INTRODUCTION
Hepatitis B virus (HBV) and hepatitis C virus (HCV) are the two most common hepatotropic viruses responsible for majority of acute and chronic hepatitis worldwide [1]. Over 350 million individuals chronically infected with HBV are at high risk of developing liver cirrhosis and hepatocellular carcinoma (HCC) [2]. HBV is a small hepatotropic DNA virus. Serological markers for HBV infection include HBsAg, anti-HBs, HBeAg, anti-HBe, and anti-HBc. HBsAg is the hallmark of infection while HBcAb is an indicator of past or present hepatitis B infection [3]. The prevalence of HBV infection varies markedly throughout the world. 45% of HBV-infected individuals live in highly endemic areas, which include China, Southeast Asia, sub-Saharan Africa and the Amazon Basin [4, 5]. Chronic infection with HCV is another major risk factor for the development of HCC worldwide. Unlike HBV, HCV is a positive-sense single-stranded RNA virus of the family Flaviviridae [6]. The highest prevalence of HCV has been reported in Africa and the Middle East, with a lower prevalence in the Americas, Australia and Northern and Western Europe [7].
Systemic lupus erythematous (SLE) is a classic systemic autoimmune diseases characterized by chronic inflammation, autoantibodies production, complement activation and immune-complex deposition, resulting in tissue and organ damage. SLE is occurring predominantly in young women with the female: male ratio of 10:1. Overall, the incidence of SLE is higher in African, American and Asian populations than in Caucasians [8]. The cause of SLE is not fully understood, but it is believe to involve hormonal, environmental, genetic and immunological factors [9].
Autoimmune disease is closely related to viral infection since it can be induced or triggered by viruses. For example, EBV was found to be associated with SLE and RA [10]. In contrast, some viral infections can also protect individuals from specific autoimmune diseases. CMV and EBV infection were shown to play a protective role in type 1 diabetes [11, 12]. Although the potential association between HBV and SLE has been studied for decades it still remains controversial. HCV infection is associated with many autoimmune processes [13], but the association between HCV infection and SLE disease has not been clearly established. Therefore, the current study was designed to evaluate the prevalence of hepatitis virus infection among SLE patients through meta-analysis of published studies.
RESULTS
Characteristics of the included studies
A flow diagram of studies selection is shown in Figure 1. A total of 2446 articles met the defined search criteria. Further screen of their titles and abstracts identified the potentially relevant articles. Finally, 22 studies were selected for the meta-analysis [14–33].
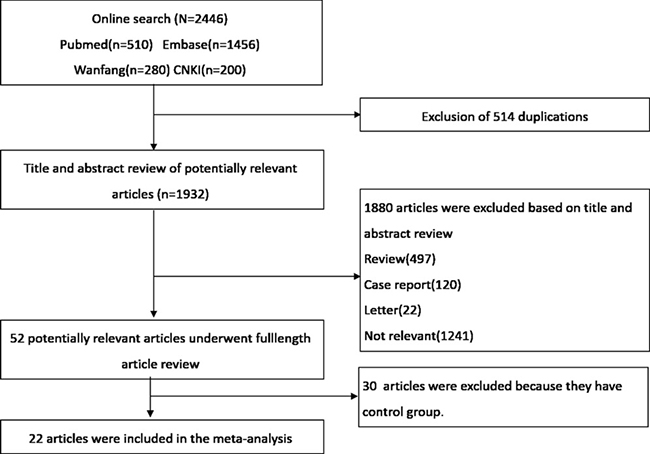
Figure 1: Flowchart depicting the selection of studies for the meta-analysis.
As listed in Table 1, 11 case-control studies, published between 1997 and 2016, were identified to analyze HBV infection state using HBsAg. All of the 11 studies were from the Asian. Of those, 8 studies were from China, one from China Taiwan, one from Japan and one from Israel. 4 studies were retrospective design, and 7 were prospective. Altogether, 127 cases of HBV infection in 9333 SLE patients were reported. Among 203329 control individuals, 16392 cases of HBV infection were identified. Controls included healthy subjects in 4 studies, non-SLE inpatients in another 4 studies, and 3 studies used rheumatoid arthritis (RA) patients as controls.
Table 1: Characteristics of included studies (HBsAg)
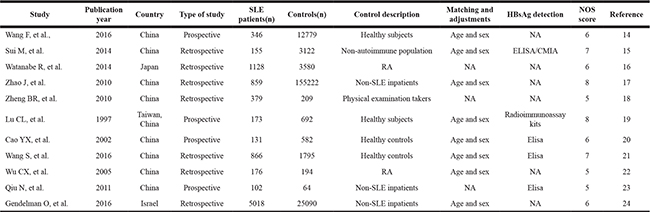
Table 2 showed the 7 studies published between 1997 and 2016, which analyzed the past or present hepatitis B infection using HBcAb status. Among these studies, 3 studies were from China, 2 studies were from Israel, one from China Taiwan and one from Japan. 4 studies selected controls from healthy subjects, 1 study used non-SLE inpatients and 2 studies used rheumatoid arthritis (RA) patients as controls.
Table 2: Characteristics of included studies (HBcAb)

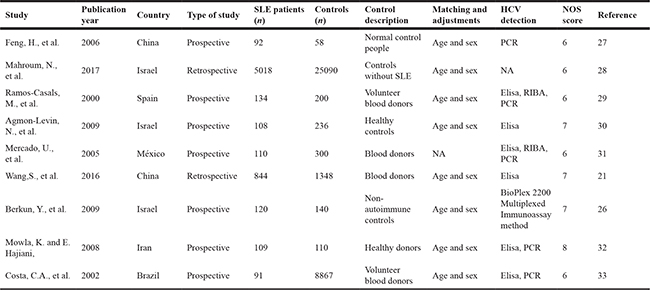
9 studies published, between 2000 and 2017, were included to analyze the prevalence of HCV infection among SLE patients. All of the 9 studies were conducted either in Asia or South America. 7 studies were retrospective studies and 2 were prospective. The quality of included studies ranged from moderate to good, varying from six to eight points, based on NOS scoring system. The detail characteristics of the included studies are listed in Table 3.
Table 3: Characteristics of included studies (HCV)
The prevalence of HBV infection in patients with SLE
We identified 11 case-control results that associated SLE with HBsAg positivity indicative of HBV infection. Of those, 10 studies from Asia reported relatively lower rate of HBsAg positivity in patients diagnosed with SLE compared with the control population, whereas one study from Israel did not support this observation [24]. In a meta-analysis of these studies, the pooled odds ratio was (OR: 0.28; 95% CI: 0.13, 0.61) in a random effect model for HBsAg positive rate in SLE patients compared with control population. However, we detected significant heterogeneity among the studies (I2 = 92%, P < 0.00001), which might be due to the study from Israel. If this study was further excluded, the adjusted OR of HBsAg in patients with SLE was 0.24 (95% CI: 0.17, 0.33). No significant heterogeneity was observed after adjustment (I2 = 32%, P = 0.15) (Figure 2A). The funnel plot and egger’s test were used to assess the publication bias of the included studies. The funnel plot was symmetric (Figure 2B) and the egger’s test showed no significant publication bias (P = 0.869).
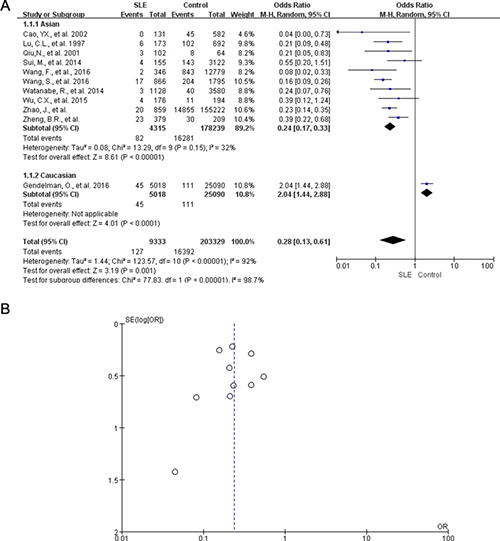
Figure 2: Meta-analysis of HBsAg positivity rate in SLE patients and controls. (A) Forest plot of the meta-analysis for the HBsAg positive rate in patients with SLE versus controls, OR, odds ratio; CI, confidence Interval. (B) Funnel plots showing lack of bias in 11 studies measuring the rate of HBsAg positivity in SLE patients and controls.
Moreover, we conducted additional meta-analysis to evaluate the infection status of HBV in SLE patients using the HBcAb positive rate. For this, 7 studies with 1282 participants were included in pooled analysis. The risk of HBcAb-positive rate in patients with SLE was 3.13-fold lower (pooled OR 0.32, 95% CI 0.23–0.46) than that in the control population. There was a moderate heterogeneity between studies with an I2 of 53% (P = 0.05) (Figure 3A). If the study from Wang, F., et al. 2016 was excluded, the adjusted OR of HBsAg in patients with SLE was 0.4 (95% CI: 0.31, 0.50). No significant heterogeneity was observed after adjustment (I2 = 0%, P = 0.56) (Supplementary Table 1). The funnel plot was symmetric (Figure 3B) and the egger’s test showed no significant publication bias (P = 0.145).
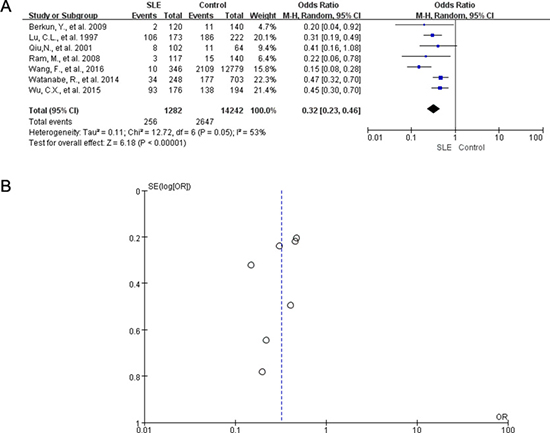
Figure 3: Meta-analysis comparing the rate of HBcAb positivity in SLE patients and controls. (A) Forest plot shows the HBcAb positive rate in patients with SLE versus controls, OR, odds ratio; CI, confidence Interval. (B) Funnel plots showed no publication bias in 7 studies measuring HBcAb positive rate in SLE patients and controls.
The prevalence of HCV infection in patients with SLE
We also conducted a meta-analysis to evaluate the risk of HCV infection in SLE patients. 9 case control studies reported the prevalence of HCV infection in SLE patients. Of those, 8 studies showed that the HCV positive rate was higher in SLE patients compared with the control population. In the meta-analysis of all 9 studies, the pooled OR was 2.91 (95% CI: 2.21, 3.84) in a fixed-effects model (Figure 4A), There was no statistically significant heterogeneity among studies (I2 = 18%; P = 0.28). The subgroup analysis showed no significant change in both the PCR group and non-PCR group (Supplementary Figure 1). Omission of any single study did not significantly change the overall OR (Supplementary Table 2). No evident asymmetry of plots was seen in the funnel plots (Figure 4B) and the Egger’s test showed no significant publication bias (P = 0.512).
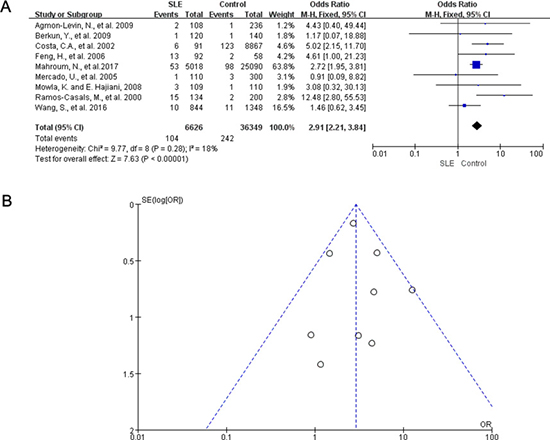
Figure 4: Meta-analysis of the prevalence rate for HCV in SLE patients and controls. (A) Forest plot showing the prevalence of HCV infection in patients with SLE versus controls. OR, odds ratio; CI, confidence Interval. (B) Funnel plots showed no publication bias in 9 studies examining HCV prevalence rate in SLE patients and controls.
DISCUSSION
The infection of HBV and HCV has posed a major public-health problem worldwide and is the major cause leading to chronic liver disease. Ineffective antiviral immune responses have been implicated as the critical factors leading to development of chronic HBV and HCV infections [34]. Although, viral infections and autoimmunity are closely associated their association often remains controversial. For example, some studies proposed that HBV or HCV infection represent a triggering factor for development of systemic autoimmune diseases [13, 34]. In contrast, it has also been suggested that HBV infection can afford a protection against development of autoimmune disorders [11, 35]. SLE is a classical autoimmune disease, which similarly to HBV affects many people worldwide, however the relation between SLE and hepatitis virus infection remains unknown. Here, we present a meta-analysis to explore the prevalence of HBV or HCV in SLE patients. The results of our meta-analysis point to a low prevalence of HBV infection in patients with SLE in highly endemic areas. The risk of HBsAg positive rate in SLE patients was lower when compared with the control group, suggesting a protective role of pro-inflammatory environment in SLE against HBV infection. This is in contrast with HCV infections, which manifest high prevalence in SLE patients compared to controls.
In this meta-analysis, the pooled OR was 0.28 for HBsAg positive rate in SLE patients compared with control population, however a significant heterogeneity was observed among the studies. Particularly, a sole study conducted in Israel revealed a different conclusion. Upon exclusion of this study, the adjusted OR of HBsAg in patients with SLE was 0.21, and no significant heterogeneity was then observed. However, our analyses suggest that a positive rate of HBsAg in SLE patients may vary among different endemic regions. Of interest, in highly endemic Asian areas, HBsAg positive rate was lower in patients with SLE than that of the control group. Moreover, to evaluate the prevalence of HBV infection in SLE patients we performed additional meta-analysis in which the level of anti-HBcAb was analysed. The presence of anti-HBcAb in serum is indicative of previous or current HBV infections. Consistent with our previous findings, our results confirmed that the rate of circulating anti-HBcAb was also lower in patients with SLE compared to the control group. These analyses therefore suggested that SLE autoimmunity exerted a protection against HBV infections. The mechanism of lower prevalence of HBV in SLE patients is still unclear. One explanation is that cytokines including IFN-α, IL-6, TNF-α are over-expressed in SLE patients. IFN-α can induce transcription of IFN responsive genes through Jak-STATs signaling pathway, which plays a critical role in the innate immune response against viral infections [36]. IFN-α is commonly used for the treatment of chronic hepatitis B (CHB) patients [37]. IL-6 production is also increased in SLE patients and involved in lupus pathogenesis [38]. Interestingly, IL-6 is a key cytokine for early control HBV infection through suppression of HBV transcription, antigen expression and replication [39]. Therefore enhanced production of IL-6 in SLE patients may have an inhibitory effect on HBV infection.
Another possibility is the association of androgen deficiency observed in SLE with HBV infection [40]. As two large prospective studies have shown, HBV carriers exhibited higher androgen concentrations than healthy controls [41, 42], therefore androgen deficiency observed in SLE patients may prevent the establishment of chronic HBV infection.
Unlike HBV, this meta-analysis demonstrated that the prevalence of HCV in SLE patients was higher than in the control group. HCV and HBV belong to different viral families (Flaviviridae and Hepadnoviridae, respectively). They are characterized by different genetic structures and epidemic features. At present, the reason for the high prevalence of HCV in SLE patients remains unclear. One explanation for higher frequency of HCV infection in patients with SLE compared to the control population could be attributed immunological dysregulation observed among SLE patients, and this may be further compounded by immunosuppressive therapies.
The present study has some limitations. First, most of the studies included in these meta-analyses were conducted in Asia where the rates of CHB are high. Additional studies regarding the percentage of HBV infection among SLE patients in other regions, such as Europe and America, should be performed in the future. Second, several studies relied on HCV diagnosis using only a traditional Elisa approach, rather that HCV RNA analysis, which is a more sensitive and accurate detection method. Nevertheless, to our knowledge, this is the first comprehensive meta-analysis to evaluate up-to-date observational studies that reported a relationship between SLE and HBV or HCV infections.
In conclusion, this meta-analysis revealed a relationship between HBV/HCV infection and SLE. Interestingly, we identified a low prevalence of HBV infection and a high prevalence of HCV infection in patients with SLE. However, the precise mechanism by which this occurs remains obscure. Further mechanistic studies are necessary to determine the role of SLE in HBV/HCV infection.
MATERIALS AND METHODS
Search strategy
The following databases were used in this study: PubMed/MEDLINE, EMBASE, as well as two major Chinese databases, China National Knowledge Infrastructure (CNKI) and Wanfang Data. The keywords or subject headings used were ‘‘hepatitis B or HBV or HBsAg or HBcAb or Hepatitis C or HCV’’ and ‘‘systemic lupus erythematosus or SLE’’, from the earliest date available to June 30, 2017. Non-English publications were also included. The bibliographies of selected original studies, reviews, and relevant abstracts were screened.
Inclusion and exclusion criteria
For each eligible study, the title and/or abstract were screened independently by two authors. Any disagreement was resolved by discussion between the authors. We included studies that met the following inclusion criteria: (1) an original case–control study (retrospective, prospective) comparing HBV or HCV infection rate between SLE patients and controls; (2) study reporting the absolute numbers of cases and controls as well as the positive rate of HBV or HCV infection; (3) Described the serological markers for defined HBV and HCV infection. Abstracts, reviews, letters, case reports, and studies that did not provide sufficient data were excluded.
Quality assessment
The methodological quality of the included studies was assessed by New castle Ottawa Scale (NOS). NOS, a star system allowing a semi-quantitative assessment of nonrandomized study quality for observed studies, contained eight items that were categorized into three major components, including selection, comparability, and exposure (case-control studies). NOS assigns a maximum of 4 points for selection, 2 for comparability, and 3 for exposure or outcome. We assigned NOS scores of 1–3, 4–6, and 7–9 for low-, intermediate-, and high-quality studies, respectively.
Data extraction
We obtained the following data from each article by using a standardized protocol: last name of the first author, study name, publication year, country where the study was conducted, prospective or retrospective nature of the study, diagnostic method of HBV infection, number of patients with HBV or HCV infection in SLE and control groups as well as the details of the controls used in the studies.
Statistical analysis
The meta-analysis was performed using Review Manager 5.3 software from the Cochrane Collaboration (London, UK). We calculated the odds ratio (OR) and 95% confidence intervals (CI) to assess the prevalence of HBV and HCV infection in the SLE group compared with the control group. In the forest plots, OR > 1 represented a risk effect and OR < 1 indicated a protective effect. The heterogeneity of the studies was evaluated using the Chi-square test and I2 statistic. The fixed-effects model was used if the heterogeneity was insignificant (Chi-square test P ≥ 0.10 and I2 ≤ 50%), while the random-effects model was preferred if significant heterogeneity was found (Chi-square test P < 0.10 or I2 > 50%). The funnel plot and Egger’s test were used to analyze publication bias.
Author contributions
Sen Wang and Yuxin Chen contributed equally to this work. Sen Wang and Yuxin Chen designed the study, analyzed the data and wrote the manuscript. Xuejing Xu and Wei Hu collected the relevant papers and data. Junhao Chen and Han Shen analyzed the data and gave suggestions. All authors reviewed the manuscript.
ACKNOWLEDGMENTS AND FUNDING
This work was supported by funding from National Natural Science Foundation of China (No.81601765 and 81600201) and supported by Nanjing Medical Science and technique Development Foundation (QRX17142). The funders had no role in the design, execution, and writing up of the study.
CONFLICTS OF INTEREST
The authors state no conflicts of interest.
REFERENCES
1. El-Serag HB. Epidemiology of viral hepatitis and hepatocellular carcinoma. Gastroenterology. 2012; 142:1264.
2. Trepo C, Chan HL, Lok A. Hepatitis B virus infection. Lancet. 2014; 384:2053–2063.
3. Seeger C, Mason WS. Molecular biology of hepatitis B virus infection. Virology. 2015; 479-480:672-686.
4. MacLachlan JH, Cowie BC. Hepatitis B virus epidemiology. Cold Spring Harb Perspect Med. 2015; 5:a21410.
5. Locarnini S, Hatzakis A, Chen DS, Lok A. Strategies to control hepatitis B: Public policy, epidemiology, vaccine and drugs. J Hepatol. 2015; 62:S76–S86.
6. Suzuki T, Aizaki H, Murakami K, Shoji I, Wakita T. Molecular biology of hepatitis C virus. J Gastroenterol. 2007; 42:411–423.
7. Hajarizadeh B, Grebely J, Dore GJ. Epidemiology and natural history of HCV infection. Nat Rev Gastroenterol Hepatol. 2013; 10:553–562.
8. Danchenko N, Satia JA, Anthony MS. Epidemiology of systemic lupus erythematosus: a comparison of worldwide disease burden. Lupus. 2006; 15:308–318.
9. Squatrito D, Emmi G, Silvestri E, Ciucciarelli L, D'Elios MM, Prisco D, Emmi L. Pathogenesis and potential therapeutic targets in systemic lupus erythematosus: from bench to bedside. Auto Immun Highlights. 2014; 5:33–45.
10. Toussirot E, Roudier J. Epstein-Barr virus in autoimmune diseases. Best Pract Res Clin Rheumatol. 2008; 22:883–896.
11. Kivity S, Agmon-Levin N, Blank M, Shoenfeld Y. Infections and autoimmunity – friends or foes? Trends Immun. 2009; 30:409–414.
12. Krause I, Anaya JM, Fraser A, Barzilai O, Ram M, Abad V, Arango A, Garcia J, Shoenfeld Y. Anti-infectious antibodies and autoimmune-associated autoantibodies in patients with type I diabetes mellitus and their close family members. Ann N Y Acad Sci. 2009; 1173:633–639.
13. McMurray RW, Elbourne K. Hepatitis C virus infection and autoimmunity. Semin Arthritis Rheum. 1997; 26:689–701.
14. Wang F, Lv S, Cai J, Zhou X, Xu J. Clinical analysis of hepatitis B virus infection in patients with systemic lupus erythematosus and rheumatoid arthritis. Int J Rheum Dis. 2016; 19:116.
15. Sui M, Wu R, Hu X, Zhang H, Jiang J, Yang Y, Niu J. Low prevalence of hepatitis B virus infection in patients with autoimmune diseases in a Chinese patient population. J Viral Hepatitis. 2014; 21:925–929.
16. Watanabe R, Ishii T, Kobayashi H, Asahina I, Takemori H, Izumiyama T, Oguchi Y, Urata Y, Nishimaki T, Chiba K, Komatsuda A, Chiba N, Miyata M, et al. Prevalence of hepatitis B virus infection in patients with rheumatic diseases in Tohoku area: A retrospective multicenter survey. Tohoku J Exp Med. 2014; 233:129–133.
17. Zhao J, Qiu M, Li M, Lu C, Gu J. Low prevalence of hepatitis B virus infection in patients with systemic lupus erythematosus in southern China. Rheumatol Int. 2010; 30:1565–1570.
18. Zheng BR, Li TW, Huang ZX, Wang M, Deng WM, Liao ZT, Lin ZM, Gu JR. Prevalence of hepatitis B virus carrier status in patients with ankylosing spondylitis and their association with HLA-B27. Int J Rheum Dis. 2010; 13:150.
19. Lu CL, Tsai ST, Chan CY, Hwang SJ, Tsai CY, Wu JC, Lu RH, Lin BC, Lee SD. Hepatitis B infection and changes in interferon-alpha and -gamma production in patients with systemic lupus erythematosus in Taiwan. J Gastroenterol Hepatol. 1997; 12:272–276.
20. Cao YX, Wang B, Yu XY, Chen Y. Relationship between systemic lupus erythematosus and hepatitis B infection and cytokine regulation. Chin J Rheumatol. 2002; 6:101–103.
21. Wang S, Huang TH, Gao S, Chen JH. Prevalence of Hepatitis B Virus Infection in Systemic Lupus Erythematosus Patients. J Mod Lab Med. 2016; 41–43.
22. Wu CX, Zeng AZ. Analysis of Hepatitis B virus infection in 370 patients with systemic autoimmune disease. J Mod Med & Health. 2015; 2161–2162.
23. Qiu N, Chen ZQ, Cai XL, Tao SN. Infection of hepatitis B virus in the patients with systemic lupus erythematosus. Chin J Leprosy & Skin Dis. 2001; 17:19–20.
24. Gendelman O, Mahroum N, Comaneshter D, Rotman-Pikielny P, Cohen AD, Amital H, Sherf M. Hepatitis B carrier state among SLE patients: case-control study. Immunol Res. 2017; 65:257–261.
25. Ram M, Anaya JM, Barzilai O, Izhaky D, Porat KB, Blank M, Shoenfeld Y. The putative protective role of hepatitis B virus (HBV) infection from autoimmune disorders. Autoimmun Rev. 2008; 7:621–625.
26. Berkun Y, Zandman-Goddard G, Barzilai O, Boaz M, Sherer Y, Larida B, Blank M, Anaya JM, Shoenfeld Y. Infectious antibodies in systemic lupus erythematosus patients. Lupus. 2009; 18:1129–1135.
27. Feng H, Zhang GY, Xie HF, Chen ML, Shi W, Wang LY. [Hepatitis C virus infection combined with systemic lupus erythematosus]. J Central South Univ (Med Ed). 2006; 31:891–893. [Article in Chinese].
28. Mahroum N, Hejly A, Tiosano S, Gendelman O, Comaneshter D, Cohen AD, Amital H. Chronic hepatitis C viral infection among SLE patients: the significance of coexistence. Immunol Res. 2017; 65:477–481.
29. Ramos-Casals M, Font J, Garcia-Carrasco M, Cervera R, Jimenez S, Trejo O, de la Red G, Sanchez-Tapias JM, Ingelmo M. Hepatitis C virus infection mimicking systemic lupus erythematosus: study of hepatitis C virus infection in a series of 134 Spanish patients with systemic lupus erythematosus. Arthritis Rheum. 2000; 43:2801–2806.
30. Agmon-Levin N, Ram M, Barzilai O, Porat-Katz BS, Parikman R, Selmi C, Gershwin ME, Anaya JM, Youinou P, Bizzaro N, Tincani A, Tzioufas AG, Cervera R, et al. Prevalence of hepatitis C serum antibody in autoimmune diseases. J Autoimmun. 2009; 32:261–266.
31. Mercado U, Avendano-Reyes M, Araiza-Casillas R, Diaz-Molina R. [Prevalance of antibodies against hepatitis C and B viruses in patients with systemic lupus erythematosus]. Rev Gastroenterol Mex. 2005; 70:399–401. [Article in Spanish].
32. Mowla K, Hajiani E. Prevalence of hepatitis C virus infection in patients with systemic lupus erythematosus: A case-control study. Hepatitis Mon. 2008; 8:41–44.
33. Costa CA, Papi JA, Coelho HS, Nogueira C, Vanderboght B, Soares JA. [Prevalence of hepatitis C in patients with systemic lupus erythematosus in the Hospital of Federal University of Rio de Janeiro (HUCCF)]. Rev Assoc Med Bras (1992). 2002; 48:42–47. [Article in Portuguese].
34. Rehermann B, Nascimbeni M. Immunology of hepatitis B virus and hepatitis C virus infection. Nat Rev Immunol. 2005; 5:215–229.
35. Liu X, Jiao Y, Cui B, Gao X, Xu J, Zhao Y. The potential protective role of hepatitis B virus infection in pristane-induced lupus in mice. Lupus. 2016; 25:1180–1189.
36. Schoggins JW, Rice CM. Interferon-stimulated genes and their antiviral effector functions. Curr Opin Virol. 2011; 1:519–525.
37. Pei RJ, Chen XW, Lu MJ. Control of hepatitis B virus replication by interferons and Toll-like receptor signaling pathways. World J Gastroenterol. 2014; 20:11618–11629.
38. Linker-Israeli M, Deans RJ, Wallace DJ, Prehn J, Ozeri-Chen T, Klinenberg JR. Elevated levels of endogenous IL-6 in systemic lupus erythematosus. A putative role in pathogenesis. J Immunol. 1991; 147:117–123.
39. Hosel M, Quasdorff M, Wiegmann K, Webb D, Zedler U, Broxtermann M, Tedjokusumo R, Esser K, Arzberger S, Kirschning CJ, Langenkamp A, Falk C, Buning H, et al. Not interferon, but interleukin-6 controls early gene expression in hepatitis B virus infection. Hepatology. 2009; 50:1773–1782.
40. James WH. A potential explanation of the reported low prevalence of hepatitis B virus infection in patients with systemic lupus erythematosus. Rheumatol Int. 2012; 32:835.
41. Yu MW, Chen CJ. Elevated serum testosterone levels and risk of hepatocellular carcinoma. Cancer Res. 1993; 53:790.
42. Yuan JM, Ross RK, Stanczyk FZ, Govindarajan S, Gao YT, Henderson BE, Yu MC. A cohort study of serum testosterone and hepatocellular carcinoma in Shanghai, China. Int J Cancer. 1995; 63:491–493.

