INTRODUCTION
Diffuse large B-cell lymphoma (DLBCL) is the most common type of non-Hodgkin lymphoma (NHL) accounting for approximately 30-40% of newly diagnosed NHL cases [1]. It is a group of highly heterogeneous diseases with variable clinical features and molecular genetic alterations [2]. DLBCL can be classified as two subtypes including germinal center B-cell like (GCB) and activated B-cell like (ABC) DLBCL according to gene expression profiling [3]. Otherwise, DLBCL can be also classified as GCB, ABC and primary mediastinal B-cell lymphoma (PMBL). ABC and PMBL subgroups are grouped as non-GCB DLBCL. Since the addition of the rituximab (R) to cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP), the prognosis of DLBCL has been greatly improved [4]. However, about 30~40% DLBCL patients still couldn’t benefit from R-CHOP and eventually develop relapsed/refractory disease [5]. Hence, further studies are needed to investigate the underlying molecular mechanism of DLBCL and to develop novel therapeutic approaches for this disease.
Programmed death ligand 1 (PD-L1, also known as B7-H1/CD274), a member of the B7 family, is an important ligand of programmed death 1 (PD-1, also known as CD279), which is an immune inhibitory receptor expressed on the surface of T cells, B cells and monocyte upon activation [6]. Recently, PD-L1 was reported to overexpress in different tumors including lymphoma, melanoma, breast cancer, ovarian cancer and bladder cancer [7–11]. Studies also found PD-1/PD-L1 engagement was able to negatively regulate immune response and involved in T cell exhaustion in tumor microenvironment, which promoted tumor progression and metastasis [12–15]. Blockade of PD-1 and PD-L1 has shown to have a therapeutic potential prospect in relapsed/refractory lymphoma and other advanced cancers [16, 17], suggesting that anti-PD-1 or anti–PD-L1 antibodies may be a novel and effective therapeutic approach for lymphoma and other cancers.
Interaction between PD-1 and PD-L1 leads to the suppression of T-cell function and further facilitates immune escape of tumor cells. However, apart from evading host immunity, little is known about the intracellular signal transduction in tumor cell after PD-L1 binding to PD-1. PD-L1 is a type I transmembrane protein with 290 amino acids, consisting of immunoglobulin V-like and C like domains, a hydrophobic transmembrane domain, and a cytoplasmic tail domain [18]. Several studies reported that PD-L2, another ligand of PD-1, directly activated dendritic cell (DC) and functioned as a receptor for signal delivered by cells expressing PD-L2 [19, 20]. PD-L1 and PD-L2 share 34% identity, suggesting they may have similar functions [21]. Meanwhile, it has been reported that PD-L1 appears to be a monomer in solution, but two PD-L1 molecules are present in the asymmetric unit [22, 23], suggesting that it is possible that PD-L1 appears to be a dimer on cell membrane, but monomer in cytoplasm. If a dimer of PD-L1 appears on cell membrane, it is very complex but is indeed possible that a part of PD-L1 could bind to extracellular PD-1, which leads to the suppression of T-cell function, and another PD-L1 could directly activate the intracellular oncogenic signaling pathways. Recently, a very interest study reported that melanoma cell-intrinsic PD-1 could promote tumor growth [24]. This further suggests that a part of the dimer PD-L1 on cell membrane could directly bind to intrinsic PD-1, and then promote the tumor growth. Therefore, we hypothesized that PD-L1 binding to PD-1 could directly activate the intracellular oncogenic signaling pathways in tumor cells. Three oncogenic pathways have been reported in DLBCL, including the constitutively activated NF-kB pathway [25], JAK/signal transducer and activator of transcription (STAT), and AKT/mTOR pathways. These oncogenic pathways usually promote cell proliferation and recede apoptosis [26–28]. Based on these premises, we evaluated whether PD-L1 expression was correlated with phosphorylated AKT (p-AKT) expression and overall survival in DLBCL in this study, and then investigated whether PD-1/PD-L1 binding could directly activate intracellular AKT/mTOR pathway in tumor cells. We found that nearly half DLBCL cases had either PD-L1 or p-AKT overexpression compared to normal lymph nodes, and PD-L1 expression was correlated with p-AKT expression. Co-expression of PD-L1 and p-AKT indicated the worst survival compared to single positive and both negative expression of them. Interestingly, we found that PD-1/PD-L1 binding could directly activate the intracellular AKT/mTOR signaling, not only in T cells, but also in DLBCL tumor cells.
RESULTS
Clinical patient characteristics
In this retrospective study, due to lack of tumor tissue or clinical data of some cases, only 100 DLBCL patients between Jan 2008 and Dec 2011 in our hospital were evaluable. Clinical characteristics of the patients were summarized in Table 1. Of the 100 studied patients, there were 60 men and 40 women. The median age was 59 years (ranging from 17 to 85). Forty patients (40%) were diagnosed as GCB-DLBCL and 60 patients (60%) were diagnosed as non-GCB-DLBCL according to the 2008 WHO classification. Thirty-eight patients (38%) were classified as clinical stages I-II and 62 patients (62%) were classified as clinical stages III-IV. Sixty-nine patients (69%) were IPI scores of 0-2 and 31 patients (31%) were IPI scores of 3-5. Thirty-nine patients (39%) were treated with R-CHOP regimen and 61 patients (61%) were treated with CHOP/CHOPE regimen.
Table 1: Association of PD-L1 and p-AKT expression with the clinical characteristics of DLBCL
Clinical Parameters |
n |
PD-L1 expression |
p-AKT expression |
||||||
|---|---|---|---|---|---|---|---|---|---|
Negative (%) |
Positive (%) |
χ2 |
P value |
Negative (%) |
Positive (%) |
χ2 |
P value |
||
Total |
100 |
46(46) |
54(54) |
52(52) |
48(48) |
||||
Gander |
|||||||||
male |
60 |
25(41.7) |
35(58.3) |
1.134 |
0.312 |
29(48.3) |
31(51.7) |
0.808 |
0.418 |
female |
40 |
21(52.5) |
19(47.5) |
23(57.5) |
17(48.3) |
||||
Age (years) |
|||||||||
<60 |
52 |
25(48.1) |
27(51.9) |
0.188 |
0.692 |
33(63.5) |
19(36.5) |
5.702 |
0.027* |
≥60 |
48 |
21(43.8) |
27(56.3) |
19(39.6) |
29(60.4) |
||||
Pathological pattern |
|||||||||
GCB |
40 |
24(60.0) |
16(40.0) |
5.260 |
0.026* |
21(52.5) |
19(47.5) |
0.007 |
1.000 |
non-GCB |
60 |
22(36.7) |
38(63.3) |
31(51.7) |
29(48.3) |
||||
Clinical stages |
|||||||||
I~II |
38 |
19(50.0) |
19(50.0) |
0.395 |
0.543 |
21(55.3) |
17(44.7) |
0.261 |
0.682 |
III~IV |
62 |
27(43.5) |
35(56.5) |
31(50.0) |
31(50.0) |
||||
IPI grades |
|||||||||
0~2 |
69 |
36(52.2) |
33(47.8) |
3.416 |
0.084 |
39(56.5) |
30(43.5) |
1.823 |
0.200 |
3~5 |
31 |
10(32.3) |
21(67.7) |
13(41.9) |
18(58.1) |
||||
Chemotherapy regimens |
|||||||||
RCHOP |
39 |
19(48.7) |
20(51.3) |
0.190 |
0.686 |
21(53.8) |
18(46.2) |
0.087 |
0.839 |
CHOP/CHOPE |
61 |
27(44.3) |
34(55.7) |
31(50.8) |
30(49.2) |
||||
*P<0.05.
The correlation of PD-L1 and p-AKT expression with clinicopathological features
Positive PD-L1 expression was found in 54 DLBCL cases (54%) by IHC. Representative IHC staining patterns of negative and positive PD-L1 expression were given in Figure 1A–1B. Positive p-AKT expression was observed in 48 DLBCL cases (48%), which was shown in Figure 1D, and representative negative case was also shown in Figure 1C. Co-expression of PD-L1 and p-AKT were observed in thirty-two patients (32%), and thirty patients (30%) showed neither PD-L1 nor p-AKT expression. Twenty-two patients (22%) were positive for PD-L1 expression as well as negative for p-AKT expression. Sixteen patients (16%) were negative for PD-L1 expression as well as positive for p-AKT expression (Table 2).
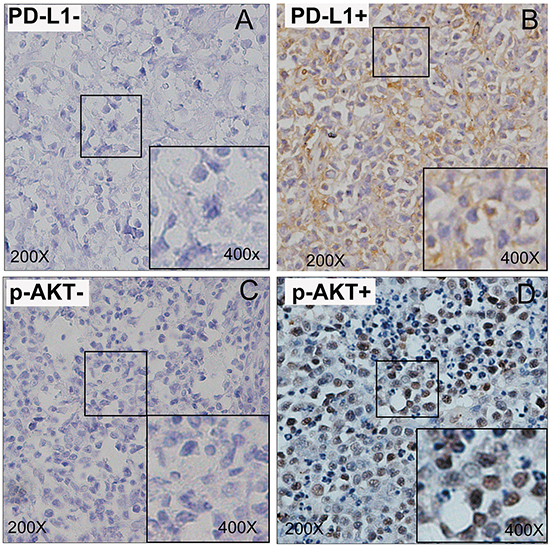
Figure 1: Immunohistochemical staining of DLBCL tumour tissues for PD-L1 and p-AKT expression. A. Representative patterns of negative PD-L1 expression. B. Representative patterns of positive PD-L1 expression. C. Representative patterns of negative p-AKT expression. D. Representative patterns of positive p-AKT expression.
Table 2: The correlation between PD-L1 and p-AKT expression
PD-L1 |
Spearman R |
χ2 |
P value |
|||
|---|---|---|---|---|---|---|
negative |
positive |
|||||
p-AKT |
negative |
30 |
22 |
0.244 |
5.962 |
0.017* |
positive |
16 |
32 |
||||
*P<0.05.
We also found that positive PD-L1 expression was significantly associated with pathological subtype (χ2=5.260; P=0.026, Table 1) and positive p-AKT expression was significantly associated with older age ≥60 years (χ2=5.702; P=0.027, Table 1). However, there were no significant difference among other clinical characteristics between positive and negative group for PD-L1 or p-AKT expression (P>0.05, Table 1). Meanwhile, we also found that PD-L1 expression was correlated with p-AKT expression (R=0.244, χ2=5.962; P=0.017, Table 2).
The influence of PD-L1 and p-AKT expression on DLBCL patient prognosis
Median follow-up duration was 52.4 (ranging from 1.5 to 89.1) months. All of the 100 patients were available for the 3-year overall survival analysis, however only 72 patients could be done for the 5-year overall survival analysis. The results revealed that 3-year and 5-year overall survival rates were 73% and 59.2%, respectively. Clinically, some DLBCL patients were only treated with CHOP/CHOPE. But other DLBCL patients were treated with standard R-CHOP. Considering the influence of different therapy schemes on DLBCL patient prognosis, we separately analyzed 61 patients who adopted CHOP/CHOPE regiment and 39 patients who adopted R-CHOP regiment. Kaplan-Meier survival curves of 61 patients who adopted CHOP/CHOPE regiment showed that DLBCL patients with either positive PD-L1 or p-AKT expression corresponded with a significantly shorter 3 years OS (P=0.018, P=0.033, Figure 2A and 2B) and 5 years OS (P=0.012, P=0.028, Figure 2D and 2E) compared to patients with negative PD-L1 or p-AKT expression. Moreover, DLBCL patients with co-expression of PD-L1 and p-AKT had the worst 5 years OS (P=0.030, Figure 2F) compared to patients with single positive or both negative expression of PD-L1 and p-AKT, but not 3 years OS (P=0.056, Figure 2C). But DLBCL patients with co-expression of PD-L1 and p-AKT had poorer 3 years OS (P=0.018) and 5 years OS (P=0.007) compared to patients with both negative expression of PD-L1 and p-AKT (Table 3).
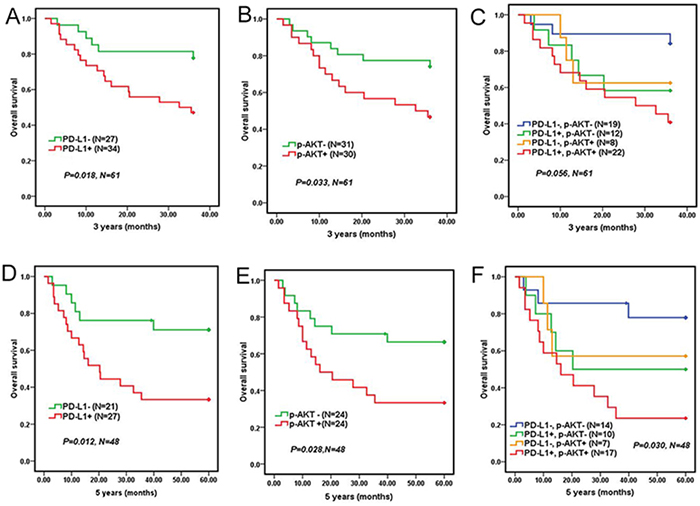
Figure 2: Overall survival of 61 DLBCL patients who adopted CHOP/CHOPE regiment according to PD-L1 and p-AKT expression. 3-year overall survival of DLBCL patients with PD-L1 expression A. p-AKT expression B. and co-expression of PD-L1 and p-AKT expression C. 5-year overall survival of DLBCL patients with PD-L1 expression D. p-AKT expression E. and co-expression of PD-L1 and p-AKT F.
Table 3: Correlations between PD-L1, p-AKT protein expression with prognosis of DLBCL patients treated with CHOP/CHOPE
Expression |
3 years OS |
5 years OS |
||||||
|---|---|---|---|---|---|---|---|---|
Survival rate |
Median OS (months) |
χ2 |
P value |
Survival rate |
Median OS (months) |
χ2 |
P value |
|
PD-L1 |
||||||||
negative |
77.8% |
31.02 |
5.630 |
0.018* |
71.4% |
46.86 |
6.287 |
0.012* |
positive |
47.1% |
24.17 |
33.3% |
29.10 |
||||
p-AKT |
||||||||
negative |
74.2% |
30.11 |
4.540 |
0.033* |
66.7% |
44.50 |
4.427 |
0.028* |
positive |
46.7% |
24.20 |
33.3% |
29.25 |
||||
Co-expression of PD-L1 and p-AKT |
||||||||
negative |
71.8% |
29.43 |
5.586 |
0.018* |
64.5% |
43.31 |
7.378 |
0.007* |
positive |
40.9% |
23.25 |
23.5% |
25.15 |
||||
*P<0.05; OS, Overall survival.
Kaplan-Meier survival curves of 39 patients who adopted R-CHOP regiment showed that DLBCL patients with positive PD-L1 expression had a significantly shorter 3 years OS (P=0.028, Figure 3A), but not 5 years OS (P=0.061, Figure 3D), compared to patients with negative PD-L1 expression. However, DLBCL patients with positive p-AKT expression had a significantly shorter 5 years OS (P=0.023, Figure 3E), but not 3 years OS (P=0. 0.051, Figure 3B), compared to patients with negative p-AKT expression. Moreover, DLBCL patients with co-expression of PD-L1 and p-AKT had the worst 3 years OS (P=0.005, Figure 3C) and 5 years OS (P=0.008, Figure 3F) compared to patients with single positive or both negative expression of PD-L1 and p-AKT. But DLBCL patients with co-expression of PD-L1 and p-AKT had poorer 3 years OS (P=0.002) and 5 years OS (P=0.014) compared to patients with both negative expression of PD-L1 and p-AKT (Table 4). Taken together, these results suggested that the co-expression of PD-L1 and p-AKT was associated with worse prognosis in DLBCL patients.
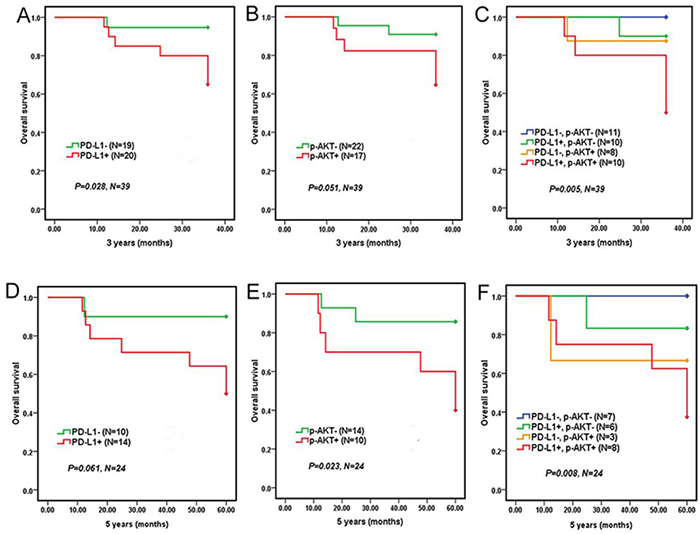
Figure 3: Overall survival of 39 DLBCL patients who adopted R-CHOP regiment according to PD-L1 and p-AKT expression. 3-year overall survival of DLBCL patients with PD-L1 expression A. p-AKT expression B. and co-expression of PD-L1 and p-AKT expression C. 5-year overall survival of DLBCL patients with PD-L1 expression D. p-AKT expression E. and co-expression of PD-L1 and p-AKT F.
Table 4: Correlations between PD-L1, p-AKT protein expression with prognosis of DLBCL patients treated with R-CHOP
Expression |
3 years OS |
5 years OS |
||||||
|---|---|---|---|---|---|---|---|---|
Survival rate |
Median OS (months) |
χ2 |
P value |
Survival rate |
Median OS (months) |
χ2 |
P value |
|
PD-L1 |
||||||||
negative |
94.70% |
34.75 |
4.849 |
0.028* |
87.50% |
55.23 |
3.514 |
0.061 |
positive |
80.00% |
31.97 |
64.30% |
46.50 |
||||
p-AKT |
||||||||
negative |
90.90% |
34.43 |
3.804 |
0.051 |
84.60% |
54.11 |
5.133 |
0.023* |
positive |
82.40% |
31.88 |
55.60% |
44.58 |
||||
Co-expression of PD-L1 and p-AKT |
||||||||
negative |
93.10% |
34.80 |
9.183 |
0.002* |
87.50% |
54.82 |
6.007 |
0.014* |
positive |
50.00% |
31.38 |
37.50% |
46.69 |
||||
*P<0.05; OS, Overall survival.
Subgroup analyses were performed according to gender, age, pathological pattern, clinical stages, IPI scores and chemotherapy regimens, PD-L1 expression, p-AKT expression and co-expression of PD-L1 and p-AKT. The results of univariate and multivariate cox analysis were summarized in Table 5. Univariate Kaplan–Meier estimates demonstrated that age (χ2= 5.963; P=0.015), pathological pattern (χ2=4.823; P=0.028), clinical stages (χ2=9.470; P=0.002), IPI scores (χ2=7.645; P=0.006), chemotherapy regimens (χ2=5.825; P=0.016), PD-L1 expression (χ2=8.945; P=0.003), p-AKT expression (χ2=9.246; P=0.002), co-expression of PD-L1 and p-AKT (χ2=13.992; P<0.001) were associated with poor prognosis in DLBCL patients. To determine the prognostic value of PD-L1 and p-AKT expression, multivariate cox regression models for comparison with prognostic factors were applied. We found that clinical stages [HR (95%CI)=3.726 (1.273–10.902), P=0.016], chemotherapy regimens [HR (95%CI) =3.564 (1.378–9.217), P=0.009], PD-L1 expression [HR(95%CI)=4.740(1.097–20.477), P=0.037] and p-AKT expression [HR(95%CI)=6.205 (1.244–30.949), P=0.026] were the independent prognostic factors negatively impacting survival.
Table 5: Univariate and multivariate analysis of prognostic factors in DLBCL
Clinical Parameters |
Univariate analysis |
Multivariate analysis |
||
|---|---|---|---|---|
χ2 |
P value |
HR(95%CI) |
P value |
|
Gander |
||||
Male vs female |
0.085 |
0.77 |
0.564(0.250-1.271) |
0.167 |
Age(years) |
||||
<60 vs ≥60 |
5.963 |
0.015* |
1.726(0.661-4.510) |
0.265 |
Pathological pattern |
||||
GCB vs non-GCB |
4.823 |
0.028* |
2.392(0.959-5.967) |
0.062 |
Clinical stages |
||||
I~II vs III~IV |
9.47 |
0.002* |
3.726(1.273-10.902) |
0.016* |
IPI grades |
||||
0~2 vs 3~5 |
7.645 |
0.006* |
0.730(0.269-1.980) |
0.536 |
Chemotherapy regimens |
||||
RCHOP vs CHOP/CHOPE |
5.825 |
0.016* |
3.564(1.378-9.217) |
0.009* |
PD-L1 expression |
||||
Negative vs positive |
8.945 |
0.003* |
4.740(1.097-20.477) |
0.037* |
p-AKT expression |
||||
Negative vs positive |
9.246 |
0.002* |
6.205(1.244-30.949) |
0.026* |
Co-expression of PD-L1 and p-AKT |
||||
Negative vs positive |
13.992 |
<0.001** |
0.279(0.041-1.884) |
0.190 |
*P<0.05, **P<0.001; CI, confidence interval; HR, hazard ratio.
In short, PD-L1 expression was correlated with p-AKT, and the co-expression of PD-L1 and p-AKT would result in a poorer prognosis compared with single positive or both negative expression of PD-L1 and p-AKT in DLBCL. Even PD-L1 and p-AKT were the two independent prognostic factors negatively impacting survival.
PD-L1 and mPD-L1 expression in DLBCL cell lines
We selected five human DLBCL cell lines to determine the total PD-L1 expression by western blot and mPD-L1 expression by flow cytometry. The results indicated that all of the five DLBCL cell lines expressed PD-L1 (Figure 4A) and mPD-L1 (Figure 4B).
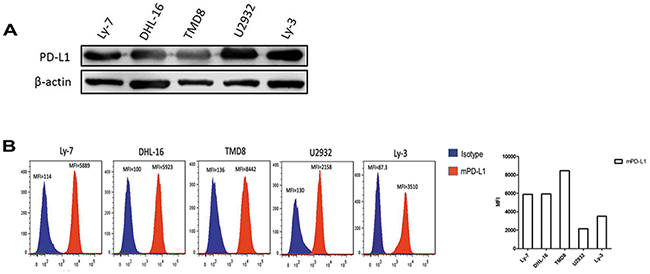
Figure 4: PD-L1 and mPD-L1 expressed widely in DLBCL cell lines. A. Total PD-L1 protein expression in DLBCL cell lines detected by western blot. B. mPD-L1 expression in DLBCL cell lines detected by flow cytometry.
PD-1/PD-L1 binding directly activates the intracellular AKT/mTOR signaling in DLBCL cells
To further determine whether PD-1/PD-L1 binding could directly activate the intracellular AKT/mTOR signaling in tumor cells, DLBCL cell lines were treated with human recombinant PD1/Fc for 24h and 48h. Total and phosphorylated AKT expressions were evaluated by western blot. Results revealed that p-AKT level was significantly up-regulated in three DLBLC cell lines including DHL-16, U2932 and Ly-3, suggesting that the intracellular AKT/mTOR pathway in DLBCL cells was activated (Figure 5). Taken together, we found that intracellular AKT/mTOR signaling could be directly activated by PD-1/PD-L1 binding in DLBCL cells. It revealed that the combination of PD-1/PD-L1 antibodies and AKT/mTOR inhibitor might be a promising and novel therapeutic approach for DLBCL in the future.
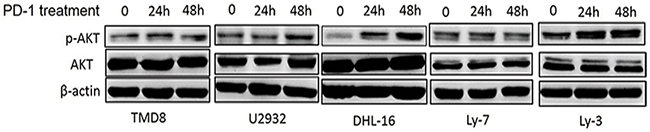
Figure 5: PD-1/PD-L1 binding directly activates the intracellular AKT/mTOR oncogene signaling in DLBCL cells.
DISCUSSION
With the advent of rituximab, the OS of DLBCL patients has been significantly improved. However, still 30~40% DLBCL patients inevitably develop into relapsed/refractory disease. So further studies are needed to investigate the underlying mechanism and develop novel therapeutic approaches for DLBCL. Recent studies have highlighted the role of PD-1/PD-L1 pathway in negatively regulating host antitumor response. As the major ligand of PD-1, PD-L1 is widely expressed and correlated with poor prognosis in many human cancers, including melanoma [29], lung cancer [30], glioblastoma [31], breast cancer [7, 32], Wilms’ tumor [33], urothelial cancer [34], pancreatic cancers [35], esophagus adenocarcinoma [36], kidney tumors [37] as well as hematopoietic malignancies [38, 39]. Kiyasu et al have also demonstrated that PD-L1 expression was associated with poor overall survival in DLBCL patients (P =0.0323) [39], which was consistent with our results in this study. In our study, we showed that positive PD-L1 expression was associated with poor survival of DLBCL patients for 3-years and 5-years OS (P<0.05). Therefore, PD-1 or PD-L1 blockage might be a novel therapeutic approach for DLBCL and other tumors. Several clinical trials carried out in the past two years had revealed that both anti-PD-1 antibodies (such as Nivolumab, Pidilizumab, and Pembrolizumab) and anti PD-L1 antibodies (such as MPDL3280A) had shown significant antitumor effects in patients with metastatic melanoma [40], Hodgkin’s lymphoma [16], bladder cancer [41], and lung cancer [42].
DLBCL tumors have several important oncogenic signaling pathways which make DLBCL to be a heterogeneous disease and impact overall survival of DLBCL patients. The AKT/mTOR signaling pathway has been demonstrated to be constitutively activated in DLBCL [28], and AKT plays a central role in signaling transduction. Activated AKT participates in multiple downstream pathways to promote the malignant phenotype of cancer cells through mediating various pro-survival signals [43–46]. As an important downstream target of AKT, mTOR plays a key role in cell cycle progression and metabolism [47]. Xu et al found that activation of AKT/mTOR pathway was related to poor outcome in DLBCL patients treated with CHOP but not R-CHOP [48]. In our study, we found that activation of AKT/mTOR pathway was related to poor survival in DLBCL patients treated with CHOP/CHOPE for 3-years and 5-years OS (P=0.033, P=0.028), and R-CHOP for 5-years OS (P=0.023), but not R-CHOP for 3-years OS (P=0.051).
In our study, spearman test showed that PD-L1 expression was correlated with p-AKT expression in DLBCL(R=0.244, χ2=5.962; P=0.017). In addition, we found that the DLBCL patients who co-expressed PD-L1 and p-AKT had the worst clinical outcome compared with the patients who were single positive or both negative expression of PD-L1 and p-AKT for 3-years and 5-years OS (P<0.05). So we hypothesized that PD-1/PD-L1 binding might directly activate the intracellular AKT/mTOR oncogenic signaling in tumor cells to promote DLBCL progression. To confirm this hypothesis, we selected five DLBCL cell lines, which overexpressed PD-L1 protein and mPD-L1, to be stimulated with human recombinant PD-1/Fc protein for 24h and 48h. Interestingly, we found that level of p-AKT protein was significantly up-regulated with a time-dependent manner, suggesting that PD-1/PD-L1 binding could directly activate the intracellular AKT/mTOR oncogenic signaling in DLBCL tumor cells. Otherwise, Parsa et al found that expression of the gene encoding PD-L1 increased after loss of PTEN gene and activation of PI3K pathway in human glioma [49]. Lastwika et al found that activation of AKT/mTOR oncogenic pathway promoted immune escape by driving the expression of PD-L1 in NSCLC [50]. Taken together, it was possible that there was a positive feedback loop between PD-1/PD-L1 axis and AKT/mTOR oncogenic signaling.
Our results indicated that the combination of PD-1/PD-L1 antibodies and AKT/mTOR inhibitors might be a promising and novel therapeutic approach for DLBCL in the future. In addition, multivariate analysis in this study showed that expression of PD-L1 or p-AKT was the dependent prognostic factor for DLBCL patients. We also found that PD-L1 expression was related to the pathological subtype, but p-AKT expression was correlated with ages. The reasons for this observed distinction between them were unclear. The numbers of patients included in our study was relatively small, and so these results required further validation in a large cohort. But it showed a consistent trend that DLBCL patients with co-expression of p-AKT and PD-L1 had worse prognosis compared to patients with single positive or both negative expression of PD-L1 and p-AKT, who were treated with either R-CHOP or CHOP/CHOPE. These results suggested that co-expression of PD-L1 and p-AKT was still noteworthy in the rituximab era, and rituximab could not overcome poor prognosis of co-expression of PD-L1 and p-AKT in DLBCL.
In summary, DLBCL patients overexpressed PD-L1 and p-AKT, and co-expression of them showed a significantly worse survival compared to single positive or both negative expression of them. PD-1/PD-L1 binding might activate the intracellular AKT/mTOR oncogenic signaling pathway in tumor cells to promote DLBCL aggressiveness. Thus, a more effective treatment approaches should be developed for this subset of DLBCL patients, and the combination of targeting AKT/mTOR and PD-1/PD-L1 pathway blockade might be a promising therapeutic strategy.
MATERIALS AND METHODS
Patients and samples
A total of 100 DLBCL cases with formalin-fixed paraffin-embedded (FFPE) tissues in the Tianjin Medical University Cancer Institute and Hospital (TMUCTH, Tianjin, China) from Jan 2008 and Dec 2011 were studied. Archived FFPE tumor tissues were obtained from our Department of Pathology and these cases were reclassified according to the 2008 WHO classification and Hans algorithm by experienced hematopathologists. In addition, 10 specimens of normal lymph gland tissue obtained from patients with reactive hyperplasia of lymph node were used as normal controls. All clinical information was obtained by reviewing the patients’ medical charts. The study and all protocols below were approved by the Ethics Committee of TMUCTH.
Immunohistochemistry
IHC staining for PD-L1 and p-AKT proteins were performed using the streptavidin–peroxidase method (SP method). Briefly, the paraffin-fixed slides were dewaxed in xylene and rehydrated through graded alcohols. Antigen retrieval was respectively carried out using EDTA buffer (pH 8.0) for anti-PD-L1 and citric acid buffer (pH 6.0) for anti-phospho-AKT (Ser473) in 120°C for 2 minutes and 30 seconds. Endogenous peroxidase activity was blocked using 0.3% hydrogen peroxide for 10 minutes at room temperature in dark place. Nonspecific binding of the primary antibody was blocked by incubating the slides with 10% normal horse serum for 30 minutes at 37°C. Then they were incubated with the primary antibodies including rabbit anti-PD-L1 polyclonal antibody (1:200, ab153991, Abcam, Cambridge, UK) and rabbit anti-phospho-AKT (Ser473) polyclonal antibody (1:100, AF0908, Affinity Biosciences, USA) at 4°C overnight. And then they were incubated with secondary anti-rabbit IgG/HRP at 37°C for 30 minutes. Subsequently, for visualisation of the antigen, the sections were performed with the chromagen 3, 3′-diaminobenzidine. The slides were counterstained with hematoxylin and mounted under coverslips.
Evaluation of IHC for PD-L1 and p-AKT proteins
Percentages of PD-L1 positive tumor cells and staining intensity were evaluated for each slide. Staining for PD-L1 was considered high expression, if ≥5% of the tumor cell population showed 2+ or 3+ membrane staining. In addition, if ≥20% of the total tissue cellularity showed 2+ or 3+ membrane or cytoplasmic staining in malignant and/or nonmalignant cells, it was considered to have a microenvironment positive for PD-L1 [51]. p-AKT expression was semiquantitatively assessed based on the staining intensity and the proportion of the stained tumor nuclei cells as follows: staining proportion was also classified as 0–3 (0 = 0–5 %, positive cells, 1 = 5–10 % positive cells, 2 = 10–50 %, 3 = ≥50 %) and the intensity of p-AKT staining was scored as 0-3 grades (0 = negative, 1 = weak, 2 = moderate, and 3 = strong). Only when the score reached 3–9, it represented positive. This scoring system was similar to previous studies [52, 53]. Two independent observers evaluated the expression levels of PD-L1 and p-AKT protein following the evaluation system and both observers reexamined the immunostained slides to determine a consensus score.
Cell culture
The DLBCL cell lines: TMD8, U2932, SUDHL-16 were cultured in RPMI-1640 medium (Life Technologies, California, USA) containing 10% fetal bovine serum (Hyclone, UT, USA). OCI-LY3 (LY3) and OCI-LY7 (LY7) were cultured in IMDM medium (Life Technologies, California, USA) supplemented with 15% fetal bovine serum (Hyclone, UT, USA). All medium were supplemented with 1% penicillin-streptomycin and all cells were incubated at 37°C in 5% CO2.
Flow cytometric analysis
For flow cytometry, DLBCL cell lines were harvested, washed, and then labeled with fluorochrome-conjugated PE anti-Human CD274 (PD-L1, B7-H1) (clone 29E.2A3, BioLegend, USA) for 30 minutes at 4°C in dark place. Then the mPD-L1in all samples was measured by flow cytometry (LSDFortessa, BD Bioscience). Results were analyzed with FlowJo software (version 7.6).
Stimulation of DLBCL-cell lines with human recombinant PD-1/FC
All five cell lines were cultured in complete medium containing 100ug/ml human recombinant PD1/Fc (10377-H03H, Sino Biological Inc., Beijing, China) for 24h and 48h. And then total proteins were isolated and run using western Blot to detect the total AKT and p-AKT expression.
Western blot analysis
Cells were harvested and suspended in RIPA lysis buffer containing 1 mM phenylmethylsulfonyl fluoride (PMSF). 20-50μg total protein (depending on different proteins) were separated by sodiumdodecyl sulfate–polyacrylamide (SDS–PAGE) gel electrophoresis and then transferred to polyvinylidene difluoride membranes (PVDF, Roche, UK), which were then blocked in 5% non-fat milk in Tris-buffer saline-Tween (TBST) for 1 h. The immunoblotting was performed by incubation with the primary antibodies including PD-L1 (Abcam, Cambridge, UK), p-AKT and total-AKT (Affinity Biosciences, USA), and β-actin (Cell Signaling Technology, Boston, USA), which was used as an endogenous protein for normalization at 4°C overnight. Blots were then washed and incubated with a 1:3000 dilution of Goat anti-Rabbit IgG H&L (HRP)-conjugated secondary (Millipore, Billerica, MA, USA). Signals were detected by enhanced chemiluminescence Plus reagents (Amersham Pharmacia, Piscataway, NJ) and formed images by Chemiluminescence Imaging System. Signal quantification was obtained using Quantity One software (Bio-Rad Laboratories, USA) and normalized to β-actin.
Statistical analysis
Clinical, pathological, and chromosomal charac- teristics of the patients were compared using chi-square tests or Fisher’s exact tests. The Kaplan-Meier method was used to estimate the over survival (OS) distributions, and the log-rank test was performed to compare the survival difference. Univariate analysis were performed with log-rank test. Multivariate-adjusted Cox regression models were used to evaluate independent prognostic factors. Difference was considered significant when the P value was <0.05 and all reported P values were two sided. These statistical analyses were performed with SPSS 17.0 statistical software (Chicago, IL, USA).
ACKNOWLEDGMENTS AND GRANT SUPPORT
This study was supported by the National Clinical Research Center for Cancer Foundation in Tianjin Medical University Cancer Institute and Hospital (B type, 5-2-18), Natural Science Foundation of China (81402945), National Major Scientific and Technological Special Project for “Significant New Drugs Development” during the Twelfth Five-year Plan Period (2013ZX09303001), Scientific Research Foundation for the Returned Overseas Chinese Scholars in Tianjin (2015-31) and Natural Science Foundation of Tianjin Medical University (2015KYZM14).
CONFLICTs OF INTEREST
The authors declared no conflicts of interest.
REFERENCES
1. Cultrera JL and Dalia SM. Diffuse large B-cell lymphoma: current strategies and future directions. Cancer Control. 2012; 19:204-213.
2. Campo E, Swerdlow SH, Harris NL, Pileri S, Stein H and Jaffe ES. The 2008 WHO classification of lymphoid neoplasms and beyond: evolving concepts and practical applications. Blood. 2011; 117:5019-5032.
3. Alizadeh AA, Eisen MB, Davis RE, Ma C, Lossos IS, Rosenwald A, Boldrick JC, Sabet H, Tran T, Yu X, Powell JI, Yang L, Marti GE, et al. Distinct types of diffuse large B-cell lymphoma identified by gene expression profiling. Nature. 2000; 403:503-511.
4. Coiffier B, Lepage E, Briere J, Herbrecht R, Tilly H, Bouabdallah R, Morel P, Van Den Neste E, Salles G, Gaulard P, Reyes F, Lederlin P and Gisselbrecht C. CHOP chemotherapy plus rituximab compared with CHOP alone in elderly patients with diffuse large-B-cell lymphoma. N Engl J Med. 2002; 346:235-242.
5. Friedberg JW. Relapsed/refractory diffuse large B-cell lymphoma. Hematology Am Soc Hematol Educ Program. 2011; 2011:498-505.
6. Keir ME, Butte MJ, Freeman GJ and Sharpe AH. PD-1 and its ligands in tolerance and immunity. Annu Rev Immunol. 2008; 26:677-704.
7. Qin T, Zeng YD, Qin G, Xu F, Lu JB, Fang WF, Xue C, Zhan JH, Zhang XK, Zheng QF, Peng RJ, Yuan ZY, Zhang L, et al. High PD-L1 expression was associated with poor prognosis in 870 Chinese patients with breast cancer. Oncotarget. 2015; 6:33972-33981. doi: 10.18632/oncotarget.5583.
8. Ahmadzadeh M, Johnson LA, Heemskerk B, Wunderlich JR, Dudley ME, White DE and Rosenberg SA. Tumor antigen-specific CD8 T cells infiltrating the tumor express high levels of PD-1 and are functionally impaired. Blood. 2009; 114:1537-1544.
9. Sun S, Fei X, Mao Y, Wang X, Garfield DH, Huang O, Wang J, Yuan F, Sun L, Yu Q, Jin X, Wang J and Shen K. PD-1(+) immune cell infiltration inversely correlates with survival of operable breast cancer patients. Cancer Immunol Immunother. 2014; 63:395-406.
10. Matsuzaki J, Gnjatic S, Mhawech-Fauceglia P, Beck A, Miller A, Tsuji T, Eppolito C, Qian F, Lele S, Shrikant P, Old LJ and Odunsi K. Tumor-infiltrating NY-ESO-1-specific CD8+ T cells are negatively regulated by LAG-3 and PD-1 in human ovarian cancer. Proc Natl Acad Sci U S A. 2010; 107:7875-7880.
11. Inman BA, Sebo TJ, Frigola X, Dong H, Bergstralh EJ, Frank I, Fradet Y, Lacombe L and Kwon ED. PD-L1 (B7-H1) expression by urothelial carcinoma of the bladder and BCG-induced granulomata: associations with localized stage progression. Cancer. 2007; 109:1499-1505.
12. Drake CG, Jaffee E and Pardoll DM. Mechanisms of immune evasion by tumors. Adv Immunol. 2006; 90:51-81.
13. Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer. 2012; 12:252-264.
14. Dong H, Strome SE, Salomao DR, Tamura H, Hirano F, Flies DB, Roche PC, Lu J, Zhu G, Tamada K, Lennon VA, Celis E and Chen L. Tumor-associated B7-H1 promotes T-cell apoptosis: a potential mechanism of immune evasion. Nat Med. 2002; 8:793-800.
15. Zou W and Chen L. Inhibitory B7-family molecules in the tumour microenvironment. Nat Rev Immunol. 2008; 8:467-477.
16. Ansell SM, Lesokhin AM, Borrello I, Halwani A, Scott EC, Gutierrez M, Schuster SJ, Millenson MM, Cattry D, Freeman GJ, Rodig SJ, Chapuy B, Ligon AH, et al. PD-1 blockade with nivolumab in relapsed or refractory Hodgkin’s lymphoma. N Engl J Med. 2015; 372:311-319.
17. Brahmer JR, Tykodi SS, Chow LQ, Hwu WJ, Topalian SL, Hwu P, Drake CG, Camacho LH, Kauh J, Odunsi K, Pitot HC, Hamid O, Bhatia S, et al. Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med. 2012; 366:2455-2465.
18. Dong H, Zhu G, Tamada K and Chen L. B7-H1, a third member of the B7 family, co-stimulates T-cell proliferation and interleukin-10 secretion. Nat Med. 1999; 5:1365-1369.
19. Nguyen LT, Radhakrishnan S, Ciric B, Tamada K, Shin T, Pardoll DM, Chen L, Rodriguez M and Pease LR. Cross-linking the B7 family molecule B7-DC directly activates immune functions of dendritic cells. J Exp Med. 2002; 196:1393-1398.
20. Radhakrishnan S, Nguyen LT, Ciric B, Ure DR, Zhou B, Tamada K, Dong H, Tseng SY, Shin T, Pardoll DM, Chen L, Kyle RA, Rodriguez M, et al. Naturally occurring human IgM antibody that binds B7-DC and potentiates T cell stimulation by dendritic cells. J Immunol. 2003; 170:1830-1838.
21. Lazar-Molnar E, Yan Q, Cao E, Ramagopal U, Nathenson SG and Almo SC. Crystal structure of the complex between programmed death-1 (PD-1) and its ligand PD-L2. Proc Natl Acad Sci U S A. 2008; 105:10483-10488.
22. Lin DY, Tanaka Y, Iwasaki M, Gittis AG, Su HP, Mikami B, Okazaki T, Honjo T, Minato N and Garboczi DN. The PD-1/PD-L1 complex resembles the antigen-binding Fv domains of antibodies and T cell receptors. Proc Natl Acad Sci U S A. 2008; 105:3011-3016.
23. Chen Y, Liu P, Gao F, Cheng H, Qi J and Gao GF. A dimeric structure of PD-L1: functional units or evolutionary relics? Protein Cell. 2010; 1:153-160.
24. Kleffel S, Posch C, Barthel SR, Mueller H, Schlapbach C, Guenova E, Elco CP, Lee N, Juneja VR, Zhan Q, Lian CG, Thomi R, Hoetzenecker W, et al. Melanoma Cell-Intrinsic PD-1 Receptor Functions Promote Tumor Growth. Cell. 2015; 162:1242-1256.
25. Compagno M, Lim WK, Grunn A, Nandula SV, Brahmachary M, Shen Q, Bertoni F, Ponzoni M, Scandurra M, Califano A, Bhagat G, Chadburn A, Dalla-Favera R, et al. Mutations of multiple genes cause deregulation of NF-kappaB in diffuse large B-cell lymphoma. Nature. 2009; 459:717-721.
26. Ding BB, Yu JJ, Yu RY, Mendez LM, Shaknovich R, Zhang Y, Cattoretti G and Ye BH. Constitutively activated STAT3 promotes cell proliferation and survival in the activated B-cell subtype of diffuse large B-cell lymphomas. Blood. 2008; 111:1515-1523.
27. Pfeifer M, Grau M, Lenze D, Wenzel SS, Wolf A, Wollert-Wulf B, Dietze K, Nogai H, Storek B, Madle H, Dorken B, Janz M, Dirnhofer S, et al. PTEN loss defines a PI3K/AKT pathway-dependent germinal center subtype of diffuse large B-cell lymphoma. Proc Natl Acad Sci U S A. 2013; 110:12420-12425.
28. Uddin S, Hussain AR, Siraj AK, Manogaran PS, Al-Jomah NA, Moorji A, Atizado V, Al-Dayel F, Belgaumi A, El-Solh H, Ezzat A, Bavi P and Al-Kuraya KS. Role of phosphatidylinositol 3’-kinase/AKT pathway in diffuse large B-cell lymphoma survival. Blood. 2006; 108:4178-4186.
29. Oba J, Nakahara T, Abe T, Hagihara A, Moroi Y and Furue M. Expression of programmed death receptor ligand 1 in melanoma may indicate tumor progression and poor patient survival. J Am Acad Dermatol. 2014; 70:954-956.
30. Chen YB, Mu CY and Huang JA. Clinical significance of programmed death-1 ligand-1 expression in patients with non-small cell lung cancer: a 5-year-follow-up study. Tumori. 2012; 98:751-755.
31. Nduom EK, Wei J, Yaghi NK, Huang N, Kong LY, Gabrusiewicz K, Ling X, Zhou S, Ivan C, Chen JQ, Burks JK, Fuller GN, Calin GA, et al. PD-L1 expression and prognostic impact in glioblastoma. Neuro Oncol. 2015; 18:195-205.
32. Ghebeh H, Mohammed S, Al-Omair A, Qattan A, Lehe C, Al-Qudaihi G, Elkum N, Alshabanah M, Bin Amer S, Tulbah A, Ajarim D, Al-Tweigeri T and Dermime S. The B7-H1 (PD-L1) T lymphocyte-inhibitory molecule is expressed in breast cancer patients with infiltrating ductal carcinoma: correlation with important high-risk prognostic factors. Neoplasia. 2006; 8:190-198.
33. Routh JC, Ashley RA, Sebo TJ, Lohse CM, Husmann DA, Kramer SA and Kwon ED. B7-H1 expression in Wilms tumor: correlation with tumor biology and disease recurrence. J Urol. 2008; 179:1954-1959; discussion 1959-1960.
34. Nakanishi J, Wada Y, Matsumoto K, Azuma M, Kikuchi K and Ueda S. Overexpression of B7-H1 (PD-L1) significantly associates with tumor grade and postoperative prognosis in human urothelial cancers. Cancer Immunol Immunother. 2007; 56:1173-1182.
35. Nomi T, Sho M, Akahori T, Hamada K, Kubo A, Kanehiro H, Nakamura S, Enomoto K, Yagita H, Azuma M and Nakajima Y. Clinical significance and therapeutic potential of the programmed death-1 ligand/programmed death-1 pathway in human pancreatic cancer. Clin Cancer Res. 2007; 13:2151-2157.
36. Ohigashi Y, Sho M, Yamada Y, Tsurui Y, Hamada K, Ikeda N, Mizuno T, Yoriki R, Kashizuka H, Yane K, Tsushima F, Otsuki N, Yagita H, et al. Clinical significance of programmed death-1 ligand-1 and programmed death-1 ligand-2 expression in human esophageal cancer. Clin Cancer Res. 2005; 11:2947-2953.
37. Thompson RH, Dong H and Kwon ED. Implications of B7-H1 expression in clear cell carcinoma of the kidney for prognostication and therapy. Clin Cancer Res. 2007; 13:709s-715s.
38. Paydas S, Bagir E, Seydaoglu G, Ercolak V, Ergin M. Programmed death-1 (PD-1), programmed death-ligand 1 (PD-L1), and EBV-encoded RNA (EBER) expression in Hodgkin lymphoma. Ann Hematol. 2015; 94:1545-1552.
39. Kiyasu J, Miyoshi H, Hirata A, Arakawa F, Ichikawa A, Niino D, Sugita Y, Yufu Y, Choi I, Abe Y, Uike N, Nagafuji K, Okamura T, et al. Expression of programmed cell death ligand 1 is associated with poor overall survival in patients with diffuse large B-cell lymphoma. Blood. 2015; 126:2193-2201.
40. Topalian SL, Sznol M, McDermott DF, Kluger HM, Carvajal RD, Sharfman WH, Brahmer JR, Lawrence DP, Atkins MB, Powderly JD, Leming PD, Lipson EJ, Puzanov I, et al. Survival, durable tumor remission, and long-term safety in patients with advanced melanoma receiving nivolumab. J Clin Oncol. 2014; 32:1020-1030.
41. Powles T, Eder JP, Fine GD, Braiteh FS, Loriot Y, Cruz C, Bellmunt J, Burris HA, Petrylak DP, Teng SL, Shen X, Boyd Z, Hegde PS, et al. MPDL3280A (anti-PD-L1) treatment leads to clinical activity in metastatic bladder cancer. Nature. 2014; 515:558-562.
42. Carbognin L, Pilotto S, Milella M, Vaccaro V, Brunelli M, Calio A, Cuppone F, Sperduti I, Giannarelli D, Chilosi M, Bronte V, Scarpa A, Bria E, et al. Differential Activity of Nivolumab, Pembrolizumab and MPDL3280A according to the Tumor Expression of Programmed Death-Ligand-1 (PD-L1): Sensitivity Analysis of Trials in Melanoma, Lung and Genitourinary Cancers. PLoS One. 2015; 10:e0130142.
43. Wendel HG, De Stanchina E, Fridman JS, Malina A, Ray S, Kogan S, Cordon-Cardo C, Pelletier J and Lowe SW. Survival signalling by Akt and eIF4E in oncogenesis and cancer therapy. Nature. 2004; 428:332-337.
44. Altomare DA and Testa JR. Perturbations of the AKT signaling pathway in human cancer. Oncogene. 2005; 24:7455-7464.
45. Davies MA. Regulation, role, and targeting of Akt in cancer. J Clin Oncol. 2011; 29:4715-4717.
46. Courtney KD, Corcoran RB and Engelman JA. The PI3K pathway as drug target in human cancer. J Clin Oncol. 2010; 28:1075-1083.
47. Chang F, Lee JT, Navolanic PM, Steelman LS, Shelton JG, Blalock WL, Franklin RA and McCubrey JA. Involvement of PI3K/Akt pathway in cell cycle progression, apoptosis, and neoplastic transformation: a target for cancer chemotherapy. Leukemia. 2003; 17:590-603.
48. Xu ZZ, Xia ZG, Wang AH, Wang WF, Liu ZY, Chen LY and Li JM. Activation of the PI3K/AKT/mTOR pathway in diffuse large B cell lymphoma: clinical significance and inhibitory effect of rituximab. Ann Hematol. 2013; 92:1351-1358.
49. Lastwika KJ, Wilson W, 3rd, Li QK, Norris J, Xu H, Ghazarian SR, Kitagawa H, Kawabata S, Taube JM, Yao S, Liu LN, Gills JJ and Dennis PA. Control of PD-L1 Expression by Oncogenic Activation of the AKT-mTOR Pathway in Non-Small Cell Lung Cancer. Cancer Res. 2016; 76:227-238.
50. Parsa AT, Waldron JS, Panner A, Crane CA, Parney IF, Barry JJ, Cachola KE, Murray JC, Tihan T, Jensen MC, Mischel PS, Stokoe D and Pieper RO. Loss of tumor suppressor PTEN function increases B7-H1 expression and immunoresistance in glioma. Nat Med. 2007; 13:84-88.
51. Chen BJ, Chapuy B, Ouyang J, Sun HH, Roemer MG, Xu ML, Yu H, Fletcher CD, Freeman GJ, Shipp MA and Rodig SJ. PD-L1 expression is characteristic of a subset of aggressive B-cell lymphomas and virus-associated malignancies. Clin Cancer Res. 2013; 19:3462-3473.
52. David O, Jett J, LeBeau H, Dy G, Hughes J, Friedman M and Brody AR. Phospho-Akt overexpression in non-small cell lung cancer confers significant stage-independent survival disadvantage. Clin Cancer Res. 2004; 10:6865-6871.
53. Pirker R, Pereira JR, von Pawel J, Krzakowski M, Ramlau R, Park K, de Marinis F, Eberhardt WE, Paz-Ares L, Storkel S, Schumacher KM, von Heydebreck A, Celik I, et al. EGFR expression as a predictor of survival for first-line chemotherapy plus cetuximab in patients with advanced non-small-cell lung cancer: analysis of data from the phase 3 FLEX study. Lancet Oncol. 2012; 13:33-42.

