement was solved by discussion with the third investigator. A total of 1708 records were identified through basic search. 1652 publications were excluded after screening through titles and abstracts. Further eligibility evaluation resulted in the exclusion of nine studies because of the absence of data about HDI or disease incidence, and an additional exclusion of four studies because they were not adult population-based. Finally, a total of 43 surveys were included in this study.
Statistical analysis
All statistical analysis was performed by SPSS 21.0 (IBM, Chicago, IL, USA). Associated data was plotted using GraphPad Prism (6.0, GraphPad Software, Inc., San Diego, CA, USA). Kolmogorov–Smirnoff test was conducted to examine the normal distribution of variables. Correlations between the incidence of AILD and HDI were obtained by Pearson coefficient (with normal distribution); in cases of skewed distributions of variables, the Spearman coefficient was applied. In addition, a linear regression analysis was conducted. One-way analysis of variance (ANOVA) or an unpaired t-test was used to compare disease incidence in groups with different socioeconomic development. A P value of less than 0.05 was considered as statistically significant.
Abbreviations
PBC: primary biliary cirrhosis; PSC: primary sclerosing cholangitis; AIH: autoimmune hepatitis; AILD: autoimmune liver diseases; HDI: human development index; IgG4: immunoglobulin G4; MRC: magnetic resonance cholangiography; ERC: endoscopic retrograde cholangiography; GNI: gross national income; HDR: human development report; IBD: inflammatory bowel disease.
ACKNOWLEDGMENTS
Authors’ contributions: Pan HY, Zou H and Zheng MH designed the study. Zou H, Dai YN and Zheng JN screened studies and extracted data. Zou H and Shi KQ did the statistical analyses. Zheng JN prepared figures. Zou H, Poucke SV, Pan HY and Zheng MH reviewed the results, interpreted data, and wrote the manuscript. All authors saw and approved the final version of the paper.
CONFLICTS OF INTERESTThe authors report no declarations of interest.
FUNDING INFORMATION
This work was supported by grants from National Natural Science Foundation of China (81500665), Zhejiang Engineering Research Center of Intelligent Medicine (2016E10011) and Project of New Century 551 Talent Nurturing in Wenzhou.
REFERENCES
1. Boonstra K, de Vries EM, van Geloven N, van Erpecum KJ, Spanier M, Poen AC, van Nieuwkerk CM, Witteman BJ, Tuynman HA, Naber AH, Kingma PJ, Beuers U, Ponsioen CY, et al. Risk factors for primary sclerosing cholangitis. Liver Int. 2016; 36:84-91.
2. Ngu JH, Gearry RB, Frampton CM, Stedman CA. Autoimmune hepatitis: the role of environmental risk factors: a population-based study. Hepatol Int. 2013; 7:869-875.
3. Tenca A, Farkkila M, Jalanko H, Vapalahti K, Arola J, Jaakkola T, Penagini R, Vapalahti O, Kolho KL. Environmental Risk Factors of Pediatric Onset Primary Sclerosing Cholangitis and Autoimmune Hepatitis. J Pediatr Gastroenterol Nutr. 2015.
4. Delgado JS, Vodonos A, Malnick S, Kriger O, Wilkof-Segev R, Delgado B, Novack V, Rosenthal A, Menachem Y, Melzer E, Fich A. Autoimmune hepatitis in southern Israel: a 15-year multicenter study. J Dig Dis. 2013; 14:611-618.
5. Triger DR. Primary biliary cirrhosis: an epidemiological study. Br Med J. 1980; 281:772-775.
6. Eriksson S, Lindgren S. The prevalence and clinical spectrum of primary biliary cirrhosis in a defined population. Scand J Gastroenterol. 1984; 19:971-976.
7. Borda F, Huarte MP, Zozaya JM, Jimenez C, del Cazo FJ, Lanas A, Tiberio G, Munoz M. Primary biliary cirrhosis in Navarra [Article in Spanish]. An Med Interna. 1989; 6:63-66.
8. Myszor M, James OF. The epidemiology of primary biliary cirrhosis in north-east England: an increasingly common disease? Q J Med. 1990; 75:377-385.
9. Danielsson A, Boqvist L, Uddenfeldt P. Epidemiology of primary biliary cirrhosis in a defined rural population in the northern part of Sweden. Hepatology. 1990; 11:458-464.
10. Almdal TP, Sorensen TI. Incidence of parenchymal liver diseases in Denmark, 1981 to 1985: analysis of hospitalization registry data. The Danish Association for the Study of the Liver. Hepatology. 1991; 13:650-655.
11. Remmel T, Remmel H, Uibo R, Salupere V. Primary biliary cirrhosis in Estonia. With special reference to incidence, prevalence, clinical features, and outcome. Scand J Gastroenterol. 1995; 30:367-371.
12. Metcalf JV, Bhopal RS, Gray J, Howel D, James OF. Incidence and prevalence of primary biliary cirrhosis in the city of Newcastle upon Tyne, England. Int J Epidemiol. 1997; 26:830-836.
13. Berdal JE, Ebbesen J, Rydning A. Incidence and prevalence of autoimmune liver diseases [Article in Norwegian]. Tidsskr Nor Laegeforen. 1998; 118:4517-4519.
14. Boberg KM, Aadland E, Jahnsen J, Raknerud N, Stiris M, Bell H. Incidence and prevalence of primary biliary cirrhosis, primary sclerosing cholangitis, and autoimmune hepatitis in a Norwegian population. Scand J Gastroenterol. 1998; 33:99-103.
15. James OF, Bhopal R, Howel D, Gray J, Burt AD, Metcalf JV. Primary biliary cirrhosis once rare, now common in the United Kingdom? Hepatology. 1999; 30:390-394.
16. Kim WR, Lindor KD, Locke GR, 3rd, Therneau TM, Homburger HA, Batts KP, Yawn BP, Petz JL, Melton LJ, 3rd, Dickson ER. Epidemiology and natural history of primary biliary cirrhosis in a US community. Gastroenterology. 2000; 119:1631-1636.
17. Whalley S, Puvanachandra P, Desai A, Kennedy H. Hepatology outpatient service provision in secondary care: a study of liver disease incidence and resource costs. Clin Med (Lond). 2007; 7:119-124.
18. Rautiainen H, Salomaa V, Niemela S, Karvonen AL, Nurmi H, Isoniemi H, Farkkila M. Prevalence and incidence of primary biliary cirrhosis are increasing in Finland. Scand J Gastroenterol. 2007; 42:1347-1353.
19. Pla X, Vergara M, Gil M, Dalmau B, Cistero B, Bella RM, Real J. Incidence, prevalence and clinical course of primary biliary cirrhosis in a Spanish community. Eur J Gastroenterol Hepatol. 2007; 19:859-864.
20. Myers RP, Shaheen AA, Fong A, Burak KW, Wan A, Swain MG, Hilsden RJ, Sutherland L, Quan H. Epidemiology and natural history of primary biliary cirrhosis in a Canadian health region: a population-based study. Hepatology. 2009; 50:1884-1892.
21. Chong VH, Telisinghe PU, Jalihal A. Primary biliary cirrhosis in Brunei Darussalam. Hepatobiliary Pancreat Dis Int. 2010; 9:622-628.
22. Delgado JS, Vodonos A, Delgado B, Jotkowitz A, Rosenthal A, Fich A, Novack V. Primary biliary cirrhosis in Southern Israel: a 20 year follow up study. Eur J Intern Med. 2012; 23:e193-198.
23. Baldursdottir TR, Bergmann OM, Jonasson JG, Ludviksson BR, Axelsson TA, Bjornsson ES. The epidemiology and natural history of primary biliary cirrhosis: a nationwide population-based study. Eur J Gastroenterol Hepatol. 2012; 24:824-830.
24. Ngu JH, Gearry RB, Wright AJ, Stedman CA. Low incidence and prevalence of primary biliary cirrhosis in Canterbury, New Zealand: a population-based study. Hepatol Int. 2012; 6:796-800.
25. Koulentaki M, Mantaka A, Sifaki-Pistolla D, Thalassinos E, Tzanakis N, Kouroumalis E. Geoepidemiology and space-time analysis of Primary biliary cirrhosis in Crete, Greece. Liver Int. 2014; 34:e200-207.
26. Boonstra K, Kunst AE, Stadhouders PH, Tuynman HA, Poen AC, van Nieuwkerk KM, Witteman EM, Hamann D, Witteman BJ, Beuers U, Ponsioen CY, Epi PSCPBCsg. Rising incidence and prevalence of primary biliary cirrhosis: a large population-based study. Liver Int. 2014; 34:e31-38.
27. Escorsell A, Pares A, Rodes J, Solis-Herruzo JA, Miras M, de la Morena E. Epidemiology of primary sclerosing cholangitis in Spain. Spanish Association for the Study of the Liver. J Hepatol. 1994; 21:787-791.
28. Hurlburt KJ, McMahon BJ, Deubner H, Hsu-Trawinski B, Williams JL, Kowdley KV. Prevalence of autoimmune liver disease in Alaska Natives. Am J Gastroenterol. 2002; 97:2402-2407.
29. Ang TL, Fock KM, Ng TM, Teo EK, Chua TS, Tan JY. Clinical profile of primary sclerosing cholangitis in Singapore. J Gastroenterol Hepatol. 2002; 17:908-913.
30. Bambha K, Kim WR, Talwalkar J, Torgerson H, Benson JT, Therneau TM, Loftus EV, Jr., Yawn BP, Dickson ER, Melton LJ, 3rd. Incidence, clinical spectrum, and outcomes of primary sclerosing cholangitis in a United States community. Gastroenterology. 2003; 125:1364-1369.
31. Kingham JG, Kochar N, Gravenor MB. Incidence, clinical patterns, and outcomes of primary sclerosing cholangitis in South Wales, United Kingdom. Gastroenterology. 2004; 126:1929-1930.
32. Kaplan GG, Laupland KB, Butzner D, Urbanski SJ, Lee SS. The burden of large and small duct primary sclerosing cholangitis in adults and children: a population-based analysis. Am J Gastroenterol. 2007; 102:1042-1049.
33. Card TR, Solaymani-Dodaran M, West J. Incidence and mortality of primary sclerosing cholangitis in the UK: a population-based cohort study. J Hepatol. 2008; 48:939-944.
34. Lindkvist B, Benito de Valle M, Gullberg B, Bjornsson E. Incidence and prevalence of primary sclerosing cholangitis in a defined adult population in Sweden. Hepatology. 2010; 52:571-577.
35. Toy E, Balasubramanian S, Selmi C, Li CS, Bowlus CL. The prevalence, incidence and natural history of primary sclerosing cholangitis in an ethnically diverse population. BMC Gastroenterol. 2011; 11:83.
36. Boonstra K, Weersma RK, van Erpecum KJ, Rauws EA, Spanier BW, Poen AC, van Nieuwkerk KM, Drenth JP, Witteman BJ, Tuynman HA, Naber AH, Kingma PJ, van Buuren HR, et al. Population-based epidemiology, malignancy risk, and outcome of primary sclerosing cholangitis. Hepatology. 2013; 58:2045-2055.
37. Ritland S. The incidence of chronic active hepatitis in Norway. A retrospective study. Scand J Gastroenterol Suppl. 1985; 107:58-60.
38. Tanner AR, Dellipiani AW. Chronic active hepatitis: a sixteen year survey at a district general hospital. Postgrad Med J. 1989; 65:725-728.
39. Lee YM, Teo EK, Ng TM, Khor C, Fock KM. Autoimmune hepatitis in Singapore: a rare syndrome affecting middle-aged women. J Gastroenterol Hepatol. 2001; 16:1384-1389.
40. Primo J, Merino C, Fernandez J, Moles JR, Llorca P, Hinojosa J. [Incidence and prevalence of autoimmune hepatitis in the area of the Hospital de Sagunto (Spain)]. Gastroenterol Hepatol. 2004; 27:239-243.
41. Werner M, Prytz H, Ohlsson B, Almer S, Bjornsson E, Bergquist A, Wallerstedt S, Sandberg-Gertzen H, Hultcrantz R, Sangfelt P, Weiland O, Danielsson A. Epidemiology and the initial presentation of autoimmune hepatitis in Sweden: a nationwide study. Scand J Gastroenterol. 2008; 43:1232-1240.
42. Primo J, Maroto N, Martinez M, Anton MD, Zaragoza A, Giner R, Devesa F, Merino C, del Olmo JA. Incidence of adult form of autoimmune hepatitis in Valencia (Spain). Acta Gastroenterol Belg. 2009; 72:402-406.
43. Ngu JH, Bechly K, Chapman BA, Burt MJ, Barclay ML, Gearry RB, Stedman CA. Population-based epidemiology study of autoimmune hepatitis: a disease of older women? J Gastroenterol Hepatol. 2010; 25:1681-1686.
44. Gronbaek L, Vilstrup H, Jepsen P. Autoimmune hepatitis in Denmark: incidence, prevalence, prognosis, and causes of death. A nationwide registry-based cohort study. J Hepatol. 2014; 60:612-617.
45. Van Gerven NM, Verwer BJ, Witte BI, van Erpecum KJ, van Buuren HR, Maijers I, Visscher AP, Verschuren EC, van Hoek B, Coenraad MJ, Beuers UH, de Man RA, Drenth JP, et al. Epidemiology and clinical characteristics of autoimmune hepatitis in the Netherlands. Scand J Gastroenterol. 2014; 49:1245-1254.
46. Yoshizawa K, Joshita S, Matsumoto A, Umemura T, Tanaka E, Morita S, Maejima T, Ota M. Incidence and prevalence of autoimmune hepatitis in the Ueda area, Japan. Hepatol Res. 2015.
47. Gershwin ME, Selmi C, Worman HJ, Gold EB, Watnik M, Utts J, Lindor KD, Kaplan MM, Vierling JM, Group UPE. Risk factors and comorbidities in primary biliary cirrhosis: a controlled interview-based study of 1032 patients. Hepatology. 2005; 42:1194-1202.
48. Hennes EM, Zeniya M, Czaja AJ, Pares A, Dalekos GN, Krawitt EL, Bittencourt PL, Porta G, Boberg KM, Hofer H, Bianchi FB, Shibata M, Schramm C, et al. Simplified criteria for the diagnosis of autoimmune hepatitis. Hepatology. 2008; 48:169-176.
49. Johnson PJ, McFarlane IG. Meeting report: International Autoimmune Hepatitis Group. Hepatology. 1993; 18:998-1005.
50. Alvarez F, Berg PA, Bianchi FB, Bianchi L, Burroughs AK, Cancado EL, Chapman RW, Cooksley WG, Czaja AJ, Desmet VJ, Donaldson PT, Eddleston AL, Fainboim L, et al. International Autoimmune Hepatitis Group Report: review of criteria for diagnosis of autoimmune hepatitis. J Hepatol. 1999; 31:929-938.

