INTRODUCTION
According to GLOBOCAN 2012 report [1], there were about 14.1 million new cancer cases and 8.2 million deaths related to the cancer in 2012. By 2025, it predicted that there would be 19.3 million new cases of cancer per year. In America, cancer is the second leading cause of death and promises to be the first place for the cause of death in next few years [2]. In spite of that, a large number of researchers are involved in cancer therapeutic and diagnostic works, the prognosis is still poor for most malignancies. Therefore, seeking prognostic indicators for the cancer seem important in our future scientific research.
In the past few years, B7-H4 (B7S1/VTCN1/B7x), a member of B7/CD28 superfamily, has been studied in many kinds of malignant tumors, including breast, lung, gastric, pancreatic, colorectal, melanoma and prostate cancer. Besides, the expression level of B7-H4 in these cancer patients is obviously extensive compared with normal ones [3]. Recent studies have shown that B7-H4 can inhibit the proliferation, activation and cytokine secretion of T cells in tumor environment, and the B7-H4 expression is associated with many clinicopathological parameters such as tumor size, primary tumor classification, TNM malignant tumor score, overall survival, and tumor infiltrating T cells [3, 4]. Recently, cancer therapies with antibodies against PD-L1 were shown to increase lifetime of particular sorts of cancers. However, not all of the cancer patients would respond to these drugs [5–7]. PD-L1 is expressed in some human cancers, but as described above, B7-H4 is expressed in a much wider range of tumors [8]. Therefore, considered the more extensive expression of B7-H4 compared with the PD-L1 in human cancer and the mechanism of B7-H4 regulating tumor development and progression, we suspect that B7-H4 may be used as a potential target for cancer treatment.
Several literatures have reported that decreased overall survival (OS) and disease-free survival (DFS) is related to the overexpression of B7-H4 [9–11]. However, Zang et al reported that B7-H4 overexpression was not notably associated with DFS (p = 0.1) [12, 13]. Moreover, B7-H4 can be detected both in tumor tissue and patients’ blood, and there still lacks a systematic pooled analysis of these two aspects so far. Thus, we conducted this meta-analysis to assess the role of B7-H4 in the prognosis of patients with cancer.
RESULTS
Excluded and included studies
A total of 282 articles were initially found by using above-mentioned searching strategy. After a screening of the titles or abstracts, 44 records were identified associated with the relationship between the expression of B7-H4 and patient prognosis in kinds of malignant tumors. Among these, 17 articles were excluded (13 lacked important data, 1 detected B7-H4 not in tissue or blood and 3 covered the same patient population). As a result, 27 studies were enrolled for present meta-analysis (Figure 1).
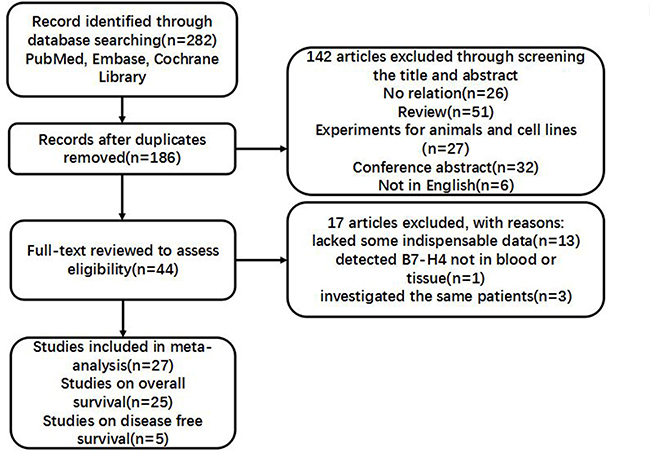
Figure 1: Flow chart for research selection strategy.
Study characteristics
In total, 3771 patients from China, Japan, Korea, Canada, America, Germany and Greece were contained in these eligible studies and Table 1 exhibited the major clinical characteristics, and Supplementary Table 2 showed other characteristics in detail. These enrolled patients were diagnosed with a variety of cancers, including cervical cancer, pancreatic cancer, oral squamous cell carcinoma, lung cancer, esophageal carcinoma, renal cell carcinoma, hepatocellular carcinoma, gastric cancer, osteosarcoma, urothelial cell carcinoma, thyroid cancer, melanoma, esophageal squamous cell carcinoma, ovarian cancer, prostate cancer. Seventeen studies (62.9%) were published in 2014 or later. The majority of studies (81.5%) reported on Asians, and five studies (18.5%) reported on Caucasians. Various cut-off values were shown in these literatures. B7-H4 were detected in tissue and blood, as each was expressed in 22 and 6 articles. The endpoints OS and DFS were respectively addressed in 25 and 5 studies. Twenty-two studies directly reported the HRs or RRs or ORs and the other articles’ parameters were estimated through survival curves indirectly.
Table 1: Characteristics of studies included in the meta-analysis
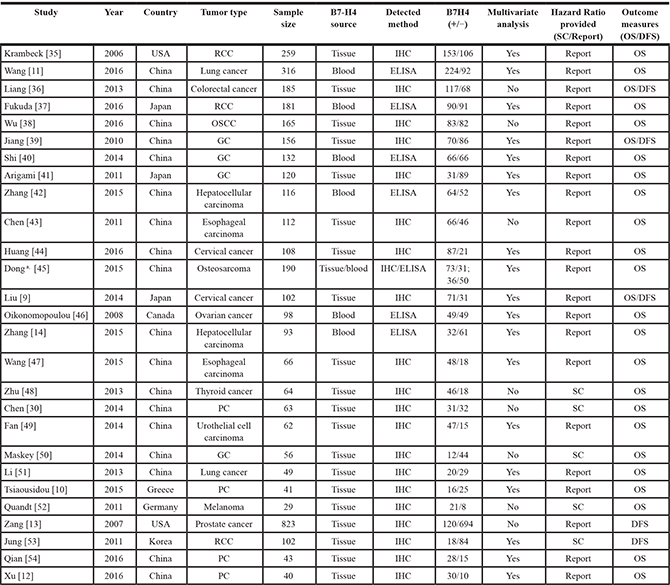
RCC: renal cell carcinoma; OSCC: oral squamous cell carcinoma; GC: gastric cancer; PC: pancreatic cancer; IHC: immunohistochemistry; ELISA: enzyme-linked immunosorbent assay; SC: survival curve.
a This article contained two cohorts, one cohort was detected from tissue, and the other was detected from blood.
Quality assessment
We conducted the quality assessment for each of 27 studies included in our meta-analysis. All studies were scored in accordance with the NOS and the quality score varied from 7 to 9, with a mean of 8.0. For more details, please see Supplementary Table 1. Better methodology could get a higher score and all the literatures were selected in the subsequent calculation.
Meta-analysis results
Overall survival
Twenty-five studies with 26 groups of people, including 2846 patients, provided proper information for OS analysis. This meta-analysis major results were shown in Table 2. We used the fixed-effects model to pool HRs because non-significant heterogeneity was found (I² = 0.0%, P = 0.632) among studies. The merged HR of 1.93 (95% CI 1.71–2.18, P < 0.001) demonstrated that high levels of B7-H4 expression were statistically associated with a worse prognosis (Figure 2). And the forest plots for the association between B7-H4 overexpression and prognosis were shown in Figure 2.
Table 2: Pooled hazard ratios for OS based on subgroup analyses
Outcome subgroup |
Number of patients |
Number of studies |
Fixed-effects model |
Heterogeneity |
|||
|---|---|---|---|---|---|---|---|
HR(95%CI) |
P value |
PSvalue |
I² |
P |
|||
Overall survival |
2846 |
25 |
1.93 (1.71–2.18) |
< 0.001 |
0.0% |
0.632 |
|
Ethnicity |
0.878 |
||||||
Asian |
2419 |
21 |
1.92 (1.68–2.19) |
< 0.001 |
0.0% |
0.58 |
|
Caucasian |
427 |
4 |
1.97 (1.46–2.66) |
< 0.001 |
0.0% |
0.399 |
|
Tumor type |
0.143 |
||||||
Renal cell carcinoma |
440 |
2 |
2.10 (1.13– 3.91) |
0.019 |
0.0% |
0.34 |
|
Pancreatic cancer |
187 |
4 |
2.69 (1.66–4.34) |
< 0.001 |
0.0% |
0.60 |
|
Lung cancer |
365 |
2 |
2.38 (1.54–3.69) |
< 0.001 |
10.4% |
0.29 |
|
Hepatocellular carcinoma |
209 |
2 |
2.22 (1.51– 3.27) |
< 0.001 |
0.0% |
0.62 |
|
Gastric cancer |
464 |
4 |
1.65 (1.27–2.14) |
< 0.001 |
0.0% |
0.84 |
|
Esophageal carcinoma |
178 |
2 |
2.01 (1.31–3.08) |
0.001 |
0.0% |
0.36 |
|
Cervical cancer |
210 |
2 |
9.20 (2.16–39.22) |
0.003 |
0.0% |
0.87 |
|
Others |
793 |
7 |
1.78 (1.47–2.14) |
< 0.001 |
0.0% |
0.52 |
|
Sample source |
0.613 |
||||||
Tissue |
1824 |
19 |
1.89 (1.63–2.20) |
< 0.001 |
9.0% |
0.35 |
|
Blood |
1022 |
7 |
2.00 (1.63–2.46) |
< 0.001 |
0.0% |
0.91 |
|
Analysis type |
0.639 |
||||||
Multivariate |
2210 |
18 |
1.94 (1.68–2.23) |
< 0.001 |
1.2% |
0.442 |
|
Univariate |
636 |
7 |
1.90 (1.50– 2.41) |
< 0.001 |
0% |
0.699 |
|
Source of HR |
0.638 |
||||||
SC |
460 |
4 |
2.53 (1.46–4.38) |
0.001 |
0.0% |
0.474 |
|
Report |
2386 |
21 |
1.90 (1.68–2.15) |
< 0.001 |
0.0% |
0.61 |
|
Sample size |
0.528 |
||||||
> 100 |
2056 |
13 |
1.88 (1.60–2.20) |
< 0.001 |
0.0% |
0.70 |
|
< 100 |
790 |
13 |
2.01 (1.66–2.42) |
< 0.001 |
6.1% |
0.39 |
|
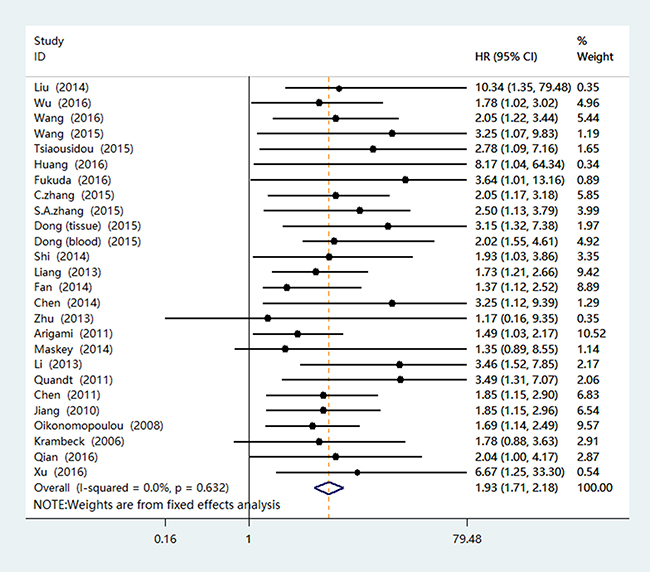
Figure 2: Forest plots of studies evaluating hazard ratios of B7-H4 overexpression in cancer patients.
Because of the unremarkable heterogeneity among studies, we conducted the subgroup analysis using the fixed-effects model on the basis of the tumor type, sample source, ethnicity, the source of HR, analysis type and sample size. As we could see in Figure 3, B7-H4 overexpression indicated a worse survival in patients with renal cell carcinoma (pooled HR = 2.10; 95% CI = 1.13–3.91; P = 0.019), pancreatic cancer (pooled HR = 2.69; 95% CI = 1.66–4.34; P < 0.001), lung cancer (pooled HR = 2.38; 95% CI = 1.54–3.69; P < 0.001), hepatocellular carcinoma (pooled HR = 2.22; 95% CI = 1.51–3.27; P < 0.001), gastric cancer (pooled HR = 1.65; 95% CI = 1.27–2.14; P < 0.001), esophageal carcinoma (pooled HR = 2.01; 95% CI = 1.31–3.08; P = 0.001), cervical cancer (pooled HR = 9.20; 95% CI = 2.16–39.22; P = 0.003) and others (pooled HR = 1.78; 95% CI = 1.47–2.14; P < 0.001). Elevated B7-H4 had negative effects on overall survival in Asian (pooled HR = 1.92; 95% CI = 1.68–2.19; P < 0.001) and Caucasian (pooled HR = 1.97; 95% CI = 1.46–2.66; P < 0.001) populations. In terms of specimen type, the overexpression of B7-H4 detected from tissue (pooled HR = 1.89; 95% CI = 1.63–2.20; P < 0.001) and blood (pooled HR = 2.00; 95%CI = 1.63–2.46; P < 0.001) both revealed poor prognosis in cancer patients. Pooled hazard ratio results were all > 1 based on ethnicity, tumor type, sample source, analysis type, source of HR and sample size (Table 2).
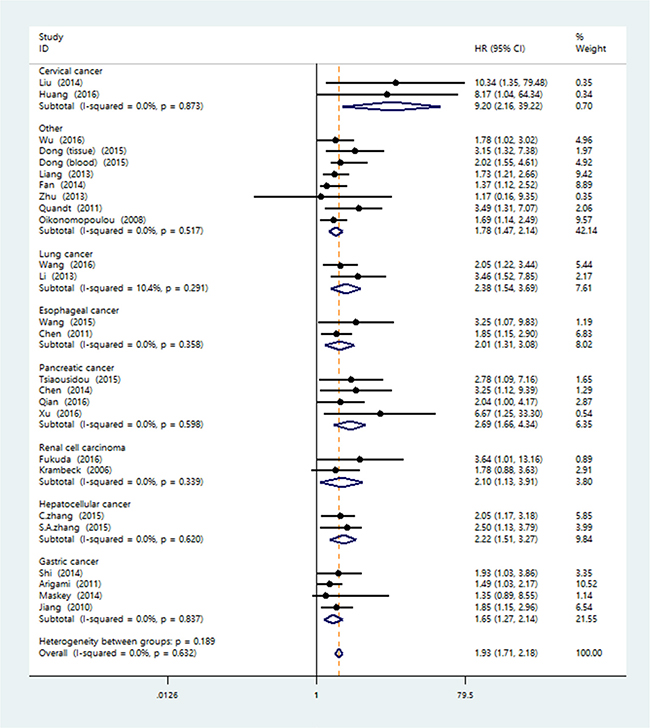
Figure 3: Forest plot of the association between B7-H4 overexpression and OS in a variety kinds of patients.
We conducted fixed-effects model sensitivity analysis via removing the literature data one by one, and showed no substantial influence. (Figure 4) A meta-regression was applied to assess the reason for the heterogeneity. Ethnicity (PS = 0.878), tumor type (PS = 0.143), sample size (PS = 0.528), sample source (PS = 0.613), analysis type (PS = 0.639) and source of HR (PS = 0.638) were not reasons for the heterogeneity. Multiple elements may contribute to the integral heterogeneity.
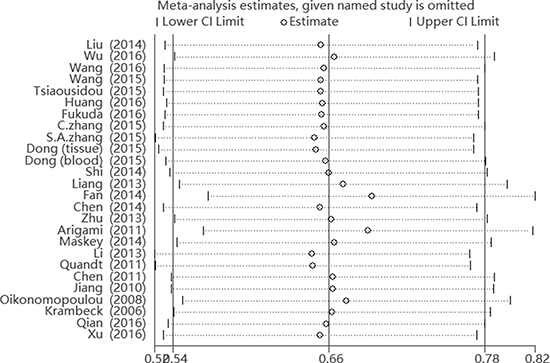
Figure 4: Sensitivity analysis of the meta-analysis of B7-H4 overexpression.
Publication bias
We measured the publication bias of articles through funnel plots, and Egger’s and Begg’s tests. In Figure 5, asymmetrical funnel plots were shown and reflected significant publication bias. Egger’s tests (P < 0.001) also proved this conclusion. In order to adjust the publication bias, we conducted a trim and fill analysis under fixed-effects model. Adjusted pooled HR for OS was 1.80 (95% CI = 1.61–2.03).
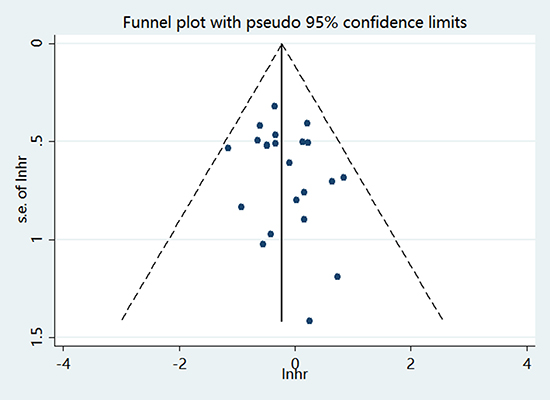
Figure 5: Funnel plot for publication bias assessment.
Disease free survival
Five studies suitable data pooled for DFS analysis which including a number of 1368 patients (Table 3). There was no obvious heterogeneity among the studies (I² = 54.8%, p = 0.065), because of this, fixed-effects model was used to pool HR for DFS. Analysis results revealed that higher levels of B7-H4 expression were associated with poorer DFS compared with the lower ones (pooled HR = 1.84; 95%CI = 1.46–2.33; P < 0.001). The forest plot of HRs for DFS was shown in Figure 6. Subgroup analysis based on ethnicity revealed B7-H4 induced a worsen DFS in Asian patients (HR = 2.20; 95% CI = 1.63–2.96; P < 0.001) than Caucasian patients (HR = 1.38; 95% CI = 0.94–2.02; P = 0.099). Overexpression B7-H4 had the worst effect in renal cell carcinoma with the highest pooled HR (HR = 9.62; 95% CI = 2.37–38.98; P = 0.002).
Table 3: Pooled hazard ratios for DFS based on subgroup analysis
Outcome subgroup |
Number of patients |
Number of studies |
Fixed-effects model |
Heterogeneity |
|||
|---|---|---|---|---|---|---|---|
HR(95%CI) |
P value |
Psvalue |
I² |
P |
|||
Disease free survival |
1368 |
5 |
1.84 (1.46–2.33) |
< 0.001 |
54.80% |
0.065 |
|
Ethnicity |
0.340 |
||||||
Asian |
545 |
4 |
2.20 (1.63–2.96) |
< 0.001 |
43.60% |
0.150 |
|
Caucasian |
823 |
1 |
1.38 (0.94–2.02) |
0.099 |
|||
Tumor type |
0.506 |
||||||
Cervical cancer |
102 |
1 |
3.19 (0.90–11.28) |
0.072 |
|||
Colorectal cancer |
185 |
1 |
1.83 (1.19–2.81) |
0.006 |
|||
Gastric cancer |
156 |
1 |
2.20 (1.39–3.49) |
0.001 |
|||
Renal cell carcinoma |
102 |
1 |
9.62 (2.37–38.98) |
0.002 |
|||
Prostate cancer |
823 |
1 |
1.38 (0.94–2.02) |
0.099 |
|||
HR = hazard ratio; CI = confidence interval; Ps = P for subgroup difference.
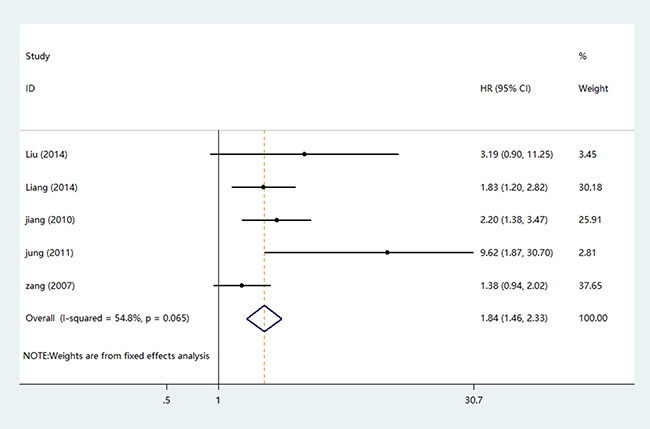
Figure 6: The forest plot of HRs for DFS.
DISCUSSION
The relationship between B7-H4 overexpression and prognosis in patients with cancer still remained not fully understood. In order to further investigate the connection between clinical outcome and B7-H4 expression, we conduct this review which is the first meta-analysis using the B7-H4 testing results which detected in blood and tissue.
B7-H4 is a newborn member of B7/CD28 family which has been identified in 2003 [4]. In the immune response, B7 superfamily has pivotal effect in regulating process, which is relevant to the initiation, development and recurrence of cancer [14, 15]. The biological mechanism of B7-H4 is mainly participate in tumor immune escape. Studies have shown that expression of B7-H4 within the tumor microenvironment can increase the function and quantity of FOXP3+ regulatory T cells (Treg cells) and facilitate the immune tolerance also infiltration capacity of Treg cells [16, 17]. By this means, Tregs are able to inhibit the proliferation of CD4+/CD8+ T cells and then suppress anti-tumor immune responds [18]. Several studies have shown that B7-H4 expression is negatively associated with the degree of tumor-infiltrating immune cells [19, 20]. It participates in the inhibition of immune cells infiltration, and this mechanism may be one of the reasons for the interpretation of tumor immune escape. Previous studies have been confirmed that the aberrant activation of Erk1/2 and AKT signaling pathway has an important affect in many tumor biological processes. In vivo and in vitro experiments confirmed that, B7-H4 silence increased the apoptosis of tumor cells, which was associated with the activity of caspase and decreased Erk1/2 and AKT phosphorylation [21, 22]. Zhang et al reported that B7-H4 can promote the G1/S phase transition and then enhance the tumor cell proliferation in vitro and tumorigenicity in vivo [23]. Another article confirmed that B7-H4 silence suppressed IL-6 secretion through JAK2/STAT3 inactivation and further downregulating cell proliferation [24]. For these reasons above, we believed that B7-H4 overexpression may predict a bad prognosis for cancer patients.
Blocking inhibiting signals for T cells in order to enhance the anti-tumor effects has become a promising cancer therapy, and it has been implemented through CTLA-4 and B7-H1 blockade in early years [5, 25, 26]. However, the CTLA-4 ligand expression location is limited to the antigen presenting cells in lymphoid tissue. The CTLA-4 functions are restricted to the early stage of the immune response. Compared with blocking the B7 family members which express precisely on various tumor, controlling the upstream stages in turn regulating effector T cells acting on peripheral tumors seems inefficient and imprecise [27]. B7-H1 is another potential immunotherapy target which is expressed on tumor and normal tissues, but B7-H4 can hardly be discovered in normal tissue and the expression pattern in tumor is wider than B7-H1[28, 29]. Chen et al. [30] also reported that B7-H4 overexpression was correlated with pancreatic cancer patients’ OS (P < 0.001), whereas the expression of B7-H1 didn’t (p = 0.089). For the reasons above, B7-H4 has the potential to become a new immunotherapy checkpoint for cancer treatment.
In our analysis, the pooled HR of B7-H4 on OS is 1.93 (HR = 1.93, 95% CI 1.71–2.18, P < 0.001), and HR = 1.84 on DFS (95% CI = 1.46–2.33; P < 0.001) which verified B7-H4 was related to a worse outcome for cancer patients. However, Zang et al. [13] reported that B7-H4 wasn’t an independent prognostic indicator, the reason why this phenomenon appeared may rely on the limited follow-up years for the long-survival period of prostate cancer patients. The previous meta-analysis which had investigated the high expression of B7-H4 influenced the prognosis of solid tumor patients also showed this trend as we illustrated [29]. While that article only included the samples derived from the tumor tissue and only contained 18 articles. Previous articles had shown the prognostic value of the blood-derived B7-H4. In addition, the blood-derived B7-H4 obtained by noninvasive methods was more clinically valuable than the tissue-derived B7-H4 obtained by invasive means. It was meaningful to conclude blood-derived B7-H4 to discussion. The present analysis had solved this question, and by subgroup analysis we found that the high expressions of blood-derived B7-H4 and tissue-derived B7-H4 were both independent prognostic indicators for poor OS (HR = 2.00 and HR = 1.89, respectively), also, high expression of B7-H4 in the blood could better reflect the poor prognosis of the disease. Therefore, it is the first meta-analysis on the relationship between B7-H4 detected in tissue/blood and OS/DFS and other clinical parameters.
However, several limitations still exist in our study. First, this meta-analysis was restricted to the published English Literatures, several studies couldn’t include because of its linguistic disparities or negative results which couldn’t be published. Second, although our analysis contained more articles and supplied the studies with B7-H4 expressed in blood compared with the previous one, the number is still inadequate, and more studies are needed to be included to make the results more credible. Third, the data of several studies were extracted from survival curves, the statistical error was inevitable which could affect the precision of results and the differences could be observed compared with the former article [29]. Fourth, the detection methods and cut-off values were varied, and the inconformity of these items may result in the heterogeneity of overall results. Unified detection methods and division criteria of high expression B7-H4 should be established to make it suitable for clinical applications. Fifth, although we did the subgroup analysis according to the ethnicity, tumor type, sample size, sample source, analysis type and source of HR, there were still other potential influencing factors to explain the variation of expression patterns in the same cancer types. However, due to the methodological reasons, many articles cannot provide the sufficient data (HR and corresponding 95% CI) to do the subgroup analysis on other factors. In our future research, we considered to narrow the scope of study (for example, conducting a single type of tumor study) to explore these differences. Last, the majority of samples were collected from Asian patients especially patients in China, so a wider sample collection is necessary to avoid the selection bias.
MATERIALS AND METHODS
The present meta-analysis was conducted in accordance with the Meta-analysis of Observational Studies in Epidemiology group (MOOSE) [31].
Literature search strategy
The relevant articles were systematically selected through PubMed, Embase and the Cochrane Library. We used the following strategies to select studies:” B7-H4 OR V-Set Domain-Containing T-Cell Activation Inhibitor 1 OR B7H4 OR B7x OR VTCN1 OR B7S1” (all fields) AND “Tumor OR Neoplasm OR Neoplasia OR Cancer OR carcinoma OR tumour OR leukemia OR myeloma OR lymphoma OR Malignancy OR Carcinomatosis OR Carcinomatoses” (all fields) AND “prognostic OR prognosis OR prognostication OR Prognoses OR survive OR Survived OR survival OR outcome” (all fields). Two authors (ZB. Meng and SK. Li) independently conducted the search. The last search was carried out on April 7, 2017.
Inclusion and exclusion criteria
Studies were qualified if they met the following criteria: (a) B7-H4 expressed in tumor tissue or blood; (b) the relationship between B7-H4 expression and tumor prognosis was examined; (c) provided sufficient and effective information to estimate the survival date such as: the hazard ratio (HR) or relative ratio (RR) or odds ratio (OR) with 95% confidence intervals (CI); (d) studies published in English. The literatures were excluded if they were duplicate reports, reviews, letters, conference abstracts, case reports, experimental and animal studies. When several research covered on the same patient cohort, the most recent literature was chosen.
Data extraction and quality assessment
Relevant studies were screened and required data were extracted independently by two researchers (ZB. Meng and FY. Wang). The following information was collected: first author; publication year; country; cancer type; sample size; gender; tumor stage; follow-up period; B7-H4 source (blood or tissue); detected methods; cut-off value; outcome measures; HR for survival outcome and corresponding 95% CI. If a study provided univariate and multivariate results both, considered the precision of data, the multivariate analysis would be selected. Some HRs and their 95% CI were not directly reported in the articles, we using the graphical data to extract information.
Two reviewers evaluated the quality of studies according to the Newcastle-Ottawa Quality Assessment Scale (NOS) [32]. The quality scores ranged from 0 to 9(9 was highest). The research with scores higher than 6 was considered as high quality.
Statistical analysis
The analysis was calculated by the STATA version 14.0 (Stata Corporation, College Station, TX, USA). The B7-H4 cut-off values classified cancer patients into high and low expression group. HRs with 95% CI were combined to assess the effective value on prognosis. Because the outcome of tumor is rare in all population and subgroups under review, the odds ratio(OR), rate ratio(RR), and hazard ratio(HR) can generally ignore the distinctions [33], the pooled ORs or RRs with 95%CI were appropriate for the assessment. If the above statistical variables were provided in the article, we used them directly. We also contacted the authors of the literature to obtain the relevant data. The rest of articles’ information we read the Kaplan-Meier survival curves through Engauge Digitizer version 9.8 to extract the data according to the method from the former literature [34]. This process was conducted by two independent researchers (ZB. Meng and YS Zhang) to avoid the reading deviation. > 1 HR represented a worse prognosis compared with a < 1 HR. Statistical heterogeneity across the eligible studies was inspected by processing the Chi-square test (assessing the P value) and calculating the I² statistic. If the I² was greater than 50% and P-value was less than 0.05, indicating a significant heterogeneity, a random-effects model (the DerSimonian-Laird method) was used. Otherwise the fixed-effects (Mante-Haenszel method) was applied to analyze the pooled HRs.
The sensitivity analyses were conducted to identify the effect of each study on the pooled result.
Publication bias assessment
We used funnel plots and Egger’s test to evaluate the publication bias. All P values were two-tailed and P was identified statistically significant if its value < 0.05. Graphical funnel plots were employed to qualitatively exhibit publication bias. And Egger’s test was used to demonstrate quantitatively.
Abbreviations
OS: overall survival; DFS: disease free survival; HR: hazard ratio; RR: rate ratio; OR: odds ratio; CI: confidence intervals; NOS: Newcastle-Ottawa Quality Assessment Scale; PS: P for subgroup difference; RCC: renal cell carcinoma; OSCC: oral squamous cell carcinoma; GC: gastric cancer; PC: pancreatic cancer; IHC: immunohistochemistry; ELISA: enzyme-linked immunosorbent assay; SC: survival curve.
Authors’ contributions
Z.M. and H.W. designed the study; Z.M. and F.W. wrote the main manuscript text; Z.M. and S.L. did the article search; Z.M. and Y.Z. analyzed the data; All authors reviewed the manuscript.
ACKNOWLEDGMENTS
The authors thank the staff from Pancreas surgery of Wuhan Union Hospital for their support during the study.
CONFLICTS OF INTEREST
The authors declare that there was not any financial or ethical conflicts of interest.
FUNDING
Supported by grants from the National Natural Science Foundation of China, No. 81372261. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
REFERENCES
1. Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA Cancer J Clin. 2015; 65:87–108. https://doi.org/10.3322/caac.21262.
2. Siegel RL, Miller KD, Jemal A. Cancer statistics, 2015. CA Cancer J Clin. 2015; 65:5–29. https://doi.org/10.3322/caac.21254.
3. Podojil JR, Miller SD. Potential targeting of B7-H4 for the treatment of cancer. Immunol Rev. 2017; 276:40–51. https://doi.org/10.1111/imr.12530.
4. Sica GL, Choi IH, Zhu G, Tamada K, Wang SD, Tamura H, Chapoval AI, Flies DB, Bajorath J, Chen L. B7-H4, a molecule of the B7 family, negatively regulates T cell immunity. Immunity. 2003; 18:849–61. doi https://doi.org/10.1016/S1074-7613(03)00152-3.
5. Brahmer JR, Tykodi SS, Chow LQ, Hwu WJ, Topalian SL, Hwu P, Drake CG, Camacho LH, Kauh J, Odunsi K, Pitot HC, Hamid O, Bhatia S, et al. Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med. 2012; 366:2455–65. https://doi.org/10.1056/NEJMoa1200694.
6. Ribas A, Camacho LH, Lopez-Berestein G, Pavlov D, Bulanhagui CA, Millham R, Comin-Anduix B, Reuben JM, Seja E, Parker CA, Sharma A, Glaspy JA, Gomez-Navarro J. Antitumor activity in melanoma and anti-self responses in a phase I trial with the anti-cytotoxic T lymphocyte-associated antigen 4 monoclonal antibody CP-675,206. J Clin Oncol. 2005; 23:8968–77. https://doi.org/10.1200/JCO.2005.01.109.
7. Twyman-Saint Victor C, Rech AJ, Maity A, Rengan R, Pauken KE, Stelekati E, Benci JL, Xu B, Dada H, Odorizzi PM, Herati RS, Mansfield KD, Patsch D, et al. Radiation and dual checkpoint blockade activate non-redundant immune mechanisms in cancer. Nature. 2015; 520:373–77. https://doi.org/10.1038/nature14292.
8. Jeon H, Vigdorovich V, Garrett-Thomson SC, Janakiram M, Ramagopal UA, Abadi YM, Lee JS, Scandiuzzi L, Ohaegbulam KC, Chinai JM, Zhao R, Yao Y, Mao Y, et al. Structure and cancer immunotherapy of the B7 family member B7x. Cell Reports. 2014; 9:1089–98. https://doi.org/10.1016/j.celrep.2014.09.053.
9. Liu W, Shibata K, Koya Y, Kajiyama H, Senga T, Yamashita M, Kikkawa F. B7-H4 overexpression correlates with a poor prognosis for cervical cancer patients. Mol Clin Oncol. 2014; 2:219–25. doi
10. Tsiaousidou A, Tsaroucha AK, Lambropoulou M, Pitiakoudis M, Polychronidis A, Chatzitheoklitos E, Romanidis K, Simopoulos C. Increased B7H4 tissue expression correlates with high CA19.9 serum levels and a worse prognosis of pancreatic adenocarcinoma. Clin Exp Med. 2016; 16:351–56. https://doi.org/10.1007/s10238-015-0352-7.
11. Wang W, Xu C, Wang Y, Yu L, Zhang X. Prognostic values of B7-H4 in non-small cell lung cancer. Biomarkers. 20162016; Jun 20:1-16. [Epub ahead of print].
12. Xu H, Chen X, Tao M, Chen K, Chen C, Xu G, Li W, Yuan S, Mao Y. B7-H3 and B7-H4 are independent predictors of a poor prognosis in patients with pancreatic cancer. Oncol Lett. 2016; 11:1841–46.
13. Zang X, Thompson RH, Al-Ahmadie HA, Serio AM, Reuter VE, Eastham JA, Scardino PT, Sharma P, Allison JP. B7-H3 and B7x are highly expressed in human prostate cancer and associated with disease spread and poor outcome. Proc Natl Acad Sci USA. 2007; 104:19458–63. https://doi.org/10.1073/pnas.0709802104.
14. Zhang C, Li Y, Wang Y. Diagnostic value of serum B7-H4 for hepatocellular carcinoma. J Surg Res. 2015; 197:301–06. https://doi.org/10.1016/j.jss.2015.04.034.
15. He C, Qiao H, Jiang H, Sun X. The inhibitory role of b7-h4 in antitumor immunity: association with cancer progression and survival. Clin Dev Immunol. 2011; 2011: 695834. https://doi.org/10.1155/2011/695834.
16. Zhao LW, Li C, Zhang RL, Xue HG, Zhang FX, Zhang F, Gai XD. B7-H1 and B7-H4 expression in colorectal carcinoma: correlation with tumor FOXP3 (+) regulatory T-cell infiltration. Acta Histochem. 2014; 116:1163–68. https://doi.org/10.1016/j.acthis.2014.06.003.
17. Podojil JR, Liu LN, Marshall SA, Chiang MY, Goings GE, Chen L, Langermann S, Miller SD. B7-H4Ig inhibits mouse and human T-cell function and treats EAE via IL-10/Treg-dependent mechanisms. J Autoimmun. 2013; 44:71–81. https://doi.org/10.1016/j.jaut.2013.04.001.
18. Kristensen NN, Schmidt EG, Rasmussen S, Balk-Møller E, Claesson MH. B7-H4-Ig treatment of normal mice changes lymphocyte homeostasis and increases the potential of regulatory T cells. Immunopharmacol Immunotoxicol. 2013; 35:505–13. https://doi.org/10.3109/08923973.2013.810642.
19. Sun Y, Wang Y, Zhao J, Gu M, Giscombe R, Lefvert AK, Wang X. B7-H3 and B7-H4 expression in non-small-cell lung cancer. Lung Cancer. 2006; 53:143–51. https://doi.org/10.1016/j.lungcan.2006.05.012.
20. Mugler KC, Singh M, Tringler B, Torkko KC, Liu W, Papkoff J, Shroyer KR. B7-h4 expression in a range of breast pathology: correlation with tumor T-cell infiltration. Appl Immunohistochem Mol Morphol. 2007; 15:363–70. https://doi.org/10.1097/01.pai.0000213159.79557.71.
21. Qian Y, Hong B, Shen L, Wu Z, Yao H, Zhang L. B7-H4 enhances oncogenicity and inhibits apoptosis in pancreatic cancer cells. Cell Tissue Res. 2013; 353:139–51. https://doi.org/10.1007/s00441-013-1640-8.
22. Zhang X, Cai L, Zhang G, Shen Y, Huang J. B7-H4 promotes tumor growth and metastatic progression in lung cancer by impacting cell proliferation and survival. Oncotarget. 2017; 8:18861–71. https://doi.org/10.18632/oncotarget.14475.
23. Zhang L, Wu H, Lu D, Li G, Sun C, Song H, Li J, Zhai T, Huang L, Hou C, Wang W, Zhou B, Chen S, et al. The costimulatory molecule B7-H4 promote tumor progression and cell proliferation through translocating into nucleus. Oncogene. 2013; 32:5347–58. https://doi.org/10.1038/onc.2012.600.
24. Chen X, Wang L, Wang W, Zhao L, Shan B. B7-H4 facilitates proliferation of esophageal squamous cell carcinoma cells through promoting interleukin-6/signal transducer and activator of transcription 3 pathway activation. Cancer Sci. 2016; 107:944–54. https://doi.org/10.1111/cas.12949.
25. Phan GQ, Yang JC, Sherry RM, Hwu P, Topalian SL, Schwartzentruber DJ, Restifo NP, Haworth LR, Seipp CA, Freezer LJ, Morton KE, Mavroukakis SA, Duray PH, et al. Cancer regression and autoimmunity induced by cytotoxic T lymphocyte-associated antigen 4 blockade in patients with metastatic melanoma. Proc Natl Acad Sci USA. 2003; 100:8372–77. https://doi.org/10.1073/pnas.1533209100.
26. Hodi FS, Mihm MC, Soiffer RJ, Haluska FG, Butler M, Seiden MV, Davis T, Henry-Spires R, MacRae S, Willman A, Padera R, Jaklitsch MT, Shankar S, et al. Biologic activity of cytotoxic T lymphocyte-associated antigen 4 antibody blockade in previously vaccinated metastatic melanoma and ovarian carcinoma patients. Proc Natl Acad Sci USA. 2003; 100:4712–17. https://doi.org/10.1073/pnas.0830997100.
27. Chambers CA, Kuhns MS, Egen JG, Allison JP. CTLA-4-mediated inhibition in regulation of T cell responses: mechanisms and manipulation in tumor immunotherapy. Annu Rev Immunol. 2001; 19:565–94. https://doi.org/10.1146/annurev.immunol.19.1.565.
28. Choi IH, Zhu G, Sica GL, Strome SE, Cheville JC, Lau JS, Zhu Y, Flies DB, Tamada K, Chen L. Genomic organization and expression analysis of B7-H4, an immune inhibitory molecule of the B7 family. J Immunol. 2003; 171:4650–54. doi https://doi.org/10.4049/jimmunol.171.9.4650.
29. Song X, Shao Y, Gu W, Xu C, Mao H, Pei H, Jiang J. Prognostic role of high B7-H4 expression in patients with solid tumors: a meta-analysis. Oncotarget. 2016; 7:76523–33. https://doi.org/10.18632/oncotarget.8598.
30. Chen Y, Sun J, Zhao H, Zhu D, Zhi Q, Song S, Zhang L, He S, Kuang Y, Zhang Z, Li D. The coexpression and clinical significance of costimulatory molecules B7-H1, B7-H3, and B7-H4 in human pancreatic cancer. Onco Targets Ther. 2014; 7:1465–72. https://doi.org/10.2147/OTT.S66809.
31. Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA. 2000; 283:2008–12. https://doi.org/10.1001/jama.283.15.2008.
32. Wells G, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Ottawa Hospital Research Institute; 2011. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp.
33. Greenland S. Quantitative methods in the review of epidemiologic literature. Epidemiol Rev. 1987; 9:1–30. doi https://doi.org/10.1093/oxfordjournals.epirev.a036298.
34. Tierney JF, Stewart LA, Ghersi D, Burdett S, Sydes MR. Practical methods for incorporating summary time-to-event data into meta-analysis. Trials. 2007; 8:16. https://doi.org/10.1186/1745-6215-8-16.
35. Krambeck AE, Thompson RH, Dong H, Lohse CM, Park ES, Kuntz SM, Leibovich BC, Blute ML, Cheville JC, Kwon ED. B7-H4 expression in renal cell carcinoma and tumor vasculature: associations with cancer progression and survival. Proc Natl Acad Sci USA. 2006; 103:10391–96. https://doi.org/10.1073/pnas.0600937103.
36. Liang M, Li J, Wang D, Li S, Sun Y, Sun T, Zhang J, Chen X, Li Q, Sun S. T-cell infiltration and expressions of T lymphocyte co-inhibitory B7-H1 and B7-H4 molecules among colorectal cancer patients in northeast China’s Heilongjiang province. Tumour Biol. 2014; 35:55–60. https://doi.org/10.1007/s13277-013-1006-6.
37. Fukuda T, Kamai T, Masuda A, Nukui A, Abe H, Arai K, Yoshida K. Higher preoperative serum levels of PD-L1 and B7-H4 are associated with invasive and metastatic potential and predictable for poor response to VEGF-targeted therapy and unfavorable prognosis of renal cell carcinoma. Cancer Med. 2016; 5:1810–20. https://doi.org/10.1002/cam4.754.
38. Wu L, Deng WW, Yu GT, Mao L, Bu LL, Ma SR, Liu B, Zhang WF, Sun ZJ. B7-H4 expression indicates poor prognosis of oral squamous cell carcinoma. Cancer Immunol Immunother. 2016; 65:1035–45. https://doi.org/10.1007/s00262-016-1867-9.
39. Jiang J, Zhu Y, Wu C, Shen Y, Wei W, Chen L, Zheng X, Sun J, Lu B, Zhang X. Tumor expression of B7-H4 predicts poor survival of patients suffering from gastric cancer. Cancer Immunol Immunother. 2010; 59:1707–14. https://doi.org/10.1007/s00262-010-0900-7.
40. Shi H, Ji M, Wu J, Zhou Q, Li X, Li Z, Zheng X, Xu B, Zhao W, Wu C, Jiang J. Serum B7-H4 expression is a significant prognostic indicator for patients with gastric cancer. World J Surg Oncol. 2014; 12:188. https://doi.org/10.1186/1477-7819-12-188.
41. Arigami T, Uenosono Y, Ishigami S, Hagihara T, Haraguchi N, Natsugoe S. Clinical significance of the B7-H4 coregulatory molecule as a novel prognostic marker in gastric cancer. World J Surg. 2011; 35:2051–57. https://doi.org/10.1007/s00268-011-1186-4.
42. Zhang SA, Wu ZX, Zhang X, Zeng ZY, Li DL. Circulating B7-H4 in serum predicts prognosis in patients with hepatocellular carcinoma. Genet Mol Res. 2015; 14:13041–48. https://doi.org/10.4238/2015.October.21.25.
43. Chen LJ, Sun J, Wu HY, Zhou SM, Tan Y, Tan M, Shan BE, Lu BF, Zhang XG. B7-H4 expression associates with cancer progression and predicts patient’s survival in human esophageal squamous cell carcinoma. Cancer Immunol Immunother. 2011; 60:1047–55. https://doi.org/10.1007/s00262-011-1017-3.
44. Huang C, Zhou L, Chang X, Pang X, Zhang H, Zhang S. B7-H3, B7-H4, Foxp3 and IL-2 expression in cervical cancer: associations with patient outcome and clinical significance. Oncol Rep. 2016; 35:2183–90.
45. Dong Q, Ma X. B7-H4 expression is associated with tumor progression and prognosis in patients with osteosarcoma. Biomed Res Int. 2015; 2015:156432. https://doi.org/10.1155/2015/156432.
46. Oikonomopoulou K, Li L, Zheng Y, Simon I, Wolfert RL, Valik D, Nekulova M, Simickova M, Frgala T, Diamandis EP. Prediction of ovarian cancer prognosis and response to chemotherapy by a serum-based multiparametric biomarker panel. Br J Cancer. 2008; 99:1103–13. https://doi.org/10.1038/sj.bjc.6604630.
47. Wang L, Cao NN, Wang S, Man HW, Li PF, Shan BE. Roles of coinhibitory molecules B7-H3 and B7-H4 in esophageal squamous cell carcinoma. Tumour Biol. 2016; 37:2961–71. https://doi.org/10.1007/s13277-015-4132-5.
48. Zhu J, Chu BF, Yang YP, Zhang SL, Zhuang M, Lu WJ, Liu YB. B7-H4 expression is associated with cancer progression and predicts patient survival in human thyroid cancer. Asian Pac J Cancer Prev. 2013; 14:3011–15. doi https://doi.org/10.7314/APJCP.2013.14.5.3011.
49. Fan M, Zhuang Q, Chen Y, Ding T, Yao H, Chen L, He X, Xu X. B7-H4 expression is correlated with tumor progression and clinical outcome in urothelial cell carcinoma. Int J Clin Exp Pathol. 2014; 7:6768–75. doi
50. Maskey N, Li K, Hu M, Xu Z, Peng C, Yu F, Cao H, Chen J, Li Y, Yang G. Impact of neoadjuvant chemotherapy on lymphocytes and co-inhibitory B7-H4 molecule in gastric cancer: low B7-H4 expression associates with favorable prognosis. Tumour Biol. 2014; 35:11837–43. https://doi.org/10.1007/s13277-014-2410-2.
51. Li ZY, Zhang XH, Chen Y, Guo JG, Sai K, Yang QY, Chen ZP, Mou YG. Clinical significance of B7-H4 expression in matched non-small cell lung cancer brain metastases and primary tumors. Onco Targets Ther. 2013; 6:869–75. https://doi.org/10.2147/OTT.S48085.
52. Quandt D, Fiedler E, Boettcher D, Marsch WC, Seliger B. B7-h4 expression in human melanoma: its association with patients’ survival and antitumor immune response. Clin Cancer Res. 2011; 17:3100–11. https://doi.org/10.1158/1078-0432.CCR-10-2268.
53. Jung SG, Choi KU, Lee SD, Lee ZZ, Chung MK. The relationship between B7-H4 expression and clinicopathological characteristics in clinical stage T1 conventional renal cell carcinoma. Korean J Urol. 2011; 52:90–95. https://doi.org/10.4111/kju.2011.52.2.90.
54. Qian Y, Sang Y, Wang FX, Hong B, Wang Q, Zhou X, Weng T, Wu Z, Zheng M, Zhang H, Yao H. Prognostic significance of B7-H4 expression in matched primary pancreatic cancer and liver metastases. Oncotarget. 2016; 7:72242–49. https://doi.org/10.18632/oncotarget.12665.

