Introduction
The insulin-like growth factor (IGF) axis is involved in many cancer types. However, the prognostic importance of the IGF-receptor family in breast cancer is unclear. The signaling network is complex and involves both the IGF-I receptor (IGF1R) and the insulin receptor (InsR). These receptors can form both homo- and heterodimer (hybrid) receptors [1]. Upon ligand-mediated activation, the receptors become phosphorylated at various tyrosine-kinase residues, which initiate further downstream signal transduction involving the phosphatidylinositol 3-kinase (PI3K) and mitogen activated protein kinase (MAPK) pathways. Furthermore, there is crosstalk between the IGF-signaling network and other signaling pathways e.g. the estrogen receptor (ER) [2-4].
Targeting the IGF signaling pathway was suggested by leading breast cancer experts as a promising approach to find more effective treatment regimens [5]. Several clinical trials with compounds targeting either IGF ligands or receptor have shown promising results in phase I. However, results from phases II and III in unselected patients have not been as encouraging [6]. This could be a consequence of treating unselected groups of patients and a reflection of the complexity of feedback loops and crosstalk with other signaling pathways [3]. It is therefore desirable to find biomarkers that can predict which patients could benefit from IGF-targeting therapies such as small-molecule inhibitors, anti-receptor antibodies, and anti-ligand antibodies [1, 7-11].
The IGF signaling network may also confer resistance to other treatments including HER2-targeted therapy, radiotherapy, endocrine therapy, and chemotherapy [12-15]. The expression patterns of IGF1R, InsR and pIGF1R are therefore important to elucidate in this complex network, its involvement in breast cancer, and its association with prognosis in different treatment groups. There are several reports addressing the prognostic value of these markers individually [16-19]. However, to our knowledge the combination of these three markers regarding prognosis has not been investigated. Given that signaling can occur via both hetero- and homodimers of IGF1R and InsR, the expression of both receptors needs to be investigated. In this study, the expression of IGF1R, InsR and pIGF1R/InsR was evaluated in tumors from 946 primary breast cancer patients in a prospective cohort. We hypothesized that a combination of IGF1R, InsR and pIGF1R/InsR may better identify subgroups of patients with poor outcome than either marker alone, and that tumors with IGF1Rstrong/InsRmod/strong/pIGF1R/InsRpos expression are associated with worse prognosis and involved in treatment resistance. The aim was to clarify the importance of these three markers individually and combined regarding risk for breast cancer events, distant metastasis, and overall survival in different treatment groups.
Results
IGF1R, InsR and pIGF1R/InsR in relation to tumor and patient characteristics
The distribution of the staining intensities for IGF1R (n = 923), InsR (n = 900) and pIGF1R/InsR (n = 904) is illustrated in Figure 1A. There were significant correlations between all markers for both cytoplasmic and membrane staining intensities (all P-values ≤0.021). For the combined dichotomized cytoplasmic intensity and membrane expression there was only a significant correlation between InsR and pIGF1R/InsR expressions (rS = 0.16, P<0.001; Figure 1B). The cut-off determination for prognostically relevant staining intensities for each marker was determined using Kaplan-Meier curves (Figure 2A). Groups where the curves crossed over were combined into one group (Figure 2B). The final dichotomized groups were based on both cytoplasmic and membrane staining (Figure 2C). For IGF1R and pIGF1R/InsR the dichotomized groups remained essentially the same after addition of membrane staining; IGF1Rnot strong (95.0%) and IGF1Rstrong (5.0%); pIGF1R/InsRneg (17.0%) and pIGF1R/InsRpos (83.0%). There was no clear separation of tumors stained for InsR and these were therefore grouped into InsRneg/weak and InsRmod/strong. The number of patients with InsRmod/strong tumors increased substantially after addition of membrane staining; InsRneg/weak (18.0%) and InsRmod/strong (82.0%).
Associations between the evaluated markers and tumor and patient characteristics are shown in Table 1. IGF1Rstrong tumor expression was associated with larger invasive tumor size (P = 0.001), increasing axillary lymph node involvement (P = 0.040), and higher histological grade (P = 0.013). IGF1Rstrong expression was further significantly associated with triple-negative tumors (P = 0.014), whereas triple negativity was significantly associated with InsRneg/weak (P = 0.021) and pIGF1R/InsRneg (P = 0.014) expression. Both InsRmod/strong and pIGF1R/InsRpos expression were associated with ER+ status (P = 0.005 and P = 0.021, respectively). IGF1Rstrong expression was associated with a higher frequency of patients receiving any endocrine treatment (P = 0.014), and specifically tamoxifen (P = 0.029), compared with IGF1Rnot strong expression. In contrast, a larger percentage of patients with tumors with InsRneg/weak expression had received tamoxifen treatment (P = 0.029), compared with patients with tumors with InsRmod/high expression. Height was the only anthropometric factor associated with InsR (P = 0.004). None of the other investigated anthropometric factors were associated with any of the other markers.
Table 1: Tumor and patient characteristics in relation to tumor-specific expression of IGF1R, InsR and pIGF1R/InsR
IGF1R |
InsR |
pIGF1R/InsR |
||||
Not strong n=877 (95%) n (%), Median (IQR) or % |
Strong n=46 (5%) n (%), Median (IQR) or % |
Negative/Weak n=162 (18%) n (%), Median (IQR) or % |
Moderate/Strong n=738 (82%) n (%), Median (IQR) or % |
Negative n=154 (17%) n (%), Median (IQR) or % |
Positive n=750 (83%) n (%), Median (IQR) or % |
|
Tumor characteristics |
||||||
Invasive tumor size |
||||||
1 (≤20 mm) |
647 (73.8) |
24 (52.2) |
114 (70.4) |
537 (72.8) |
119 (77.3) |
532 (70.9) |
2+ (≥21 mm or skin or muscular involvement independent of size) |
230 (26.2) |
22 (47.8) |
48 (29.6) |
201 (27.2) |
35 (22.7) |
218 (29.1) |
Axillary lymph node involvement |
||||||
0 |
537 (61.4) |
23 (50.0) |
94 (58.0) |
453 (61.5) |
86 (56.2) |
464 (61.9) |
1-3 |
264 (30.2) |
15 (32.6) |
46 (28.4) |
227 (30.8) |
47 (30.7) |
227 (30.3) |
≥4 |
74 (8.5) |
8 (17.4) |
22 (13.6) |
56 (7.6) |
20 (13.1) |
58 (7.7) |
Missing |
2 |
0 |
0 |
2 |
1 |
1 |
Histologic grade |
||||||
I |
224 (25.6) |
6 (13.0) |
37 (22.8) |
181 (24.6) |
39 (25.3) |
185 (24.7) |
II |
436 (49.8) |
22 (47.8) |
86 (53.1) |
366 (49.7) |
71 (46.1) |
376 (50.2) |
III |
216 (24.7) |
18 (39.1) |
39 (24.1) |
190 (25.8) |
44 (28.6) |
188 (25.1) |
Hormone receptor status |
||||||
ER+ |
775 (88.6) |
38 (82.6) |
132 (81.5) |
658 (89.4) |
126 (82.4) |
667 (89.1) |
PR+ |
630 (72.0) |
28 (60.9) |
114 (70.4) |
523 (71.1) |
110 (71.9) |
529 (70.6) |
Missing |
2 |
0 |
0 |
2 |
1 |
1 |
HER2 amplificationa |
67 (11.4) |
3 (9.7) |
8 (10.5) |
57 (10.9) |
9 (14.1) |
60 (11.0) |
Missing |
288 |
15 |
86 |
213 |
90 |
203 |
Triple-negative (ER-PR-HER2-) |
46 (7.3) |
6 (19.4) |
12 (14.8) |
41 (7.3) |
11 (15.1) |
40 (6.9) |
Missing |
243 |
15 |
81 |
174 |
81 |
169 |
Treatment by last follow-upb |
||||||
Ever chemotherapy |
219 (25.0) |
15 (32.6) |
41 (25.3) |
187 (25.3) |
34 (22.1) |
196 (26.1) |
Ever radiotherapy |
564 (64.3) |
28 (60.9) |
103 (63.6) |
471 (63.8) |
92 (59.7) |
485 (64.7) |
ER+ only |
||||||
Ever endocrine therapy |
605 (78.0) |
36 (94.7) |
105 (79.5) |
518 (78.6) |
100 (79.4) |
525 (78.6) |
Ever tamoxifen |
454 (58.5) |
29 (76.3) |
90 (68.2) |
382 (58.0) |
82 (65.1) |
392 (58.7) |
Ever aromatase inhibitor |
300 (38.7) |
17 (44.7) |
49 (37.1) |
259 (39.3) |
53 (42.1) |
255 (38.2) |
Patient characteristics |
||||||
Age at diagnosis, years |
61.1 (52.5-68.0) |
60.8 (52.0-69.1) |
60.2 (50.2-66.9) |
61.4 (53.0-68.2) |
61.2 (54.6-69.4) |
61.1 (52.3-67.9) |
Weight, kg |
70.0 (62.0-79.0) |
66.5 (58.3-74.0) |
68.0 (61.0-76.0) |
70.0 (62.0-79.6) |
70.0 (62.0-79.0) |
70.0 (62.0-78.5) |
Missing |
22 |
2 |
3 |
20 |
3 |
19 |
Height, m |
1.66 (1.62-1.70) |
1.64 (1.60-1.68) |
1.64 (1.60-1.68) |
1.66 (1.62-1.70) |
1.65 (1.61-1.69) |
1.66 (1.62-1.70) |
Missing |
22 |
2 |
3 |
20 |
2 |
20 |
BMI, kg/m2 |
25.2 (22.6-28.5) |
24.4 (21.8-27.7) |
25.0 (22.9-27.7) |
25.2 (22.4-28.7) |
25.3 (22.7-28.6) |
25.1 (22.5-28.3) |
Missing |
24 |
2 |
3 |
22 |
3 |
21 |
Waist-to-hip ratio, m/m |
0.86 (0.81-0.90) |
0.87 (0.82-0.90) |
0.85 (0.80-0.90) |
0.86 (0.81-0.91) |
0.84 (0.80-0.90) |
0.86 (0.81-0.90) |
Missing |
31 |
4 |
3 |
29 |
4 |
29 |
Total breast volume ≥850 mL |
424 (57.0) |
21 (61.8) |
83 (61.5) |
349 (55.7) |
78 (60.0) |
359 (56.7) |
Missing |
133 |
12 |
27 |
111 |
24 |
117 |
Abbreviations: IQR, interquartile range
a HER2 was routinely analyzed in patients <70 years with invasive tumors as of November 2005.
b Patients may have received more than one type of treatment prior to any event.
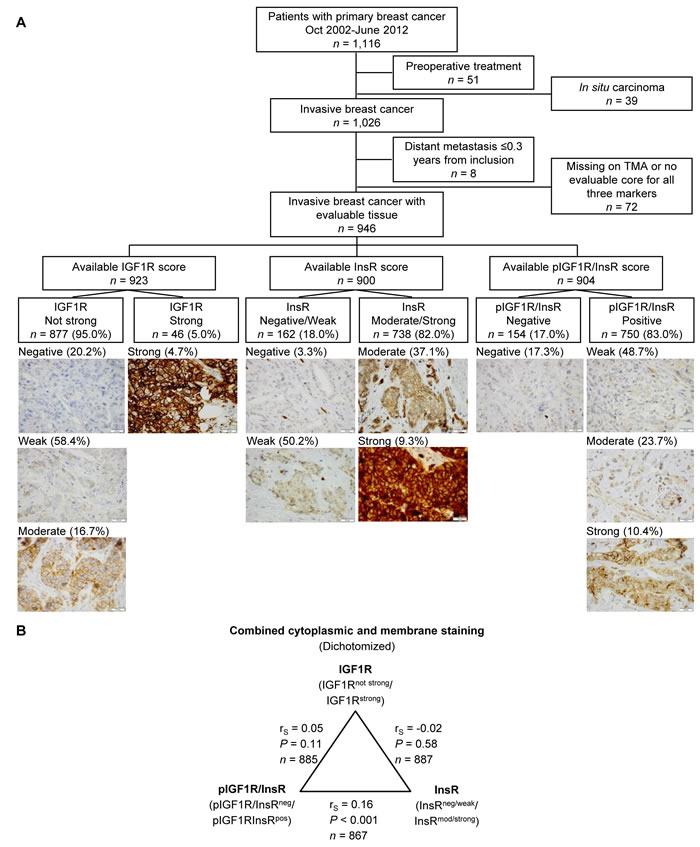
Figure 1: A. Flow chart of study population and division of evaluated markers. Total available staining scores for each group are based on combined cytoplasmic and membrane staining. Representative images for IGF1R, InsR and pIGF1R/InsR are shown (scale bar = 20 μm). The corresponding percentages of tumors with different staining intensities indicate cytoplasmic staining only. B. Correlations between IGF1R, InsR and pIGF1R/InsR for combined cytoplasmic and membrane staining.
The prognostic impact of individual markers
Patients were followed for up to 11 years with a median follow-up of 5.0 years for patients still at risk. Of the 946 patients, 115 had had any breast cancer event of which 72 patients had a distant metastasis and 91 patients died due to any cause. Of the 91 patients who died, 55 patients had had a reported breast cancer event prior to death.
Patients with tumors with IGF1Rstrong expression was significantly associated with breast cancer events (LogRank P = 0.040; Figure 2C). However, IGF1Rstrong expression was not an independent prognostic marker for any breast cancer event, adjusted HR (HRadj) (1.60; 95% CI 0.82-3.07), distant metastasis, or overall survival in multivariable Cox regression analyses.
InsR did not provide any significant prognostic information regarding event-free survival (Figure 2C) or distant metastasis. However, patients with InsRmod/strong expressing tumors had a borderline decreased risk of death due to any cause after adjusting for other prognostic factors and tumor storage time, HRadj (0.66; 95% CI 0.41-1.06).
Patients with pIGF1R/InsRpos tumors had significantly longer event-free survival compared to patients with pIGF1R/InsRneg tumors (LogRank P = 0.020; Figure 2C). Multivariable analysis revealed that pIGF1R/InsR did not provide independent prognostic information regarding event-free survival after adjustment for other prognostic factors and tumor storage time, HRadj (0.70; 95% CI 0.46-1.06). Distant metastasis-free survival and overall survival were not associated with pIGF1R/InsR in the multivariable models.
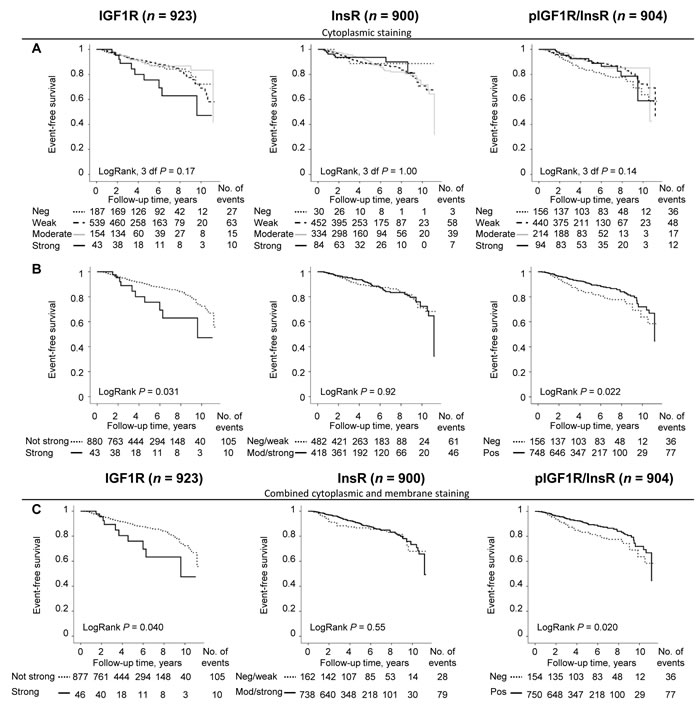
Figure 2: Cut-off determination based on the prognostic significance of IGF1R, InsR and pIGF1R/InsR using Kaplan-Meier plots. Curves representing A. four different cytoplasmic staining intensities, B. dichotomized groups after merging overlapping cytoplasmic staining intensity curves, and C. combined cytoplasmic and membrane staining as individual prognostic markers in relation to event-free survival.
The prognostic significance of combining IGF1R, InsR and pIGF1R/InsR
The combined expression of IGF1R, InsR, and pIGF1R/InsR was investigated and resulted in eight combinations with different impacts on patient prognosis. In total, 858 tumors were successfully scored for all markers. Patients having IGF1Rstrong/InsRmod/strong/pIGF1R/InsRpos tumors had significantly shorter event-free survival compared with all other groups (LogRank 7 df, P = 0.019; Figure 3A). A non-significant 2-fold increased risk for breast cancer events was observed among patients with IGF1Rstrong/InsRmod/strong/pIGF1R/InsRpos tumors compared with all other groups after adjustment for other prognostic factors and tumor storage time, HRadj (2.00; 95% CI 0.96-4.18).
Since IGF1R and pIGF1R/InsR provided individual prognostic information in the univariable models, these two markers were combined. Patients with tumors with both IGF1Rstrong and pIGF1R/InsRpos expression had the highest risk for events, followed by tumors with IGF1Rnot strong and pIGF1R/InsRneg expression, while patients with tumors with IGF1Rnot strong and pIGF1R/InsRpos expression had a better prognosis (LogRank 3 df, P = 0.008; Figure 3B). There were only four patients with IGF1Rstrong expressing tumors in combination with and pIGF1R/InsRneg. While InsR did not provide any individual prognostic information regarding breast cancer events, there was a significant effect modification of InsR on the association between the combined IGF1R and pIGF1R/InsR markers and event-free survival (Pinteraction = 0.041). Further stratification by InsR expression revealed that while no association was seen in InsRneg/weak (LogRank 3 df, P = 0.94), InsRmod/strong expression was required to distinguish between the combinations of IGF1R and pIGF1R/InsR on event-free survival (LogRank 3 df, P = 0.002; Figure 3B).
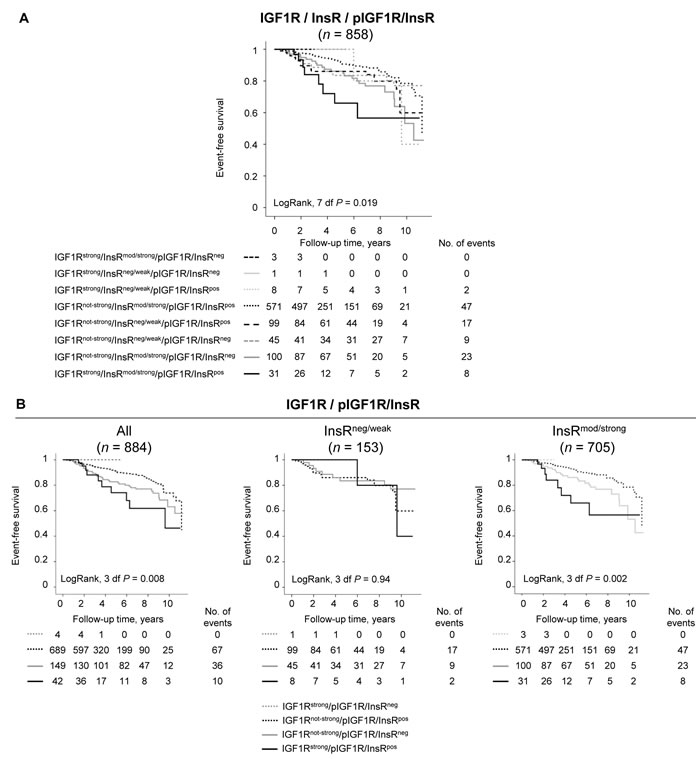
Figure 3: The prognostic value of various IGF1R, InsR and pIGF1R/InsR combinations. Kaplan-Meier curves showing event-free survival in relation to A. the eight different IGF1R, InsR, and pIGF1R/InsR combinations, and B. the four different IGF1R and pIGF1R/InsR combinations among all patients or stratified according to InsR status, (pinteraction = 0.041).
The prognostic impact of IGF1R, InsR and pIGF1R/InsR in different treatment groups
The expression of the three markers in relation to response to endocrine treatment, radiotherapy and chemotherapy was assessed due to the reported influence of IGF-signaling on cancer treatments. Any breast cancer event was used as a marker for poor treatment response.
Neither InsR nor pIGF1R/InsR was associated with outcome among endocrine-treated patients with ER+ tumors, irrespective of type of endocrine treatment. However, there was a borderline significant 2-fold increased risk for recurrence among the patients with ER+ tumors who ever received any type of endocrine treatment and had IGF1Rstrong tumor expression compared with IGF1Rnot strong tumor expression, HRadj (2.07; 95% CI 0.98-4.37) adjusted for prognostic markers and treatment with chemotherapy and radiotherapy. Since aromatase inhibitor (AIs) are mainly offered to postmenopausal women, patients were stratified according to age. Among AI- but not tamoxifen (TAM)-treated patients ≥50 years (n = 148), IGF1Rstrong expression was associated with increased risk of breast cancer events, HRadj (4.45; 95% CI 1.12-17.73). This association was not significant in patients ≥50 years who received both AI and TAM switch treatment (n = 142), HRadj (2.33; 95% CI 0.42-12.99), and not observed in patients ≥50 years treated with TAM but not AIs (n = 246), HRadj (0.80; 95% CI 0.10-6.58). In contrast, among the younger TAM-treated patients <50 years (n = 107) with or without AIs, IGF1Rstrong expression was weakly associated with increased risk of breast cancer events, HRadj (3.91; 95% CI 0.67-22.83). The association appeared to be driven by the group of patients who received TAM but not AIs (n = 85), HRadj (14.29; 95% CI 1.82-112.25). There were too few AI-treated patients <50 years to allow for separate analyses. Endocrine treatment response was not associated with any of the other markers individually or combined. Neither IGF1R, InsR nor pIGF1R/InsR added any prognostic information alone or combined among patients treated with radiotherapy (n = 604) or chemotherapy (n = 239).
Phospho-IGF1R/InsR adds prognostic information in non-endocrine-treated patients
There was a significant effect modification of any type of endocrine treatment on the prognostic value of pIGF1R/InsR among patients with ER+ tumors (Pinteraction = 0.022). Patients were therefore stratified according to endocrine treatment. As stated above, pIGF1R/InsR was not associated with event-free survival for endocrine-treated patients with ER+ tumors whether or not they had also received radiotherapy or chemotherapy (Figure 4A-4C). Non-endocrine-treated patients with ER+ and pIGF1R/InsRpos tumors had a borderline significant decreased risk of any event after adjustment for prognostic factors and tumor storage time, HRadj (0.39; 95% CI 0.15-1.04). Significant decreased risks for any event with pIGF1R/InsRpos expression were observed among non-endocrine-treated patients with ER- tumors, HRadj (0.27; 95% CI 0.09-0.77), as well as for all non-endocrine-treated patients irrespective of ER status, HRadj (0.32; 95% CI 0.16-0.63; Table 2; Figure 4D). The interaction between pIGF1R/InsR and endocrine treatment was present irrespective of ER status (Pinteraction = 0.024). Phospho-IGF1R/InsR was not a prognostic marker for distant metastasis-free survival or overall survival.
The prognostic value of pIGF1R/InsR expression was investigated in radiotherapy- (n = 169) and chemotherapy- (n = 80) non-endocrine-treated patients irrespective of ER status. Radiotherapy-treated patients with pIGF1R/InsRpos tumors had a lower risk for breast cancer events, HRadj (0.31; 95% CI 0.12-0.80; Figure 4E), but not for distant metastasis-free survival or overall survival. A similar association was also seen in chemotherapy-treated patients with pIGF1R/InsRpos tumors, HRadj (0.29; 95% CI 0.09-0.99; Figure 4F). Among the patients treated with chemotherapy, pIGF1R/InsRpos was additionally borderline associated with better prognosis for distant metastasis-free survival, HRadj (0.23; 95% CI 0.05-1.03), and overall survival, HRadj (0.30; 95% CI 0.08-1.08).
The pIGF1R/InsR antibody may cross-react with other activated tyrosine kinase receptors according to the manufacturer. There were only 7 out of 748 (0.9%) pIGF1R/InsRpos tumors with negative staining for both IGF1R and InsR, and additional 13 (1.7%) tumors with expression unknown for one or both of the markers. The effect estimates remained essentially the same after removing these cases in a restriction analysis (Table 2).
Table 2: Multivariable Cox regression models for pIGF1R/InsR among non-endocrine-treated patients irrespective of ER status.
Model 1 n=248 |
Model 2a n=248 |
Model 3b n=240 |
||||||||
Variables |
HR |
95% CI |
P-value |
HR |
95% CI |
P-value |
HR |
95% CI |
P-value |
|
pIGF1R/InsR |
positive |
0.32 |
0.17-0.62 |
0.001 |
0.32 |
0.16-0.63 |
0.001 |
0.34 |
0.17-0.67 |
0.002 |
Age |
continuous |
0.98 |
0.95-1.01 |
0.19 |
0.98 |
0.95-1.01 |
0.19 |
0.98 |
0.95-1.01 |
0.17 |
Invasive tumor size |
≥21 mm or skin or muscular involvement |
4.90 |
1.94-12.38 |
0.001 |
4.88 |
1.93-12.35 |
0.001 |
4.73 |
1.89-11.87 |
0.001 |
Axillary node involvement |
positive |
1.77 |
0.76-4.11 |
0.19 |
1.78 |
0.76-4.18 |
0.19 |
1.80 |
0.77-4.17 |
0.17 |
Histological grade |
III |
1.23 |
0.41-3.67 |
0.71 |
1.21 |
0.40-3.73 |
0.74 |
1.26 |
0.41-3.84 |
0.69 |
ER |
positive |
0.95 |
0.29-3.17 |
0.93 |
0.93 |
0.26-3.29 |
0.91 |
0.93 |
0.26-3.29 |
0.91 |
BMI |
≥25 kg/m2 |
1.10 |
0.56-2.14 |
0.79 |
1.10 |
0.56-2.14 |
0.79 |
1.14 |
0.58-2.22 |
0.71 |
All models are adjusted for treatment; chemotherapy and radiotherapy.
a Adjusted for tumor storage time (years).
b Restriction analysis: Excluding pIGF1R/InsRpos tumors without positive staining for both IGF1R and InsR, or unknown for one or both of the markers (n=20 for total and n=8 for non-endocrine-treated patients) and adjusted for tumor storage time (years).
23 patients had missing values for one or more adjustment variables.
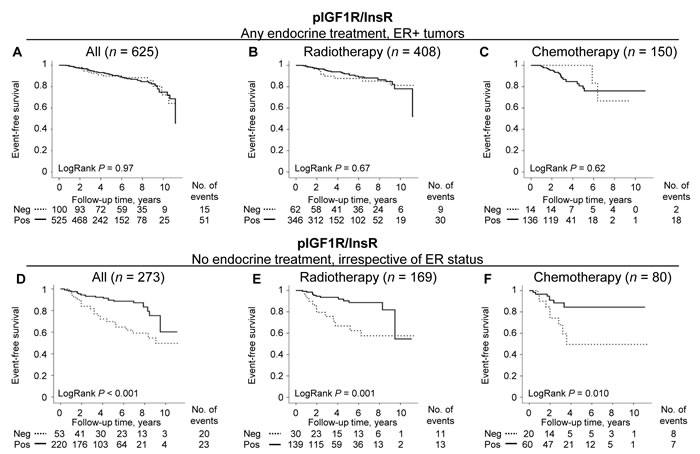
Figure 4: The prognostic importance of pIGF1R/InsR depending on endocrine treatment regarding event-free survival. Kaplan-Meier curves presenting A.-C. endocrine-treated patients with ER+ tumors and D.-F. non-endocrine-treated patients irrespective of ER status. (B, E) patients also receiving adjuvant radiotherapy, and (C, F) patients also treated with adjuvant chemotherapy. Dashed lines represent patients with pIGF1R/InsRneg tumors, and solid lines pIGF1R/InsRpos tumors.
Phospho-IGF1R/InsR adds opposing overall survival information depending on InsR status among non-endocrine-treated patients
The potential involvement of InsR on patient outcome in combination with pIGF1R/InsR was investigated in non-endocrine-treated patients. For patients with tumors with InsRmod/strong expression, pIGF1R/InsRpos was associated with significantly lower risk for events, HRadj (0.26; 95% CI 0.12-0.58), and distant metastasis, HRadj (0.22; 95% CI 0.06-0.85) compared with pIGF1R/InsR negativity. There was no significant interaction between InsR and pIGF1R/InsR when investigating any type of first event or distant metastasis-free survival. However, for overall survival the interaction between the markers indicated a significant effect modification of pIGF1R/InsR depending on InsR status (Pinteraction = 0.030). Phospho-IGF1R/InsR positivity was non-significantly associated with shorter overall survival in patients with InsRneg/weak tumors, but was borderline associated with longer overall survival in patients with InsRmod/strong expression, HRadj (0.32; 95% CI 0.10-1.01).
Sensitivity analyses
Since there were 15 patients with bilateral tumors, sensitivity analyses were performed. For each of the markers, five patients had no evaluable core on the bilateral side. For the patients with two evaluable tumors, few tumors changed dichotomized status; IGF1R (n = 1), InsR (n = 3), and pIGF1R/InsR (n = 4). The results remained essentially the same in the sensitivity analyses using the dichotomized status for the contralateral tumor in all but two analyses. For InsRmod/high in all patients, the results became significant HRadj 0.60 (95%CI 0.37-0.97), while for IGF1Rstrong the subgroup of AI-treated patients >50 years old with ER+ tumors, the results became non-significant when using the IGF1R status for the contralateral tumor.
Discussion
The IGF system has an established mitogenic role in cancer. However, recent clinical trials examining IGF1R targeting therapies have been disappointing and have highlighted the need for improved selection of patients likely to benefit from these treatment strategies. This study demonstrated that IGF1Rstrong expression was associated with poorer prognosis and impacted endocrine treatment response differently depending on patients’ age and type of endocrine therapy. Phospho-IGF1R/InsRpos expression was independently associated with longer event-free survival, but this association was only observed among non-endocrine treated patients irrespective of ER status. InsR conferred a significant effect modification on the associations between prognosis and combinations of IGF1R and pIGF1R/InsR, where pIGF1R/InsR, IGF1Rstrong/InsRmod/strong/pIGF1R/InsRpos tumors were associated with the worst prognosis.
The prognostic importance of tumor IGF1R levels has previously been studied with conflicting results, possibly related to different patient cohort compositions, antibodies, and cut-offs [16, 17, 20, 21]. In the present study, the prognostic relevant cut-offs were determined through exploratory analyses. Groups where the curves crossed over were combined into one group in order to avoid violation of the assumption of proportional hazards. A recent meta-analysis of ten independent studies evaluating cytoplasmic and membrane staining of IGF1R in breast cancer patients concluded that IGF1R was associated with better outcome in hormone receptor positive cancers, but with poor survival in triple-negative breast cancers [20]. This is in contrast to our finding of worse prognosis among patients with IGF1Rstrong expressing tumors; however IGF1R was not an independent prognostic marker. In the present study, there was a significant association between IGF1Rstrong expression and triple-negative tumors, larger invasive tumors and axillary lymph node involvement, which are all features of aggressive breast cancer. It may appear contradictory with a significant association between IGF1Rstrong expression and higher frequency of endocrine treatment, as well as a higher proportion of triple-negative tumors among IGF1Rstrong tumors compared to the IGF1Rnot strong tumors. However, the almost all of the patients with ER+ IGF1Rstrong tumors received endocrine treatment, which may reflect more aggressive tumor features, compared to a significantly lower proportion of endocrine-treated patients with ER+ IGF1Rnot strong tumors. Given the established mitogenic role of IGF1R from numerous preclinical studies, it is possible that tumors with IGF1Rstrong expression circumvent regulatory feedback loops and acquire more aggressive characteristics.
Despite a significant association between IGF1Rstrong expression and higher frequency of endocrine treatment, no association between IGF1Rstrong expression and ER positivity was detected in this patient cohort. IGF1Rstrong expression indicated poor prognosis among endocrine-treated patients with ER+ tumors, also after adjustment for chemotherapy and radiotherapy, although this finding should be interpreted with caution due to limited number of patients with tumors with IGF1Rstrong expression. Further, in one of the subgroups, the results did not remain significant in the sensitivity analyses when the contralateral tumor was used. These results are in line with a previous report showing that IGF1R overexpression is associated with endocrine resistance caused by increased downstream signaling [22], The treatment-predictive role of IGF1Rstrong expression differed depending on type of endocrine treatment and age of the patient. The shorter event-free survival among endocrine-treated patients with IGF1Rstrong expressing tumors may reflect general aggressive features related to those tumors. Endocrine-treated patients with IGF1Rstrong expressing tumors may therefore benefit from additional treatment, possibly an IGF1R-targeting therapy.
In contrast to the expected mitogenic role of IGF1R signaling, pIGF1R/InsR (Tyr1131/Tyr1146) positivity was independently associated with significantly longer event-free survival, consistent with some [18, 23], but not all previous research [19]. However, the association between longer event-free survival and pIGF1R/InsR positivity was only present in non-endocrine-treated patients irrespective of ER status. Although this is not a randomized controlled trial population and endocrine-treated and non-endocrine-treated patients differed in many aspects, we hypothesize that endocrine treatment may be more beneficial for patients with pIGF1R/InsRneg tumors. Exploratory analyses in the present cohort among patients with ER+ and pIGF1R/InsRneg tumors showed a lower risk for breast cancer events for endocrine-treated patients compared to non-endocrine treated patients. In contrast, no difference between endocrine-treated and non-endocrine-treated patients was observed among patients with ER+ and pIGF1R/InsRpos tumors (data not shown). In order to accurately test this hypothesis, the endocrine-treatment predictive value of pIGF1R/InsR should be tested in a randomized controlled trial, such as SBII:2, with patients randomized to TAM or no TAM treatment irrespective of ER status [24].
This study showed that non-endocrine-treated patients with pIGF1R/InsRpos tumors were less likely to have recurrence after radiotherapy and chemotherapy, compared with patients having pIGF1R/InsRneg tumors. The same was not seen in endocrine-treated patients. Tumors with higher proliferation rates are more sensitive to radiotherapy and chemotherapy. Since pIGF1R/InsR positivity indicates active IGF1R-signaling, which promotes cell proliferation, a plausible biological explanation would be that pIGF1R/InsRpos tumors with higher proliferative signals are more responsive to radio- and chemotherapy, than pIGF1R/InsRneg tumors. However, the Ki67 proliferative index was only available as of March 2009 and therefore not further investigated in this study. In support of our findings, it has been shown in experimental models that blocking IGF1R after chemotherapy resulted in better therapeutic response than IGF1R blockade followed by chemotherapy [25]. In contrast to the report by Turner et al., IGF1R was not a prognostic marker for radiotherapy response [13].
InsRmod/strong expression was associated with longer overall survival, and both InsRmod/strong and pIGF1R/InsRpos expression was associated with ER+, which confirm the engagement of the two signaling systems [2]. Previously, InsR positivity has been associated with worse outcome [19, 26]. However, earlier studies have focused on individual markers. In the present study, InsR status was important in combination with the other markers. Patients with tumors with both pIGF1R/InsRpos and IGF1Rstrong expression had a worse prognosis only when the tumor also expressed mod/strong levels of InsR, suggesting formation of IGF1R/InsR heterodimers. This is in line with a previous report demonstrating a direct association between InsR overexpression and increased abundance of hybrid IGF1R/InsR receptors, relative to IGF1R homodimers, in breast cancer specimens. Furthermore, hybrid receptors were more responsive to IGF-I stimulation with receptor phosphorylation exceeding that of IGF1R [27]. This illustrates the complexity of the IGF1R signaling network and the importance of evaluating several biomarkers in the pathway.
This population-based patient cohort is representative for the southern region of Sweden [28] with a high follow-up rate [29, 30]. Accordingly, the included patients were not randomized to treatment, often received more than one treatment, and may have switched between TAM and AIs. In addition, treatment regimens and guidelines changed over time, which made it challenging to evaluate any treatment specific effects. However, this study includes consecutive primary breast cancer patients and thereby reflects the authentic clinical situation. The missing 72 cases did not differ significantly from the included 946 patients regarding tumor and patient characteristics (data not shown). This indicates that there was no bias between included patients with evaluable tumors and excluded patients with non-evaluable tumors. Each marker was evaluated on a separate tissue section of the tumor core, which enables co-expression of the markers in the same tumor, but not in individual cells. Triple-staining immunohistochemistry could increase the accuracy of the co-staining but is technically challenging due to the risk of cross reactions between antibodies as well as difficulties in distinguishing between three colors. This study also provides support for the notion that staining of some, but not all markers change with storage time and adjustment for storage time may be warranted.
The selected pIGF1R/InsR antibody was chosen based on a previous publication evaluating the expression of pIGF1R/InsR in breast cancer tissue with IHC, and the specificity by treating DU145 prostate cancer cells with a IGF1R tyrosine kinase inhibitor [19]. Since the antibody may cross-react with other tyrosine kinase receptors, restriction analyses were performed in the present study. The results remained essentially the same after removing the few cases that were pIGF1R/InsRpos but negative for both IGF1R and InsR or had tumors where expression for either IGF1R and/or InsR was unknown (n = 20). The findings from this study suggest that this pIGF1R/InsR antibody may be a clinically relevant marker since the results obtained using this antibody indicated a strong independent association with prognosis among non-endocrine-treated breast cancer patients. There are two isoforms of the insulin receptor, InsR-A and InsR-B, where InsR-A is the predominant isoform in breast cancer [31]. The selected InsR antibody detects the β subunit, which is identical for the two isoforms and cannot distinguish between them. InsR expression in the present study thus reflects the total amount of InsR that may form heterodimers with IGF1R.
The disappointing results from clinical trials with IGF1R inhibitors may be due to an inadequate selection of patients and emphasize the importance of finding predictive biomarkers. These should also include InsR since it can form heterodimers with IGF1R. Although beyond the scope of this study, aberrant systemic or local IGF ligand levels may additionally predict patients with IGF-dependent tumors likely to respond to IGF-intervention strategies. Body constitution such as weight and BMI may influence IGF-I, insulin and C-peptide levels [32, 33]. In line with this, there are indications that BMI might be important to consider when identifying patients likely to benefit from IGF-targeted therapies [1]. Compared to North American cohorts, the present study population had a relatively low BMI that may influence the relationship between IGF1R signaling and breast cancer prognosis. Data regarding body measurements were available in the present patient cohort, and all multivariable models were adjusted for BMI. The only association observed between body constitution and tumor markers was between height and InsR expression.
Taken together, the data from this study supports the hypothesis that patients with IGF1Rstrong/InsRmod/strong/pIGF1R/InsRpos tumors had shorter event-free survival compared to all other groups. InsR significantly modified the impact of the combination of IGF1R and pIGF1R/InsR on prognosis, which may reflect the balance of IGF1R/InsR hetero- and homodimers and thereby receptor activity. IGF1Rstrong expression was a predictive indicator of age-related endocrine treatment response, and pIGF1R/InsR positivity indicated better response to radiotherapy and/or chemotherapy in non-endocrine-treated patients, irrespective of ER status. This study highlights the complexity of the IGF system including its interplay with endocrine treatment in relation to breast cancer outcome. The results suggest that evaluation of all three markers confer a more comprehensive understanding than individual markers and may lead to improved selection of patients for IGF-treatment regimens.
Material and Methods
Patients
The patient material for this study is part of an ongoing cohort, BC Blood Study, and described in detail by Simonsson et al. [29]. 1,116 patients diagnosed with primary breast cancer between October 2002 and June 2012 at the Skåne University Hospital, Lund, Sweden, were included. The patients were between 24 and 99 years old at inclusion without other history of cancer within the last ten years. The patients’ body measurements, including weight, height, waist and hip circumference, and breast volume [34, 35], were measured by a research nurse prior to surgery. Patients were additionally asked to fill out questionnaires regarding reproductive history, use of exogenous hormones or other medications, and lifestyle factors including smoking, alcohol and coffee consumption. Clinicopathological information regarding tumor size, lymph node status, histological grade, HER2 (HER2 was routinely analyzed in patients <70 years with invasive tumors as of November 2005; nmissing = 263), ER, and progesterone receptor (PR) status were obtained from medical records and pathology reports. Information about breast cancer recurrence or death was collected from patient charts, pathology reports, the Regional Tumor Registry or the Population Registry. Treatment was administered according to standard of care and was recorded until the first breast cancer event. In patients without breast cancer events, treatments were recorded until last follow-up or death prior to July 1, 2014. Written informed consents were obtained from all participating patients and the study was approved by the local ethics committee at Lund University (Dnr 75-02, Dnr 37-08, Dnr 658-09, Dnr 58-12, Dnr 379-12, Dnr 227-13, Dnr 277-15, and Dnr 458-15).
The final study cohort consisted of 946 patients after excluding patients who received preoperative treatment (n = 51), patients with only ductal carcinoma in situ (n = 39), patients with distant metastasis ≤0.3 years from baseline (n = 8), and tumors missing from the TMA or no evaluable cores for all three markers (n = 72; Figure 1A). Inability to assess staining was due to loss of tumor cores or cores not containing invasive tumor cells. The report followed the REMARK criteria [36].
Tissue microarray and immunohistochemistry
Dual cores (1.0 mm) from representative tumor regions of formalin-fixed paraffin-embedded (FFPE) tissue blocks were collected from surgical specimens and assembled in a tissue microarray (TMA), using a semi-automated tissue array device (Beeches instruments, Sun Prairie, WI). The FFPE blocks were stored in room temperature prior to sectioning and the 4 μm thick TMA sections were kept in -20°C until immunohistochemical staining. The sections were automatically deparaffinized followed by pretreatment using the PT Link system (DAKO, Glostrup, Denmark). Sections for all three markers were obtained from the same tumor core and sectioned at the same occasion. Immunohistochemistry was subsequently performed for each marker on individual slides using the Autostainer Plus from DAKO with the EnVision FLEX high-pH kit, according to the manufacturer’s instructions (DAKO, Glostrup, Denmark). The following antibodies were used: IGF1Rβ (sc-713, Santa Cruz Biotechnology; dilution 1:150), phospho-IGF1Rβ (Tyr1131)/Insulin Receptor β (Tyr1146) (#3021, Cell Signaling Technology; dilution 1:50), Insulin Receptor (β-subunit) (GR36, Calbiochem; dilution 1:50).
Evaluation of the immunohistochemical staining was performed by two independent observers (SBj, AR), without knowledge of tumor characteristics and patient information. In case of discrepancy for any of the three assessed markers and any parameter (5.6%), a re-examination was done until consensus was reached. Scoring included cytoplasmic staining intensity score; negative (neg), weak, moderate (mod), strong, and membrane staining; neg, weak, strong. Since both cytoplasmic and membranous receptors may be of importance, a combined score of cytoplasmic and membrane staining was applied for all three markers. For IGF1R: tumors showing neg, weak or moderate cytoplasmic and/or membrane negative or weak staining were considered IGF1Rnot strong, and the tumors with either strong cytoplasmic or strong membrane staining were classified as IGF1Rstrong. For InsR: tumors with no or weak cytoplasmic staining and no membrane staining were considered InsRneg/weak, while moderate and strong cytoplasmic staining and positive membrane staining was considered InsRmod/strong. For pIGF1R/InsR: tumors with no staining in the cytoplasm and membrane were considered pIGF1R/InsRneg, and those with weak, moderate or strong cytoplasmic and/or membrane staining were considered pIGF1R/InsRpos. In case of bilateral tumors (n = 15), the highest value was applied. All dichotomized values for cytoplasmic intensity and membrane staining came from the same tumor for each individual marker. Dichotomized scores for the three different markers came from the same tumor except in one case. This patient was therefore removed from all analyses with combined markers (n = 858). The tumor characteristics from the same tumor were used in all analyses where tumor characteristics were included. Sensitivity analyses were performed using the values for the bilateral tumor.
Statistical methods
The SPSS software versions 19 and 22 (IBM) was utilized for all statistical analyses. The following variables were used as continuous variables: age (years), BMI (kg/m2), waist-to-hip ratio, height (m), and weight (kg). The subsequent variables were used as dichotomous variables: breast volume (≥850 mL; yes/no), patients who had received postoperative chemotherapy (yes/no), radiotherapy (yes/no), and endocrine therapy (yes/no); the endocrine therapy group was stratified according to TAM treatment (yes/no) and AI treatment (yes/no) prior to any breast cancer event, last follow-up or death. Tumor characteristics included invasive pathologic tumor size (≤20 mm, ≥21-50 mm, ≥51 mm or skin or muscular involvement), axillary lymph node involvement (0, 1-3, 4+), histologic grade (I-III), hormone receptor status (ER+, PR+), HER2 amplification, and triple-negativity for ER, PR and HER2. Due to few patients with tumors ≥51 mm (n = 14) or skin or muscular involvement (n = 2) these groups were combined with patients with tumors ≥21 mm for all analyses.
Linear-by-linear association test was used for associations between expression levels and categorical variables. The Mann-Whitney U-test was used to compare medians for continuous variables due to non-normal distributions. The LogRank test was used for univariable survival analyses, and illustrated with Kaplan-Meier curves. Cox regression was used for multivariable analyses providing hazard ratios (HRs) with 95% confidence intervals (CI) adjusted for age (continuous), invasive tumor size (≥21 mm or skin or muscular involvement), any axillary lymph node involvement, histological grade III, ER status, and BMI (≥25 kg/m2). Staining intensity may vary depending on storage time for the tumors. Tumor storage time (years) between surgery and staining of IGF1R, InsR and pIGF1R/InsR was therefore investigated with the Mann-Whitney U-test. A significant association between longer tumor storage time and weaker staining intensity was found for InsR (P<0.001) and for pIGF1R/InsR (P<0.001), while staining intensity did not significantly differ with storage time for IGF1R (P = 0.28). Tumor storage time was therefore added to the adjustment variables for analyses of InsR and pIGF1R/InsR. Interaction terms between the combination of IGF1R and pIGF1R/InsR and InsR, and between pIGF1R/InsR and any endocrine treatment, and pIGF1R/InsR and InsR were calculated and used in Cox regression analyses to investigate potential effect modifications prior to stratification.
Patients were followed from inclusion to the first breast cancer event or distant metastasis, respectively, and patients without events were censored at the last follow-up or death prior to July 1st 2014. Breast cancer events were defined as local or regional recurrences, contralateral cancer or distant metastasis. For distant metastasis-free survival, only distant metastases were considered events. Death due to any cause was the only considered event for overall survival.
Power calculations assuming 900 patients with an accrual interval of 10 years and additional follow-up time of two years and a frequency of 5% or 16.7% of IGF1Rstrong, InsRmod/strong and pIGF1R/InsRpos tumors showed that the study was able to detect true HRs between 0.591 and 1.866 for 5%, and 0.731 and 1.412 for 16.7% with 80% power and α of 5% [37].
Two-tailed nominal P-values not adjusted for multiple testing are presented. A P-value of less than 0.05 was considered significant.
Abbreviations
insulin-like growth factor receptor 1 (IGF1R), insulin receptor (InsR), estrogen receptor (ER), progesterone receptor (PgR), human epidermal growth factor receptor (HER2), tamoxifen (TAM, aromatase inhibitor (AI), phosphatidylinositol 3-kinase (PI3K), mitogen activated protein kinase (MAPK)
Acknowledgments
The authors thank research nurses Anette Ahlin Gullers, Monika Meszaros, Maj-Britt Hedenblad, Karin Henriksson, Annette Möller, Helén Thell, Jessica Åkesson, and Linda Ågren. They also thank Björn Nodin and Elise Nilsson for TMA construction, Kristina Lövgren for staining, and Catarina Blennow for sectioning, as well as breast pathologist Anna Ehinger for help with histopathological assessments.
Conflicts of interest
No potential conflicts of interest were disclosed.
Funding
This work was supported by grants from The Swedish Cancer Society (CAN2014/465) (Helena Jernström); the Swedish Research Council (K2012-54X-22027-01-3) (Helena Jernström); the Mrs. Berta Kamprad Foundation (BKS19/2014, BKS27/2015) (Helena Jernström); the Gunnar Nilsson Foundation (Helena Jernström); the Swedish Breast Cancer Group (BRO) (Christian Ingvar); the South Swedish Health Care Region (Region Skåne ALF 10622) (Helena Jernström); Konung Gustaf V:s Jubileumsfond (Helena Jernström); the Lund Hospital Fund (Christian Ingvar), the RATHER consortium (http://www.ratherproject.com/), and the Seventh Framework program ([email protected]). The funding agencies played no role in design of the study; the collection, analysis, and interpretation of the data; the writing of the manuscript; or the decision to submit the manuscript for publication.
Author contributions
Conception and design: S. Björner, A. Rosendahl, C Rose, C. Ingvar, H. Jernström Development of methodology: S. Björner, A. Rosendahl, H. Jernström Acquisition of data: S. Björner, A. Rosendahl, M. Simonsson, A. Markkula, C. Ingvar, H. Jernström Analysis and interpretation of data: S. Björner, A. Rosendahl, H. Jernström Writing, review, and/or revision of the manuscript: S. Björner, A. Rosendahl, M. Simonsson, A. Markkula, K. Jirström, S. Borgquist, C. Rose, C. Ingvar, H. Jernström Administrative, technical, or material support: S Björner, A. Rosendahl, M. Simonsson, A. Markkula, K. Jirström, H. Jernström Study supervision: C. Ingvar, H. Jernström.
Editorial note
This paper has been accepted based in part on peer-review conducted by another journal and the authors’ response and revisions as well as expedited peer-review in Oncotarget.
References
1. Pollak M. The insulin and insulin-like growth factor receptor family in neoplasia: an update. Nat Rev Cancer. 2012; 12: 159-69. doi: 10.1038/nrc3215.
2. Yee D, Lee AV. Crosstalk between the insulin-like growth factors and estrogens in breast cancer. J Mammary Gland Biol Neoplasia. 2000; 5: 107-15.
3. Crudden C, Girnita A, Girnita L. Targeting the IGF-1R: The Tale of the Tortoise and the Hare. Front Endocrinol (Lausanne). 2015; 6: 64. doi: 10.3389/fendo.2015.00064.
4. Hawsawi Y, El-Gendy R, Twelves C, Speirs V, Beattie J. Insulin-like growth factor - oestradiol crosstalk and mammary gland tumourigenesis. Biochim Biophys Acta. 2013; 1836: 345-53. doi: 10.1016/j.bbcan.2013.10.005.
5. Eccles SA, Aboagye EO, Ali S, Anderson AS, Armes J, Berditchevski F, Blaydes JP, Brennan K, Brown NJ, Bryant HE, Bundred NJ, Burchell JM, Campbell AM, et al. Critical research gaps and translational priorities for the successful prevention and treatment of breast cancer. BCR. 2013; 15: R92. doi: 10.1186/bcr3493.
6. Yee D. Insulin-like growth factor receptor inhibitors: baby or the bathwater? J Natl Cancer Inst. 2012; 104: 975-81. doi: 10.1093/jnci/djs258.
7. Wang N, Rayes RF, Elahi SM, Lu Y, Hancock MA, Massie B, Rowe GE, Aomari H, Hossain S, Durocher Y, Pinard M, Tabaries S, Siegel PM, et al. The IGF-Trap: Novel Inhibitor of Carcinoma Growth and Metastasis. Mol Cancer Ther. 2015; 14: 982-93. doi: 10.1158/1535-7163.MCT-14-0751.
8. Sachdev D. Drug evaluation: CP-751871, a human antibody against type I insulin-like growth factor receptor for the potential treatment of cancer. Curr Opin Mol Ther. 2007; 9: 299-304.
9. Gao J, Chesebrough JW, Cartlidge SA, Ricketts SA, Incognito L, Veldman-Jones M, Blakey DC, Tabrizi M, Jallal B, Trail PA, Coats S, Bosslet K, Chang YS. Dual IGF-I/II-neutralizing antibody MEDI-573 potently inhibits IGF signaling and tumor growth. Cancer Res. 2011; 71: 1029-40. doi: 10.1158/0008-5472.CAN-10-2274.
10. Friedbichler K, Hofmann MH, Kroez M, Ostermann E, Lamche HR, Koessl C, Borges E, Pollak MN, Adolf G, Adam PJ. Pharmacodynamic and antineoplastic activity of BI 836845, a fully human IGF ligand-neutralizing antibody, and mechanistic rationale for combination with rapamycin. Mol Cancer Ther. 2014; 13: 399-409. doi: 10.1158/1535-7163.MCT-13-0598.
11. Iams WT, Lovly CM. Molecular Pathways: Clinical Applications and Future Direction of Insulin-like Growth Factor-1 Receptor Pathway Blockade. Clin Cancer Res. 2015; 21: 4270-7. doi: 10.1158/1078-0432.CCR-14-2518.
12. Lu Y, Zi X, Zhao Y, Mascarenhas D, Pollak M. Insulin-like growth factor-I receptor signaling and resistance to trastuzumab (Herceptin). J Natl Cancer Inst. 2001; 93: 1852-7.
13. Turner BC, Haffty BG, Narayanan L, Yuan J, Havre PA, Gumbs AA, Kaplan L, Burgaud JL, Carter D, Baserga R, Glazer PM. Insulin-like growth factor-I receptor overexpression mediates cellular radioresistance and local breast cancer recurrence after lumpectomy and radiation. Cancer Res. 1997; 57: 3079-83.
14. Fox EM, Miller TW, Balko JM, Kuba MG, Sanchez V, Smith RA, Liu S, Gonzalez-Angulo AM, Mills GB, Ye F, Shyr Y, Manning HC, Buck E, et al. A kinome-wide screen identifies the insulin/IGF-I receptor pathway as a mechanism of escape from hormone dependence in breast cancer. Cancer Res. 2011; 71: 6773-84. doi: 10.1158/0008-5472.CAN-11-1295.
15. Gooch JL, Van Den Berg CL, Yee D. Insulin-like growth factor (IGF)-I rescues breast cancer cells from chemotherapy-induced cell death—proliferative and anti-apoptotic effects. Breast Cancer Res Treat. 1999; 56: 1-10.
16. Aaltonen KE, Rosendahl AH, Olsson H, Malmström P, Hartman L, Fernö M. Association between insulin-like growth factor-1 receptor (IGF1R) negativity and poor prognosis in a cohort of women with primary breast cancer. BMC Cancer. 2014; 14: 794. doi: 10.1186/1471-2407-14-794.
17. Yerushalmi R, Gelmon KA, Leung S, Gao D, Cheang M, Pollak M, Turashvili G, Gilks BC, Kennecke H. Insulin-like growth factor receptor (IGF-1R) in breast cancer subtypes. Breast Cancer Res Treat. 2012; 132: 131-42. doi: 10.1007/s10549-011-1529-8.
18. Peiro G, Benlloch S, Sanchez-Tejada L, Adrover E, Lerma E, Peiro FM, Sanchez-Paya J, Aranda FI. Low activation of Insulin-like Growth Factor 1-Receptor (IGF1R) is associated with local recurrence in early breast carcinoma. Breast Cancer Res Treat. 2009; 117: 433-41. doi: 10.1007/s10549-008-0139-6.
19. Law JH, Habibi G, Hu K, Masoudi H, Wang MY, Stratford AL, Park E, Gee JM, Finlay P, Jones HE, Nicholson RI, Carboni J, Gottardis M, et al. Phosphorylated insulin-like growth factor-i/insulin receptor is present in all breast cancer subtypes and is related to poor survival. Cancer Res. 2008; 68: 10238-46. doi: 10.1158/0008-5472.CAN-08-2755.
20. Yan S, Jiao X, Li K, Li W, Zou H. The impact of IGF-1R expression on the outcomes of patients with breast cancer: a meta-analysis. Onco Targets Ther. 2015; 8: 279-87. doi: 10.2147/OTT.S74774.
21. Engels CC, de Glas NA, Sajet A, Bastiaannet E, Smit VT, Kuppen PJ, Seynaeve C, van de Velde CJ, Liefers GJ. The influence of insulin-like Growth Factor-1-Receptor expression and endocrine treatment on clinical outcome of postmenopausal hormone receptor positive breast cancer patients: A Dutch TEAM substudy analysis. Mol Oncol. 2016; 10: 509-16. doi: 10.1016/j.molonc.2015.10.010.
22. Zhang Y, Moerkens M, Ramaiahgari S, de Bont H, Price L, Meerman J, van de Water B. Elevated insulin-like growth factor 1 receptor signaling induces antiestrogen resistance through the MAPK/ERK and PI3K/Akt signaling routes. BCR. 2011; 13: R52. doi: 10.1186/bcr2883.
23. Gee JM, Robertson JF, Gutteridge E, Ellis IO, Pinder SE, Rubini M, Nicholson RI. Epidermal growth factor receptor/HER2/insulin-like growth factor receptor signalling and oestrogen receptor activity in clinical breast cancer. Endocr Relat Cancer. 2005; 12 Suppl 1: S99-S111. doi: 10.1677/erc.1.01005.
24. Stendahl M, Nilsson S, Wigerup C, Jirström K, Jönsson PE, Stål O, Landberg G. p27Kip1 is a predictive factor for tamoxifen treatment response but not a prognostic marker in premenopausal breast cancer patients. Int J Cancer. 2010; 127: 2851-8. doi: 10.1002/ijc.25297.
25. Zeng X, Sachdev D, Zhang H, Gaillard-Kelly M, Yee D. Sequencing of type I insulin-like growth factor receptor inhibition affects chemotherapy response in vitro and in vivo. Clin Cancer Res. 2009; 15: 2840-9. doi: 10.1158/1078-0432.CCR-08-1401.
26. Gradishar WJ, Yardley DA, Layman R, Sparano JA, Chuang E, Northfelt DW, Schwartz GN, Youssoufian H, Tang S, Novosiadly R, Forest A, Nguyen TS, Cosaert J, et al. Clinical and Translational Results of a Phase II, Randomized Trial of an Anti-IGF-1R (Cixutumumab) in Women with Breast Cancer That Progressed on Endocrine Therapy. Clin Cancer Res. 2016; 22: 301-9. doi: 10.1158/1078-0432.CCR-15-0588.
27. Pandini G, Vigneri R, Costantino A, Frasca F, Ippolito A, Fujita-Yamaguchi Y, Siddle K, Goldfine ID, Belfiore A. Insulin and insulin-like growth factor-I (IGF-I) receptor overexpression in breast cancers leads to insulin/IGF-I hybrid receptor overexpression: evidence for a second mechanism of IGF-I signaling. Clin Cancer Res. 1999; 5: 1935-44.
28. Persson M, Simonsson M, Markkula A, Rose C, Ingvar C, Jernström H. Impacts of smoking on endocrine treatment response in a prospective breast cancer cohort. Br J Cancer. 2016; 115: 382-90. doi: 10.1038/bjc.2016.174.
29. Simonsson M, Söderlind V, Henningson M, Hjertberg M, Rose C, Ingvar C, Jernström H. Coffee prevents early events in tamoxifen-treated breast cancer patients and modulates hormone receptor status. CCC. 2013; 24: 929-40. doi: 10.1007/s10552-013-0169-1.
30. Lundin KB, Henningson M, Hietala M, Ingvar C, Rose C, Jernström H. Androgen receptor genotypes predict response to endocrine treatment in breast cancer patients. Br J Cancer. 2011; 105: 1676-83. doi: 10.1038/bjc.2011.441.
31. Harrington SC, Weroha SJ, Reynolds C, Suman VJ, Lingle WL, Haluska P. Quantifying insulin receptor isoform expression in FFPE breast tumors. Growth Horm IGF Res. 2012; 22: 108-15. doi: 10.1016/j.ghir.2012.04.001.
32. Jernström H, Barrett-Connor E. Obesity, weight change, fasting insulin, proinsulin, C-peptide, and insulin-like growth factor-1 levels in women with and without breast cancer: the Rancho Bernardo Study. J Womens Health Gend Based Med. 1999; 8: 1265-72.
33. Jernström H, Olsson H. Insulin-like growth factor-1 in relation to adult weight and birth weight in healthy nulliparous women. Int J Gynaecol Obstet. 1998; 62: 11-8.
34. Markkula A, Bromee A, Henningson M, Hietala M, Ringberg A, Ingvar C, Rose C, Jernström H. Given breast cancer, does breast size matter? Data from a prospective breast cancer cohort. CCC. 2012; 23: 1307-16. doi: 10.1007/s10552-012-0008-9.
35. Ringberg A, Bågeman E, Rose C, Ingvar C, Jernström H. Of cup and bra size: reply to a prospective study of breast size and premenopausal breast cancer incidence. Int J Cancer. 2006; 119: 2242-3; author reply 4. doi: 10.1002/ijc.22104.
36. McShane LM, Altman DG, Sauerbrei W, Taube SE, Gion M, Clark GM, Statistics Subcommittee of the NCIEWGoCD. REporting recommendations for tumor MARKer prognostic studies (REMARK). Nat Clin Pract Urol. 2005; 2: 416-22.
37. Dupont WD, Plummer WD, Jr. Power and sample size calculations for studies involving linear regression. Control Clin Trials. 1998; 19: 589-601.

