INTRODUCTION
Prostate cancer being the most common cancer and second leading cause of death among men in the Western world [1] is under constant surveillance by researchers and medical personnel worldwide. Despite the efforts, prostate cancer tends to be highly aggressive and can lead to significant mortality and morbidity [2]. It is of utmost importance to devise new methods aiming for earlier diagnosis and optimum individualized therapy of prostate cancer.
Among the ongoing advancements for the treatment of prostate cancer the possibilities involving Prostate specific Membrane Antigen (PSMA) have gained momentum. In the light of published data it can be deduced that radioligand therapy (RLT) with 177Lu-PSMA is effective and has a low toxicity profile [3]. It is also observed that up to 30% of patients do not show and prostate specific antigen (PSA) decline in response to RLT [3, 4]. Therefore, establishment of pre-therapeutic biomarkers for patient selection for RLT would be helpful to avoid over-treatment.
However, there is a continuous strive for establishment of pre therapeutic parameters in order to have an earliest possible assessment to therapy response, which can in turn guide towards redesigning or modifications in treatment course, thus directly affecting the patient survival. It can also help in selection of patient groups that can have maximum benefit from therapy. So far, such biomarkers are not available. Only low platelet counts and permanent use of an analgesic medication for bone pain are negative predictors of therapy response [5]. In contrast, pre-therapeutic tracer uptake as determined by visual assessment or SUV-measurement does not predict therapy response.
In the recent years, tumor textural analysis (a measurement of spatial heterogeneity) as acquired through PET scans is becoming increasingly important for extracting useful information concerning response prediction. PET having the ability for physiological imaging can provide in-depth information about cell metabolism, perfusion, cell proliferation, morphology, tumor viability and receptor density [6]. All these factors can contribute towards tumor heterogeneity and can in turn predict the therapy response. In most cases, these parameters have been used for assessment between pre and post therapy PET scans. For example, several tumors including sarcoma [7], head and neck tumors [8], esophageal carcinoma [9], NSCLC [10], rectal carcinoma [11] have been analyzed this way. However, this information can be even more beneficial if acquired as early as possible in the course of therapy. Different attempts have been made to acquire relevant data in the earlier treatment stages and even from the pre-therapeutic diagnostic scans and/or clinical parameters [12]. Most of these efforts have been made utilizing the anatomical imaging such as MR imaging or CT. However, no large amount of data is available highlighting the use of baseline PET scans as response predictors or therapy planners with particular emphasis on the role of textural heterogeneity parameters in prostate cancer for patients undergoing PSMA therapy. A study which elaborated the predictive role of textural features to predict outcome from base line PET scan showed significant results in cervix and head and neck cancers [13] and one other predicting survival in sarcoma patients [7]. Combination of latest advancements like therapy with PSMA-ligand labels with 177Lu and analysis of tumor textural heterogeneity may have a potential to provide first-rate information. Especially as recent studies found a non-responder rate of about 30% (no PSA decline) after radiopeptide therapy with 177Lu-PSMA [5, 14–16].
The objective of this current study was hence to assess the predictive ability of tumor textural heterogeneity parameters from baseline 68Ga-PSMA PET scan. Selected textural heterogeneity parameters had been previously widely used in different studies and showed a significant potential for depicting the outcome [9–11, 17, 18]. The predictive value of these parameters was compared to established clinical parameters (PSA, serum and bone alkaline phosphate, Eastern Cooperative Oncology Group (ECOG) criterion).
RESULTS
Seventy patients were evaluated in this study. Decrease in PSA level was observed in 42/70 patients (60%) and they were labeled as responders to therapy. Increase in PSA level was seen in 28/70 patients (40%) considered as non-responders (Figure 1A).
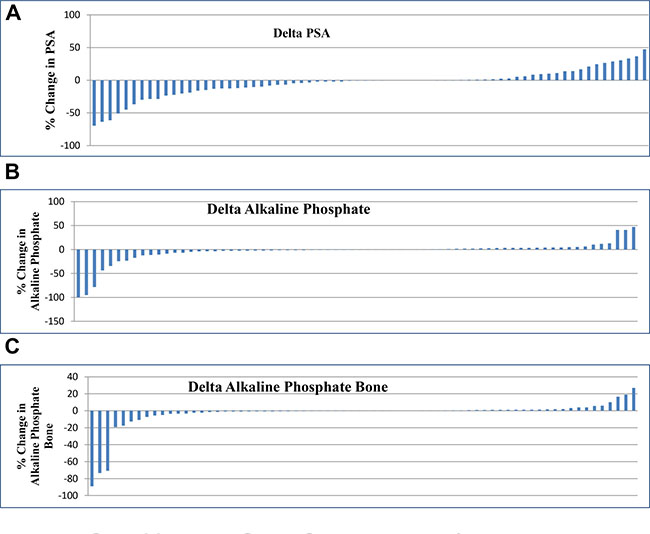
Figure 1: (A) Percentage change in PSA. (B) Percentage change in Alkaline Phosphate. (C) Percentage change in Alkaline Phosphate Bone.
41/70 patients (58%) showed response via decrease in serum alkaline phosphate level (Figure 1B) and 39/70 patients (55%) showed response by decrease in bone specific alkaline phosphate (Figure 1C). Among the responders 24/70 patients (34.2%) showed decrease in both PSA and alkaline phosphate levels at the same time while 22/70 patients (31.42%) showed decrease in PSA, alkaline phosphate and bone specific alkaline phosphate levels together. No change was observed in ECOG of any patient.
Analysis of PET based heterogeneity parameters revealed that only two textural heterogeneity parameters entropy and homogeneity showed correlation with change in pre and post therapy PSA levels. Textural heterogeneity parameters which showed correlation with PSA were derived from bone lesions. Parameters obtained from lymph node and other lesions did not show any correlation with any of correlating clinical parameters. Change in pre and post therapy values of serum alkaline phosphate, bone specific alkaline phosphate and individual patient ECOG status derived from all types of lesions remained uncorrelated. Similarly textural heterogeneity parameters other than entropy and homogeneity also remained uncorrelated. Actual values of correlating parameters as obtained through Spearman correlation are as under.
Entropy showed a negative correlation (rs = −0.327 and p = 0.006) and homogeneity showed a positive correlation (rs = 0.315 and p = 0.008) with change in pre and post therapy PSA levels (Figure 2A and 2B). It is essential to be taken into account that change in PSA levels was obtained as post therapy levels minus the pre therapy level (post therapy PSA–pre therapy PSA). As described in methods a negative value of this equation meant that post therapy PSA was less than that of pre therapy and the case was considered as of a responder. So the resultant value of a responder was negative and vice versa. Hence, a negative correlation of entropy with this change (also represented with a negative value) meant that entropy and change in PSA levels was directly proportional to each other. Or in other words the responders showed a higher entropy value. Similarly, homogeneity showed a positive correlation and hence a negative proportionality with the change in PSA levels signifying that the responders had a lower homogeneity.
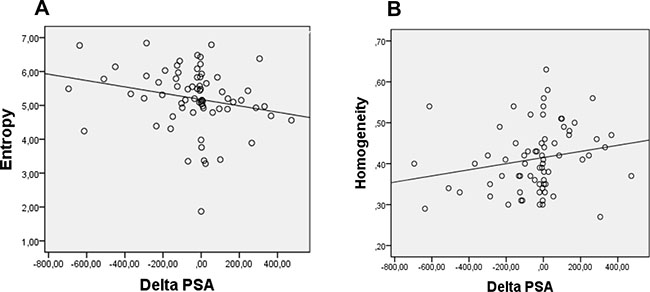
Figure 2: (A) Representation of negative correlation between absolute ΔPSA(ng/ml) and entropy of bone lesions (R2 = 0.283). (B) Representation of positive correlation between absolute ΔPSA (ng/ml) and homogeneity of bone lesions (R2 = 0.326).
Table 1 summarizes the positive results i.e. obtained by correlating positive textural heterogeneity parameters obtained from bone lesions with change in pre and post therapy PSA levels. Rest of the parameters are also given for comparison. It can be also seen that SUV values also did not positively correlate.
Table 1: Correlation of bone lesion derived PET parameters with change in PSA level
PET parameter |
Correlating clinical parameter |
Spearman coefficient |
p-value |
|---|---|---|---|
Entropy |
ΔPSA |
0.327 |
0.006 |
Homogeneity |
ΔPSA |
–0.315 |
0.008 |
COV |
ΔPSA |
0.113 |
0.516 |
Contrast |
ΔPSA |
0.257 |
0.136 |
Size Variation |
ΔPSA |
–0.309 |
0.071 |
SUV(mean) |
ΔPSA |
0.168 |
0.333 |
The ROC analysis also showed that entropy and homogeneity are statistically significant (p < 0.05) for predictive ability of pre-therapeutic PET. Further results of ROC analysis are summarized in the Table 2.
Table 2: Results of ROC analysis for predictive value of pre therapeutic PET-CT
Parameter |
AUC |
95% Confidence interval |
Cut-off value |
|---|---|---|---|
Entropy |
0.695 |
0.57 to 0.799 |
>5.15 |
Homogeneity |
0.683 |
0.56 to 0.789 |
≤0.43 |
Sensitivity and specificity was also assessed for both parameters through ROC (Figure 3A and 3B) and these values were used to find out positive and negative predictive values (Table 3).
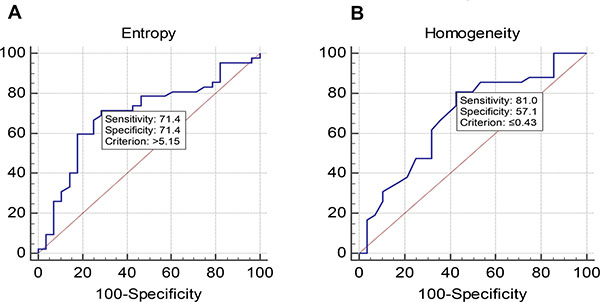
Figure 3: (A) and (B) Showing results of ROC analysis.
Table 3: Outcomes of positive parameters
Parameter |
Sensitivity |
Specificity |
Positive predictive value |
Negative predictive value |
|---|---|---|---|---|
Entropy |
71.4% |
71.4% |
62.5% |
78.9% |
Homogeneity |
81.0% |
57.1% |
66.6% |
73.9% |
For the above mentioned parameters, the combined sensitivity of entropy and homogeneity for predicting outcome was 57.83% and the combined specificity was 87.74%. The Pearson correlation and linear regression analysis did not show any dependence between textural heterogeneity parameters and lesion volume. The value of R for correlation between volume and entropy and volume and homogeneity was 0.002 and 0.004 respectively.
DISCUSSION
In our study, we analyzed the predictive capability of textural heterogeneity parameters in patients undergoing 177Lu-PSMA therapy for determination of patient selection criteria, treatment outcome and survival analysis. The retrospective German multicenter analysis [15] showed that 177Lu-PSMA RLT demonstrated a PSA decline occurred in 65% of patients after 1 cycle of RLT. There are still almost 30% of the patients who did not show or showed less than 50% decline in serum PSA level. It is very important to identify those patients and so that therapy modifications might be performed which can then help in increasing the efficacy of treatment. Our study aimed at utilization of heterogeneity parameters in an effort to improve the selection criterion of patients and acted as a means to predict improved outcome. Our study showed a potential for response prediction through baseline PSMA PET-CT scan using textural features. It also suggested that more heterogeneous the tumor was in PSMA expression more responsive it was to PSMA therapy, thus contributing efficiently towards patient selection, treatment planning and improvement in overall diagnostic accuracy. The ROC analysis showed that two textural heterogeneity parameters entropy and homogeneity were statistically significant (p < 0.05) for predictive ability as obtained from the baseline 68Ga-PSMA scan prior to 177Lu-PSMA therapy. Spearman correlation showed that entropy showed a negative correlation (rs = −0.327 and p = 0.006) and homogeneity showed a positive correlation (rs = 0.315 and p = 0.008) with change in pre and post therapy PSA levels.
Predictive ability of various parameters from the baseline scan has also been previously investigated. Ferdinandus et al., 2017 [5] analyzed the effect of different pretherapeutic parameters on the therapeutic response measured by prostate-specific antigen (PSA) 2 months after radioligandtherapy. Numerous studies have also reported the use of textural heterogeneity parameters for the assessment of patient outcome. Eary et al., [7] proposed that heterogeneity in 18F-FDG spatial distribution can be used to predict tumor biologic aggressiveness. In another study by Cheng et al., 2013 [8] the researchers showed that two textural heterogeneity parameters entropy and homogeneity showed ability to predict outcome in patients with advanced T-stage oropharyngeal squamous cell carcinoma. However, the conventional PET parameters SUV mean and max did not show such ability. Tumor volume also had no effect on textural heterogeneity.
Similarly in another study by Tixier et al., 2011 [9] the aim was to evaluate textural analysis of baseline PET scans for the prediction of therapy response in esophageal cancer. Receiver-operating-characteristic curve analysis showed that tumor textural analysis can provide non-responder, partial-responder, and complete-responder patient identification with higher sensitivity (76%–92%) than any SUV measurement. Textural features of tumor metabolic distribution extracted from baseline 18F-FDG PET images allow for the best stratification of esophageal carcinoma patients in the context of therapy-response prediction. In our study the combined sensitivity of entropy and homogeneity for predicting outcome was 57.8% and the combined specificity was 87.7%.
It is interesting to note that in our results entropy showed a directly proportional correlation with change in pre and post therapy PSA levels while homogeneity showed an inverse relationship. In other words it can be inferred that more heterogeneous the tumor was, the better it responded to the PSMA therapy. As higher entropy is a measure of greater heterogeneity of the tumor. The patients which were labeled as responders owing to decrease in post PSMA therapy PSA levels showed a higher entropy in baseline scan. Similarly, the responders showed lower homogeneity in the baseline scan. Although we did define the response to therapy by PSA levels and did not correlate the textural features with patient outcomes, we have shown in previous studies, that a reduction of PSA after therapy with Lu-177 PSMA is a prognostic factor for overall survival [14, 19]. Therefore, we can assume that the PSMA expression on the tumor cell surface of patients included in the present study was quite high. With increasing heterogeneity, the PSMA expression increased, which might pave the way for an increased uptake of PSMA bound ligands. Consequently, it can be hypothesized that those tumors respond better to therapy. Hence, our study showed that with increased heterogeneity in PSMA expression, a better response to PSMA therapy could be expected.
In a study by Pyka T et al. [10] predictive value of textural heterogeneity parameters in FET-PET for recurrence and prognosis in non-small cell lung carcinoma (NSCLC) patients receiving primary stereotactic radiation therapy (SBRT). This study showed that entropy has predictive potential for local recurrence with an AUC of 0.872. The study also showed that higher value of entropy was linked to poor outcome. In our study entropy was also a predictor for outcome with an AUC of 0.695 however, higher entropy showed better outcome for PSMA therapy.
An interesting question which arises here is whether a more heterogeneous tumor can respond better to the treatment? In many previous studies involving textural heterogeneity it was proven otherwise. Increased textural heterogeneity has already been linked with poor outcome. On the contrary, our study points in the opposite direction. One of the reasons for this behavior could be that this phenomenon can possibly be highly tumor and therapy specific. PSMA shows significant over expression in metastatic, poorly differentiated and therapy refractory carcinomas. Treatment refractory tumors can have the presence of multiple clones resulting in formation of complex systems and contributing towards tumor heterogeneity [19]. Patients included in our study group had already metastatic disease which was treatment refractory. Therefore, we can assume that there was a significant PSMA overexpression in tumors of patients included in our study. More heterogeneous a tumor is, more PSMA expression it shows thereby increasing the uptake of PSMA bound ligands and thus responding better to therapy. In a very interesting study by Jeffrey West and Paul Newton [20] about optimizing chemo-scheduling based on tumor growth rates discussed ways to optimize chemotherapeutic scheduling using a Moran process evolutionary game-theory model of tumor growth that incorporates more general dynamical and evolutionary features of tumor cell kinetics. It proves the fact that over multiple cycles, higher entropy strategies have a bigger impact on faster growing tumors than on slower growing tumors.
Hence, firstly this study showed the possibility of extracting vital data via the analysis of baseline scan only which can directly predict the outcome of patient. This finding can be of excessive importance in selecting the patients which can possibly respond better by altering the treatment regimen. Secondly, this study differentiates the textural parameters which can be used for gaining outcome data and also points out their correlation with the outcome.
This study had some limitations. First, the reproducibility of tumor heterogeneity as assessed by PSMA PET-CT has not been much explored yet. For the assessment of this robustness repeated analysis of PSMA PET-CT studies will have to be performed in a short interval of time. For FDG-PET-CT, such a study has been performed by Tixier et al. and demonstrated reproducibility of textural parameters comparable to the range of conventional SUV [9]. They found that several textural parameters showed reproducibility comparable to the range of conventional SUV. Therefore, these parameters can be applied for therapy response assessment at least with the same confidence as SUV.
The analysis of heterogeneity can also be limited by the size of the lesion. If the lesion becomes too small, the analysis of differences in radiotracer uptake within the lesion does not make sense. Investigating small structures, e.g. lymph node metastases, may challenge the value of textural parameters. In our study, the smallest lesion was 7.8 cm3, which is still about 62 voxels. A second point that needs further investigation is the influence of reconstruction parameters on tissue heterogeneity. PET reconstruction algorithms require smoothing of the raw image data which could influence assessment of tumor textural heterogeneity. PET images assessed in this study were reconstructed using the standard protocols for clinical routine at our institution. For comparison of changes in tumor heterogeneity, all images were acquired and reconstructed with the same set of parameters. Metabolically active tumor volumes were delineated manually instead of using segmentation algorithms with fixed thresholds and might therefore be prone to interindividual differences. However, the appropriate segmentation method is still widely discussed; semiautomatic methods often fail depending on the tumor localization [21, 22]. Therefore, we considered manual delineation to be optimal for our study especially as we included metastases varying in location as well as signal-to-background ratio. Additionally, Hatt and colleagues [23] could demonstrate that the predictive value of textural parameters is not affected by partial volume effect and is relatively independent of the method used to delineate the tumor volumes to be analyzed.
MATERIALS AND METHODS
Inclusion criteria
70 patients with histologically proven prostate cancer were retrospectively included in this study. Clinical data was collected from November 2014 to April 2016. All patients were planned to undergo 177Lu-PSMA-617 (abbreviated as 177Lu-PSMA in this study) RLT. Average age of patients was 71.46 years. Inclusion criteria for this retrospective analysis were progressive metastatic castration-resistant prostate cancer (mCRPC) patients. Patients experienced progression under next-generation androgen-deprivation therapy (e.g., abiraterone, enzalutamide) or first- or second-line chemotherapy (e.g., docetaxel, cabazitaxel) or were not eligible for chemotherapy. All patients eligible for 223Ra received this treatment before undergoing 177Lu-PSMA RLT. 39 patients had prior chemotherapy. 16 patients had been treated previously with 223Ra, while 27 patients had previous external beam radiation therapy (EBRT). Patient characteristics are shown in Table 4.
Table 4: Patient characteristics
Characteristic |
Data |
|---|---|
Age |
71.5 years (48–88 years) |
Site of metastasis: |
|
Bone |
70 (100%) |
Lymph node |
33 (47.1%) |
Other (liver, prostate) |
15 (21.4%) |
Previous therapy of mCRPC: |
|
Androgen deprivation therapy |
70 (100%) |
Chemotherapy |
39 (55.7%) |
223Ra |
16 (22.8%) |
EBRT to bone |
27 (38.5%) |
68Ga-PSMA scan
A 68Ga-PSMA PET scan was performed for every patient. Each patient underwent 68Ga-PSMA scan before therapy with 177Lu-PSMA termed as the baseline scan. The objectives of the baseline scan included staging and therapy planning for all patients. After the baseline scan patients underwent 177Lu-PSMA radioligand therapy. Renal function of every patient was analyzed prior to therapy with 99mTc-MAG3 renal scintigraphy.
Data were acquired with a Biograph Sensation 2 PET/computer tomography (PETCT) scanner (Siemens Medical Solutions). The axial and transverse fields of view were 16.2 and 58.5 cm respectively. The transverse resolution of the scanner was about 6.5 mm, whereas the axial resolution was 6.0 mm, both at a radius of 10 mm. The computer tomography (CT) component was a 2-slice spiral CT scanner. About 73 minutes (range 50–90 minutes) after the intravenous injection of approximately 131.3 MBq (range 98.8 to 174.8 MBq) of 68Ga-PSMA, the patient was placed in the scanner. Low dose CT from the head to mid-thighs was performed followed by the PET scan of the same area in 6–7 bed positions, each for 3–4 minutes depending on the body weight of the patient. The CT data were reconstructed in 512 × 512 pixel matrices. PET data was reconstructed into 128 × 128 matrices in axial, coronal and sagittal planes using the iterative attenuation-weighted ordered subset algorithm implemented by the manufacturer using 4 iterations and 16 subsets. Attenuation and scatter correction was performed using the CT data. Final voxel size was 5.3 mm × 5.3 mm × 5 mm. All patients gave written and informed consent to the imaging procedure. All patient record and information was anonymized before analysis.
PET data analysis
Image data were transferred to an Interview Fusion Workstation (Mediso Medical Imaging System, Budapest, Hungary). Firstly, co-registration between PET and CT images was performed. Tumor volume was manually delineated on PET images (Figure 4) with a standard uptake value (SUV) threshold [24, 25]. All the 70 patients had bone metastasis. Thirty three patients had lymph node metastasis along with bone metastasis. Fifteen patients had additional liver and/or prostate lesions. Three VOIs each for bone and lymph node lesions were delineated manually. Other lesions were also delineated if present in liver and prostate. Parameters to be evaluated were measured in these VOIs. A total of 328 VOIs were delineated. Mean volume of the lesions was 32.9 cm3 (range 7.8 cm3 to 82.3 cm3). For each patient three bone lesions were marked. Similarly, three lymph node and other (liver and prostate) lesions were delineated where applicable. For every patient on average six VOIs were marked (range 3–12 depending on organ involvement. For final analysis a mean value of every included parameter was determined.
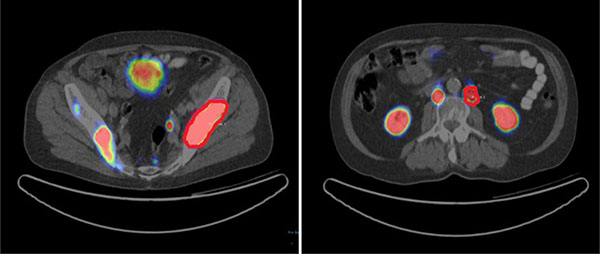
Figure 4: VOIs for analysis of bone and lymph node lesions.
Tumor textural heterogeneity was assessed by extraction of local and global textural features from uptake histogram analysis and normalized gray-level co-occurrence matrix (NGLCM) respectively [17]. The selected heterogeneity parameters were COV, entropy, homogeneity, contrast and size variation (Table 5).
Table 5: Overview of textural heterogeneity parameters
Parameter |
Order |
Description |
|---|---|---|
COV |
1st |
A normalized measure of dispersion of a frequency distribution (standard deviation divided by the mean value of the activity concentration in the tumor volume). |
Entropy |
2nd |
Measures randomness of distribution, e.g. a homogenous matrix demonstrates low entropy. |
Homogeneity |
2nd |
A measure for continuous areas of same or similar voxel values in an image or voxel of interest (VOI). |
Contrast |
2nd |
A measure of local variations present in the image. A high contrast value indicates a high degree of local variation. |
Size Variation |
3rd |
Measures the difference of the grey value when going to the next voxel. It is high when the intensity changes very often between single voxels. |
The selected parameters have been used widely in numerous PET studies and showed a statistically significant ability to depict the role of textural heterogeneity for analysis of tumor behavior [7–12, 17, 18]. SUV mean histogram analysis was used to calculate coefficient of variation (COV) [6, 26]. Rest of the parameters, entropy, homogeneity, contrast and size variation were calculated from NGLCM contained three dimensional gray-level information [6, 26]. For comparison purpose SUV mean as a conventional PET parameter was also analyzed.
Treatment response
After the baseline scan all patients underwent 177Lu-PSMA therapy. The decision for 177Lu-PSMA radioligand therapy was made by the local interdisciplinary tumor board at each therapy center. The protocol followed for therapy has already been explained in detail by Rahabar et al. [15]. The parameters used to assess the response to 177Lu-PSMA therapy were pre and post therapy changes in levels of PSA (prostate specific antigen), serum and bone alkaline phosphate and Eastern Cooperative Oncology Group (ECOG) criterion. Time difference between pre and post therapy levels was 7.1 weeks (average 6–8 weeks). Change in levels of clinical parameters was obtained as post therapy levels minus the pre therapy level (post therapy PSA – pre therapy PSA). A negative value of this equation meant that post therapy PSA was less than that of pre therapy and the case was considered as of a responder and viceversa.
Statistical analysis
The statistical analysis was performed using SPSS (version 22, IBM). To evaluate the correlation between conventional and textural heterogeneity parameters and changes in pre and post therapy clinical parameters Spearman correlation was used. Statistical tests were conducted at a two-sided level of significance as p < 0.05. A multivariate regression analysis was performed to see the dependence between textural heterogeneity parameters and the lesion volume.
Receiver-operating-characteristics (ROC) analysis was also performed using MedCalc software (version 12.3.0.0; MedCalc). ROC analysis was performed to estimate the optimal cutoff value of the correlating parameters for response assessment. For this purpose, the Youden index was used to maximize the sum of sensitivity and specificity [27]. The area under the curve (AUC) was calculated for each parameter using the nonparametric method developed by Hanley and McNeil [28] representing the overall predictive or prognostic performance. For AUCs, exact binominal confidence intervals were calculated (95% confidence level), indicating the statistical significance of predictive capability if the critical value of 0.5 is not included.
To see any correlation between lesion size and parameters with predictive capability Pearson correlation and linear regression analysis was performed.
CONCLUSIONS
Our study showed a potential for response prediction for 177Lu-PSMA therapy through baseline PSMA PET-CT scan using textural features. It also suggested that more heterogeneous the tumor was in PSMA expression more responsive it was to PSMA therapy, thus contributing efficiently towards patient selection, treatment planning and improvement in overall diagnostic accuracy.
Ethics statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Disclosure
Ralph Bundschuh has a noncommercial research contract with Mediso Medical Imaging Systems, Ralph Bundschuh is on the speaker’s bureau for Mediso Medical Imaging Systems, and Norbert Zsótér is employed by Mediso Medical Imaging Systems. All other authors had full control of the data and information submitted for publication.
CONFLICTS OF INTEREST
The authors declare that they have no financial or non-financial competing interests.
REFERENCES
1. Siegel R, Miller K, Jemal A. Cancer statistics, 2015. CA Cancer J Clin. 2015; 65:5–29. http://onlinelibrary.wiley.com/doi/10.3322/caac.21254.
2. Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, Abraham J, Adair T, Aggarwal R, Ahn SY, Alvarado M, Anderson HR, Anderson LM, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012; 380:2095–128. https://doi.org/10.1016/S0140-6736(12)61728-0.
3. Kratochwil C, Giesel FL, Stefanova M, Benešová M, Bronzel M, Afshar-Oromieh A, Mier W, Eder M, Kopka K, Haberkorn U. PSMA-Targeted Radionuclide Therapy of Metastatic Castration-Resistant Prostate Cancer with 177Lu-Labeled PSMA-617. J Nucl Med. 2016; 57:1170–6. https://doi.org/10.2967/jnumed.115.171397.
4. Zechmann CM, Afshar-Oromieh A, Armor T, Stubbs JB, Mier W, Hadaschik B, Joyal J, Kopka K, Debus J, Babich JW, Haberkorn U. Radiation dosimetry and first therapy results with a (124)I/(131)I-labeled small molecule (MIP-1095) targeting PSMA for prostate cancer therapy. Eur J Nucl Med Mol Imaging. 2014; 41:1280–92. https://doi.org/10.1007/s00259-014-2713-y.
5. Ferdinandus J, Eppard E, Gaertner FC, Kürpig S, Fimmers R, Yordanova A, Hauser S, Feldmann G, Essler M, Ahmadzadehfar H. Predictors of Response to Radioligand Therapy of Metastatic Castrate-Resistant Prostate Cancer with 177Lu-PSMA-617. J Nucl Med. 2017; 58:312–19. https://doi.org/10.2967/jnumed.116.178228.
6. Chicklore S, Goh V, Siddique M, Roy A, Marsden PK, Cook GJ. Quantifying tumour heterogeneity in 18F-FDG PET/CT imaging by texture analysis. Eur J Nucl Med Mol Imaging. 2013; 40:133–40. https://doi.org/10.1007/s00259-012-2247-0.
7. Eary JF, O’Sullivan F, O’Sullivan J, Conrad EU. Spatial heterogeneity in sarcoma 18F-FDG uptake as a predictor of patient outcome. J Nucl Med. 2008; 49:1973–79. https://doi.org/10.2967/jnumed.108.053397.
8. Cheng NM, Fang YH, Chang JT, Huang CG, Tsan DL, Ng SH, Wang HM, Lin CY, Liao CT, Yen TC. Textural features of pretreatment 18F-FDG PET/CT images: prognostic significance in patients with advanced T-stage oropharyngeal squamous cell carcinoma. J Nucl Med. 2013; 54:1703–09. https://doi.org/10.2967/jnumed.112.119289.
9. Tixier F, Le Rest CC, Hatt M, Albarghach N, Pradier O, Metges JP, Corcos L, Visvikis D. Intratumor heterogeneity characterized by textural features on baseline 18F-FDG PET images predicts response to concomitant radiochemotherapy in esophageal cancer. J Nucl Med. 2011; 52:369–78. https://doi.org/10.2967/jnumed.110.082404.
10. Pyka T, Bundschuh RA, Andratschke N, Mayer B, Specht HM, Papp L, Zsótér N, Essler M. Textural features in pre-treatment [F18]-FDG-PET/CT are correlated with risk of local recurrence and disease-specific survival in early stage NSCLC patients receiving primary stereotactic radiation therapy. Radiat Oncol. 2015; 10:100. https://doi.org/10.1186/s13014-015-0407-7.
11. Bundschuh RA, Dinges J, Neumann L, Seyfried M, Zsótér N, Papp L, Rosenberg R, Becker K, Astner ST, Henninger M, Herrmann K, Ziegler SI, Schwaiger M, Essler M. Textural Parameters of Tumor Heterogeneity in 18F-FDG PET/CT for Therapy Response Assessment and Prognosis in Patients with Locally Advanced Rectal Cancer. J Nucl Med. 2014; 55:891–7. https://doi.org/10.2967/jnumed.113.127340.
12. Divrik RT, Türkeri L, Şahin AF, Akdoğan B, Ateş F, Çal Ç, Baltacı S, and Urooncology Association. Prediction of response to androgen deprivation therapy and castration resistance in primary metastatic prostate cancer. Urol Int. 2012; 88:25–33. Abstract https://doi.org/10.1159/000334539.
13. El Naqa I, Grigsby P, Apte A, Kidd E, Donnelly E, Khullar D, Chaudhari S, Yang D, Schmitt M, Laforest R, Thorstad W, Deasy JO. Exploring feature-based approaches in PET images for predicting cancer treatment outcomes. Pattern Recognit. 2009; 42:1162–71. https://doi.org/10.1016/j.patcog.2008.08.011.
14. Ahmadzadehfar H, Wegen S, Yordanova A, Fimmers R, Kürpig S, Eppard E, Wei X, Schlenkhoff C, Hauser S, Essler M. Overall survival and response pattern of castration-resistant metastatic prostate cancer to multiple cycles of radioligand therapy using [177Lu]Lu-PSMA-617. Eur J Nucl Med Mol Imaging. 2017; 44:1448–54. https://doi.org/10.1007/s00259-017-3716-2.
15. Rahbar K, Ahmadzadehfar H, Kratochwil C, Haberkorn U, Schäfers M, Essler M, Baum RP, Kulkarni HR, Schmidt M, Drzezga A, Bartenstein P, Pfestroff A, Luster M, et al. German Multicenter Study Investigating 177Lu-PSMA-617 Radioligand Therapy in Advanced Prostate Cancer Patients. J Nucl Med. 2017; 58:85–90. https://doi.org/10.2967/jnumed.116.183194.
16. Rahbar K, Schmidt M, Heinzel A, Eppard E, Bode A, Yordanova A, Claesener M, Ahmadzadehfar H. Response and Tolerability of a Single Dose of 177Lu-PSMA-617 in Patients with Metastatic Castration-Resistant Prostate Cancer: A Multicenter Retrospective Analysis. J Nucl Med. 2016; 57:1334–38. https://doi.org/10.2967/jnumed.116.173757.
17. Dong X, Sun X, Sun L, Maxim PG, Xing L, Huang Y, Li W, Wan H, Zhao X, Xing L, Yu J. Early Change in Metabolic Tumor Heterogeneity during Chemoradiotherapy and Its Prognostic Value for Patients with Locally Advanced Non-Small Cell Lung Cancer. PLoS One. 2016; 11:e0157836. https://doi.org/10.1371/journal.pone.0157836.
18. Dong X, Wu P, Sun X, Li W, Wan H, Yu J, Xing L. Intra-tumour 18F-FDG uptake heterogeneity decreases the reliability on target volume definition with positron emission tomography/computed tomography imaging. J Med Imaging Radiat Oncol. 2015; 59:338–45. https://doi.org/10.1111/1754-9485.12289.
19. Ahmadzadehfar H, Eppard E, Kürpig S, Fimmers R, Yordanova A, Schlenkhoff CD, Gärtner F, Rogenhofer S, Essler M. Therapeutic response and side effects of repeated radioligand therapy with 177Lu-PSMA-DKFZ-617 of castrate-resistant metastatic prostate cancer. Oncotarget. 2016; 7:12477–88. https://doi.org/10.18632/oncotarget.7245.
20. West J, Newton PK. Chemotherapeutic dose scheduling based on tumor growth rates provides a case for low-dose metronomic high-entropy therapies. Cancer Res. 2017; 77:6717–28. https://doi.org/10.1158/0008-5472.CAN-17-1120.
21. Bundschuh RA, Andratschke N, Dinges J, Duma MN, Astner ST, Brügel M, Ziegler SI, Molls M, Schwaiger M, Essler M. Respiratory gated [18F]FDG PET/CT for target volume delineation in stereotactic radiation treatment of liver metastases. Strahlenther Onkol. 2012; 188:592–8. https://doi.org/10.1007/s00066-012-0094-3.
22. Zaidi H, Abdoli M, Fuentes CL, El Naqa IM. Comparative methods for PET image segmentation in pharyngolaryngeal squamous cell carcinoma. Eur J Nucl Med Mol Imaging. 2012; 39:881–91. https://doi.org/10.1007/s00259-011-2053-0.
23. Hatt M, Tixier F, Cheze Le Rest C, Pradier O, Visvikis D. Robustness of intratumour 18F-FDG PET uptake heterogeneity quantification for therapy response prediction in oesophageal carcinoma. Eur J Nucl Med Mol Imaging. 2013; 40:1662–71. https://doi.org/10.1007/s00259-013-2486-8.
24. Fendler WP, Rahbar K, Herrmann K, Kratochwil C, Eiber M. 177Lu-PSMA Radioligand Therapy for Prostate Cancer. J Nucl Med. 2017; 58:1196–1200. https://doi.org/10.2967/jnumed.117.191023.
25. Mathieu C, Ferrer L, Carlier T, Colombié M, Rusu D, Kraeber-Bodéré F, Campion L, Rousseau C. Assessment of Lymph Nodes and Prostate Status Using Early Dynamic Curves with 18F-Choline PET/CT in Prostate Cancer. Front Med (Lausanne). 2015; 2:67. https://doi.org/10.3389%2Ffmed.2015.00067.
26. Tixier F, Hatt M, Le Rest CC, Le Pogam A, Corcos L, Visvikis D. Reproducibility of tumor uptake heterogeneity characterization through textural feature analysis in 18F-FDG PET. J Nucl Med. 2012; 53:693–700. https://doi.org/10.2967/jnumed.111.099127.
27. Youden WJ. Index for rating diagnostic tests. Cancer. 1950; 3:32–35. https://doi.org/10.1002/1097-0142(1950)3:1%3C32::AID-CNCR2820030106%3E3.0.CO;2-3.
28. Hanley JA, McNeil BJ. The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology. 1982; 143:29–36. https://doi.org/10.1148/radiology.143.1.7063747.

