INTRODUCTION
Approximately 400,000 new bladder cancer cases are diagnosed each year worldwide, with the highest rates in Europe, United States and Egypt [1]. While non- muscle invasive bladder cancer (NMIBC) recurs in up to 70% of cases after local treatment, they generally do not cause mortality [2]. However, once progression occurs (i.e. invasion into smooth muscle layers), rates of cancer-specific survival decrease to approximately 65% even in organ-confined disease [3, 4]. For this reason, most recent large-scale clinical trials define progression as increase in tumor staging from NMIBC to ≥T2 muscle-invasive bladder cancer (MIBC) [5–7]. Despite extensive research efforts to define genetic alterations and molecular signatures that associated with progression [8–11], the underlying mechanisms of bladder cancer progression remain elusive.
Several alterations within urothelial carcinoma cells were reported to associate with NMIBC progression. For instance, FGFR3 activating mutation associates with and is predictive of better prognosis [12–14], and abnormal expression of cytokeratin 20 positively associates with progression [15, 16]. Methylation of TBX2 and TBX3 genes are recently demonstrated to be predictive of progression [17]. Nevertheless, the tumor microenvironment, specifically alterations in the subepithelial stroma, during invasive progression of NMIBC remains largely unexplored.
It is well appreciated that epithelial cell functions, including cellular differentiation, migration and invasion, are directed by physical interactions with the extracellular matrix (ECM) [18]. Type I collagen is a major structural component of the ECM within bladder, and epithelial tumorigenesis is often accompanied by ECM alterations and remodeling [19]. In the current study, we set out to investigate a possible association of ECM alteration, particularly type I collagen mRNA and protein expression, with NMIBC progression to muscle-invasive disease.
RESULTS
High COL1A1 and COL1A2 mRNA expression correlates with poor overall and progression-free survival
First, we analyzed gene expression of a multi-institutional cohort comprising 189 Ta NMIBC patients, mRNA expression of genes encoding collagen I were evaluated in correlative with patient progression and survival using Cox regression and Kaplan-Meier analyses. Increased Type I collagen mRNA expression (COL1A1 and COL1A2 genes) was associated with NMIBC progression in this multi-institutional cohort (Figure 1A; patient information summarized in Table 1). Cox regression analyses demonstrated that higher COL1A1 and COL1A2 mRNA expression in patients were significantly associated with worse progression-free survival (Figure 1A) and overall survival (Figure 1B). Ten out of the fourteen COL1A1 probes and four out of the six COL1A2 probes demonstrated statistical significance for progression-free survival (p < 0.05 and p < 0.01, respectively - Supplementary Table S1). For overall survival, 9 out of the 14 COL1A1 probes and 4 out of the 6 COL1A2 probes demonstrated statistical significance (p < 0.01 and p < 0.001, respectively - Supplementary Table S1). Representative Kaplan-Meier analyses of the progression-free and overall survival corresponding to low or high mRNA expression of COL1A1 and COL1A2 are illustrated in Figure 1A and Figure 1B, respectively.
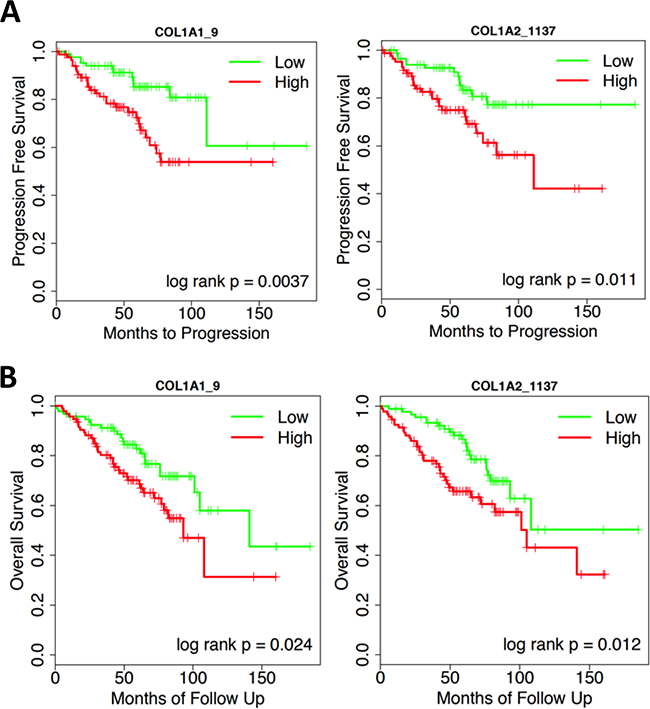
Figure 1: Representative Kaplan-Meier analyses of the A. progression-free and, B. overall survival corresponding to low (green) or high (red) mRNA expression of COL1A1 and COL1A2.
Table 1: Stage Tis, Ta mRNA Cohort – 189 Patients
Characteristic |
N (%) |
|---|---|
Median Age (IQR) |
67 (58-74) |
Male |
154 (81) |
High Grade* |
64 (34) |
CIS+ |
17 (9) |
EORTC High-Risk Group |
67 (35) |
Median Follow-up in Years (IQR) |
4.8 (3.4-6.7) |
Progression to T2 |
21 (11) |
Deaths |
57 (30) |
*2004 World Health Organization grade definitions
**European Organisation for Research and Treatment of Cancer
High collagen I protein expression near the tumor-ECM boundary significantly correlates with poor progression-free survival
To evaluate type I collagen expression at the protein level, we performed immunohistochemical (IHC) analysis using a NMIBC patient cohort treated at a single institute (patient information summarized in Table 2). Immunohistochemical analysis revealed very specific brown 3,3’-Diaminobenzidine (DAB) staining of collagen I, evidently accompanied by negatively stained areas that were counterstained by Hematoxylin (blue; Figure 2A-2D). Four different staining patterns of type I collagen protein were observed (Figure 2A-2D). For staining pattern 1, collagen I was expressed within the thin lining of stromal regions within epithelial papillary lesions (Figure 2A); for staining pattern 2, collagen I was expressed within the vasculature of stroma (Figure 2B); for staining pattern 3, reticular expression of collagen I was observed surrounding epithelial tumor cells (Figure 2C); and, for staining pattern 4, dense collagen I was expressed within subepithelial lamina propria near the tumor-ECM boundary (Figure 2D). Particularly, increased collagen I protein expression near the tumor-ECM boundary (staining pattern 4), was significantly associated with progression of NMIBC in this single institution cohort (Figure 2E; p = 0.0145). Representative patient samples with comparison to serial sections of H&E staining are also demonstrated in Figure 2A-2D. Nevertheless, collagen I staining within papillary tumor stroma, vascular tumor stroma, or surrounding reticular stroma (staining pattern types 1-3, respectively) were not significantly associated with NMIBC progression.
Table 2: Stage Tis, Ta Risk-Matched Tumor Bank Cohort – 80 Patients
Characteristic |
Progression (n = 16) N (%) |
No Progression (n = 64) N (%) |
P-Value |
|---|---|---|---|
Median Age (IQR) |
74 (60-78) |
69 (62-78) |
0.66 |
Male |
16 (100) |
63 (98) |
1.00 |
High Grade* |
9 (56) |
37 (58) |
0.91 |
CIS+ |
9 (56) |
27 (42) |
0.31 |
Multifocal |
10 (63) |
19 (30) |
0.01 |
> 3 cm |
3 (19) |
10 (16) |
0.76 |
EORTC High-Risk Group** |
9 (56) |
37 (58) |
0.91 |
Prior Local Treatment |
1 (6) |
5 (8) |
1.00 |
Median Follow-up in Years (IQR) |
6.6 (4.6-10.7) |
5.5 (3.5-8.4) |
0.32 |
*2004 World Health Organization grade definitions
**European Organisation for Research and Treatment of Cancer
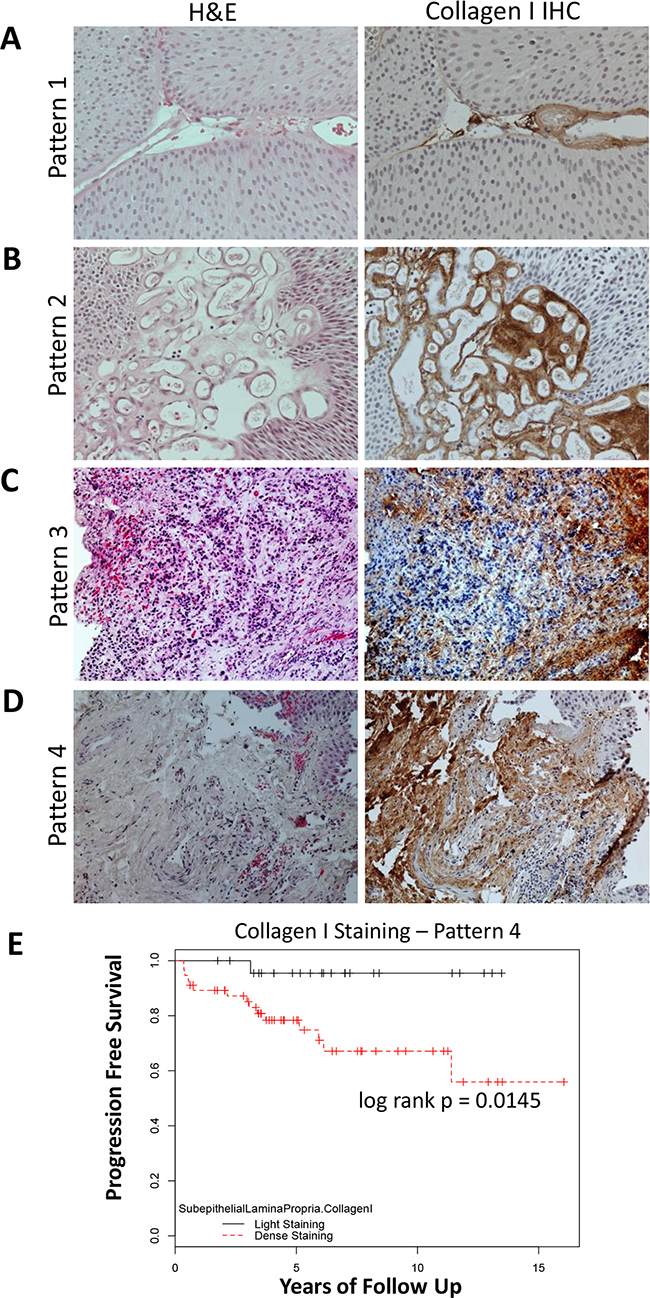
Figure 2: Specimen were scored based upon observed patterns of collagen I staining. Representative images for each of the staining pattern were listed as: A. pattern type 1 – staining of thin papillary tumor stroma, B. pattern type 2 – staining of vascular tumor stroma, C. pattern type 3 – reticular staining pattern of collagen surrounding epithelial tumor cells, and D. pattern type 4 – dense staining of subepithelial lamina propria near the tumor-ECM boundary. Serial sections with Hematoxylin & Eosin (H&E) staining was demonstrated in the left column. E. Kaplan-Meier plot of Collagen I IHC protein expression in the LP and its association with progression-free survival, (P = 0.0145).
Second harmonic generation (SHG) imaging revealed a significant association of low collagen fiber curvature ratio to progression
Due to the physical properties of type I collagen, when excited with a 400 nm wavelength photon, type I collagen emits a photon at exactly twice the wavelength (800 nm) [20]. This unique endogenous property of collagen can be visualized using state-of-the-art two-photon confocal microscopy, with a technique called SHG imaging [20]. Therefore, this imaging modality can reveal the structure of non-denatured collagen type I in tumor tissues without the aid of staining or fluorescent probes. The structure of subepithelial type I collagen was further examined using SHG imaging, using serial sections from the prior specimens concurrently analyzed by IHC (Figure 3; H&E and ColI IHC; representative images from patient 1-3). We have quantified collagen I structure in these SHG images (Figure 3; green fluorescent pseudo color), using a previously reported methodology to measure the curvature ratio (CR) of individual collagen fibers [21]. The CR was calculated using a previously reported method, where the traced length of the fibril (A) is divided by the linear distance between the two ends (B) [21, 22]. The median fibril CR (A divided by B) was compared between each image (Figure 3). Significantly lower collagen fiber CR near the tumor-stromal interface was observed in NMIBC specimen that progress into MIBC, when compared to those that did not progress into MIBC (Figure 4A; p = 0.0018). However, there was no significant difference in the maximum SHG signal between these two patient subgroups (Figure 4B).
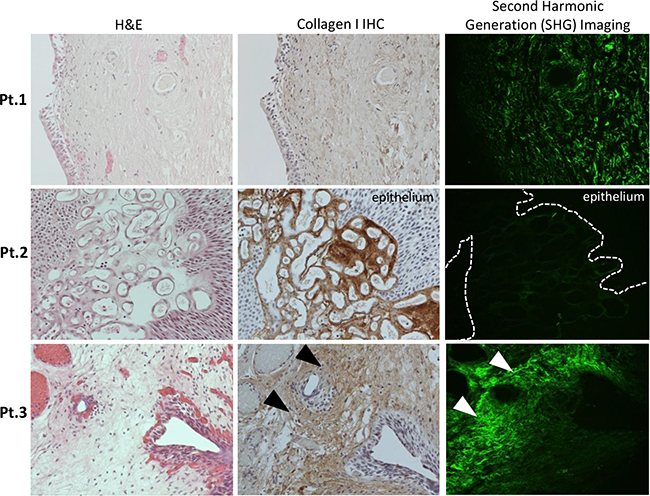
Figure 3: Representative images from individual NMIBC patients demonstrating Hematoxylin & Eosin (H&E) analysis, Collagen I protein expression by immunohistochemical analysis (IHC) and Second Harmonic Generation (SHG) imaging (20x serial sections from left to right). Patient 1 (Pt.1) – Carcinoma-in-situ (CIS) with normal lamina propria (LP), collagen I staining by IHC and SHG imaging of curved collagen fibers, no progression. Patient 2 (Pt.2) – Papillary tumor with increased collagen I IHC staining within vascular stroma, also visualized on SHG, no progression. Patient 3 (Pt.3)– increased sub-epithelial LP staining and fibers with low curvature ratio by SHG imaging, experienced progression to MIBC. Corresponding areas of dense, straight-fibered collagen I deposition in the subepithelial stroma were marked with arrows.
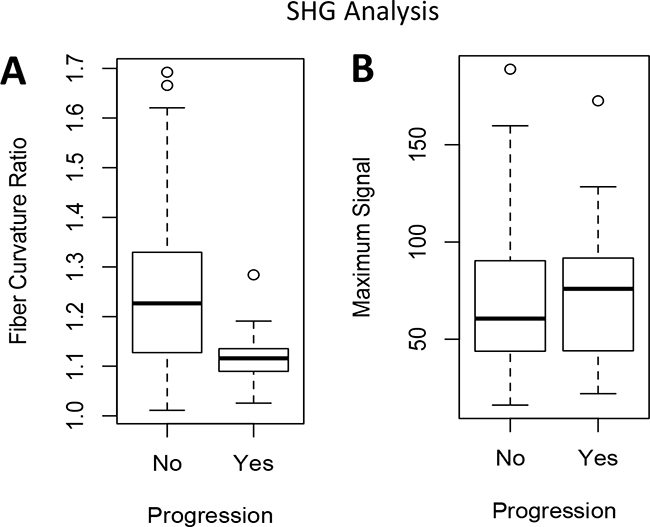
Figure 4: SHG imaging quantification comparing patients with progression to muscle-invasive disease versus those with no progression. Wilcoxon rank sum was used to compare measurements between patients with and without progression. (A) Median fiber curvature ratio P = 0.0018 (B) Maximum SHG signal P = 0.652.
DISCUSSION
Recently, it has been reported that type I collagen remodeling in the ECM microenvironment accompanies stromal invasion and epithelial tumorigenesis in other cancer types [22]. For the first time, we have investigated the collagen microenvironment in the context of NMIBC progression, and demonstrated a positive association of high COL1A1 and COL1A2 mRNA expression to progression and decreased overall survival in non-muscle invasive (Ta and Tis) disease (Figure 1) in a multi-center cohort. Within this multi-center NMIBC cohort, 35% of patients were considered high-risk based upon The European Organization for Research and Treatment of Cancer (EORTC) classification (Table 1), and risk group was significantly associated with progression and overall survival, as expected. Therefore, we decided to investigate the association of altered type I collagen protein expression with NMIBC progression in another risk-matched cohort of NMIBC. FFPE tissue blocks from the Michael E. DeBakey VAMC tissue bank, from 1992-2012, were obtained for this purpose. The control group was well-matched to the progression group, as the comparison between the risk factors revealed no major differences (Table 2), while multifocal disease was the only factor statistically increased in the progression group (Table 2). The VAMC treatment setting was advantageous for this investigation for several reasons. First, with the exception of six patients who underwent resection at an outside facility prior to their initial presentation to the VAMC, all tissues were obtained from the initial diagnosis and local surgical resection. Therefore, stromal changes associated with prior local surgical or intravesical treatment-induced wound healing would not be a confounding factor in this cohort. Second, the majority of patients in the cohort were followed long-term at the VAMC, allowing for detailed clinical follow-up.
Using these high-quality banked FFPE samples, type I collagen IHC was performed on serially sectioned slides, using IHC and a novel imaging analysis. Two blinded observers applied previously determined scoring criteria (Figure 2A-2D). To our knowledge at the time of this study, no other study has described patterns of bladder tumor type I collagen staining. Therefore, the criteria for papillary tumor stromal staining, vascular tumor stromal staining, reticular tumor stromal staining, and dense lamina propria staining near the tumor-ECM boundary (staining patterns 1-4, respectively, Figure 2A-2D), were based on our objective observation. In our analysis, dense type I collagen staining in the subepithelial lamina propria near the tumor-ECM boundary, was significantly associated with progression (Figure 2E). Similar collagen I staining patterns was observed in colon cancer at the invasive fronts [23]. In the context of bladder cancer, our IHC findings were logical for a few reasons. First, papillary tumors with fine stromal projections were documented to be less prone to progression when compared to broad-based or sessile tumors [24]. Secondly, the lamina propria is the immediate adjacent site at the invasive fronts for cancer cells; therefore, it is possible that type I collagen deposition within the lamina propria precedes muscle invasion.
We further investigated type I collagen structure in the context of these IHC staining pattern using SHG imaging. By comparing NMIBC tissues stained by collagen type I IHC to serially sectioned tumor tissues analyzed by SHG imaging (Figure 3; second and third column, respectively), we demonstrated the feasibility in using SHG imaging to capture collagen expressing areas within the bladder cancer specimens (Figure 3; third column). Additionally, SHG imaging provided unique quantitative data on the collagen type I fibril structure, where low CR (straighter fibers) were associated with tumor progression. Straighter fibers, with low CR, have been reported to represent a stronger tensile strength due to collagen fiber cross-linking and are associated with epithelial cancer cell invasion [22]. In prior research using breast cancer specimen derived from mouse models, these dense aligned type I collagen fibers at the tumor-ECM boundary led to increased rates of cancer progression [25–27]. Additional clinical research in breast cancer has demonstrated this type of pattern may provide valuable prognostic information in predicting clinical outcomes [28]. Consistent with this finding, we found a similar association in NMIBC, where patients with specimen demonstrating low CR experienced stage progression during follow-up.
Since type I collagen is one of the most abundant ECM components, these findings implicate a role for the stromal microenvironment in modulating invasive progression of NMIBC. Such implication is further supported by other study demonstrating additional collagen types, e.g. Col4a1 and Col18a1, are within a 12-gene signature predictive of progression [29]. Additionally, recent reports demonstrated a reciprocal interaction between urothelial carcinoma cells and the stromal compartment, through paracrine signaling pathways sonic-hedgehog and Wnt/BMP, which modulates epithelial differentiation and progression of bladder cancer [30, 31]. Indeed, not only have similar signaling pathways been described in other epithelial cancer types, but they can be modulated via epithelial transmembrane collagen receptors interacting with type I collagen in the ECM, resulting in epithelial mesenchymal transition (EMT) and progression of disease [23, 32, 33].
With respect to cellular differentiation, type I collagen can inhibit tumor differentiation in colon cancer models, resulting in stem-cell like gene expression at the invasive front [32, 34]. Although these mechanisms have yet to be explored in bladder cancer, stem-cell like features are typically associated with more aggressive bladder cancer phenotypes, resulting in poor clinical outcomes [35, 36]. A very recent study performing high-throughput analysis of NMIBC revealed a Class 2 tumor that associates with progression, these Class 2 tumors enriched for cancer stem cell markers such as ALDH1A1, ALDH1A2, PROM1, NES and THY1. [37] Additionally, our group recently demonstrated that deposition of collagen-rich ECM, as part of the wound repair process, is exploited by bladder cancer cells contributing to progressive development of chemoresistance in invasive bladder cancer through a stem-cell like phenotype [38]. Therefore, further characterization of type I collagen in the ECM of bladder tumors, and the signaling pathways utilized for stromal-epithelial interaction, will provide insights into both progression of bladder cancer, and potential resistance to treatment.
Notwithstanding, we recognize that the current study could be limited by a retrospective design and cohort size. We used rigorous statistical methods, however due to our limited cohort size, we relied on univariate analysis to assess the association of type I collagen with NMIBC progression and overall survival. Although we attempted to correct for confounders in our risk-matched cohort, it would be of importance to investigate these findings in the future using a larger, prospective cohort via multivariate analysis.
Together, we demonstrated for the first time, alterations in type I collagen mRNA expression, protein expression, and collagen structure were associated with progression of NMIBC to muscle-invasion. Our findings implicate the importance of stroma and wound response during bladder tumorigenesis, and will likely open a new avenue to further study collagen signaling through integrins or other downstream collagen receptors/effectors during bladder tumorigenesis. Additionally, further evaluation of the tumor microenvironment and tumor stroma may reveal additional biomarkers for progression that could be used to aid existing nomograms for NMIBC risk prediction [39, 40].
MATERIALS AND METHODS
Patients
A multi-center NMIBC cohort comprising 189 Ta NMIBC patients was utilized to investigate the association between collagen type I mRNA expression levels (COL1A1 and COL1A2) and clinical outcome. The patient characteristics for this cohort are described in Table 1. These patients were part of a multi-institutional effort to validate an mRNA assay predicting clinical outcomes [41]. Tumor progression was defined as increase in stage to T2 (muscle-invasive disease) or higher on subsequent biopsy or development of clinically proven metastasis. Since pathological tumor progression was our primary study endpoint, patients with initial stage T1 disease (lamina propria invasion) or higher were excluded due to the approximate 15-30% incidence of initial under staging of T1 disease [42–44].
A second single-institution NMIBC cohort was developed to investigate type I collagen protein expression and structure. From 1992 to 2012, 389 patients with bladder cancer who underwent local surgical treatment for bladder cancer during their initial presentation at the Michael E. DeBakey Veterans Affairs Medical Center (VAMC) in Houston were prospectively entered into an institutional cancer registry. Tumor stage and grade, as well as patient demographic information were entered into this registry. During this time period, sixteen patients who initially presented with Ta or Tis disease, experienced progression into muscle invasive disease during follow up. For each patient whom experienced progression, four other patients whom also presented with Ta or Tis disease during the same time period were included in this cohort. These patients had similar follow-up periods and known disease risk factors for progression including grade, presence of carcinoma in situ, tumors larger than 3 cm, and multifocal disease [2]. The patient characteristics for this cohort are described in Table 2.
Specimen characteristics
For the single-institution cohort, tissues from their initial and subsequent surgical treatments were stored as formalin-fixed paraffin-embedded (FFPE) samples in a central tumor bank. After reviewing patient demographic information and clinical follow-up to ensure fidelity, FFPE tissues from the initial surgical resection (trans-urethral resection of the tumor) were obtained from a central tissue repository. All initial pathology reports were reviewed, and specimen were re-evaluated using haematoxylin and eosin (H&E) slides by a pathologist (M.I.) to confirm the accuracy of initial disease staging. The tissue repository and patient information were protected and stored in accordance with the good research practices and under approval of the institutional review board protocol number H-26809.
Assay methods
mRNA expression from the multi-institutional cohort was analyzed using a custom cDNA microarray [41], with 14 and 6 specific probes used to hybridize COL1A1 and COL1A2 respectively (Figure 1).
For the single-institution cohort at the Michael E. DeBakey Veterans Affairs Medical Center (VAMC), immunohistochemistical (IHC) analysis was performed using a rabbit polyclonal antibody against Collagen I (Abcam, ab34710, 1:200). DAKO HRP-linked anti-rabbit secondary antibody was used to visualize the primary antibody. Collagen I IHC staining of tumor papillary stroma and subepithelial lamina propria compartments were compared, by two blinded observers. Specimen were scored based upon observed patterns of collagen I staining as follows: pattern type 1– staining of thin papillary tumor stroma, pattern type 2 – staining of vascular tumor stroma, pattern type 3 – reticular staining pattern of collagen surrounding epithelial tumor cells, and pattern type 4 – dense staining of subepithelial lamina propria near the tumor-ECM boundary (Figure 2A-2D). Both primary and secondary staining patterns were recorded for each specimen. Any discrepancies between observers were discussed until a final consensus score was agreed upon.
For second harmonic generation (SHG) imaging analysis, serial sections from the paraffin-embedded specimen were imaged using a state-of the art Carl Zeiss LSM 7 multiphoton microscope, and Chameleon Laser. The excitation wavelength was set to 400 nm, and imaging wavelength at 800 nm. Each specimen was imaged in at least two representative areas of stroma using a 20x objective. Images were analyzed using ImageJ version 1.48 (Wayne Rasband, NIH). Uniform 100x100 pixel regions of interest were repeatedly measured until the maximum signal was found for each image. The curvature ratio (CR) of individual collagen fibrils was measured for at least 10 representative fibrils in each image. The CR was calculated using a previously reported method, where the traced length of the fibril (A) is divided by the linear distance between the two ends (B) [21, 22]. The median fibril CR (A divided by B) was compared between each image (Figure 3).
Study design
Follow-up data and patient characteristics for the multi-institutional cohort were collected in a retrospective fashion [41]. Therefore, the association of COL1A1 and COL1A2 mRNA expression with tumor progression and overall survival was examined using subgroup analysis of a retrospective cohort study.
For the single-institution cohort, although specimens and patient characteristics were prospectively entered into a tumor registry, follow-up information was obtained in a retrospective fashion. Thus, the investigation of collagen type I protein expression and structure was performed as a separate retrospective cohort study. As stated previously, tumor grade and staging, patient characteristics, and follow-up were matched between sixteen patients whom experienced progression and sixty-four patients who did not.
The primary endpoint for analysis was progression to muscle-invasive disease (stage T2 or higher), which was determined by subsequent tumor biopsy in the majority of cases, or in a few, development of metastasis. The secondary endpoint for analysis was overall survival. The median follow-up for the multi-institutional cohort was 4.1 years. Within the single-institution cohort, a median follow up of 6.6 years and 5.5 years, were observed for patients whom experienced progression and those who did not, respectively.
Statistical analysis methods
All statistics were performed using R version 3.1.3 (https://cran.r-project.org/). Cox proportional hazard regression analysis was first used to examine if gene expression was significantly associated with progression-free and overall survival, respectively (Figure 1). For each gene in the Cox regression analysis, if the association was significant, the tumors were classified into low or high gene expression group using the median gene value as the cutoff. Survival curves were generated for the low or high gene expression tumors using the Kaplan-Meier method and log-rank test was used to evaluate if the survival curves were statistically different.
Patient characteristics and risk factors were compared using Fisher’s exact test, Pearson’s chi-squared test and Wilcoxon rank sum, when appropriate. Progression-free survival was compared between specimens with differing type I collagen IHC staining patterns also using log-rank test and Kaplan-Meier method. Analysis of SHG maximum signal and fiber CR were performed using Wilcoxon rank sum test. All tests were performed with two-sided tests and statistical significance was defined as p < 0.05, unless otherwise specified.
ACKNOWLEDGMENTS
We would like to thank the following grant funding support from the National Cancer Institute CA175397 (K.S.C.), Cancer Prevention and Research Institute of Texas (CPRIT RP140252) (K.S.C.), and the V Scholar Award (K.S.C.), CPRIT pre-doctoral fellowship RP101499 (A.V.K.), and AUA Research Scholar Award (P.L.H.). This work is also supported by the Human Tissue Acquisition & Pathology Core (NCI CA125123; M. Ittmann) at Baylor College of Medicine.
CONFLICTS OF INTEREST
The authors declare no conflict of interest.
REFERENCES
1. Chavan S, Bray F, Lortet-Tieulent J, Goodman M and Jemal A. International variations in bladder cancer incidence and mortality. European urology. 2014; 66:59-73.
2. Sylvester RJ, van der Meijden AP, Oosterlinck W, Witjes JA, Bouffioux C, Denis L, Newling DW and Kurth K. Predicting recurrence and progression in individual patients with stage Ta T1 bladder cancer using EORTC risk tables: a combined analysis of 2596 patients from seven EORTC trials. European urology. 2006; 49:466-465; discussion 475-467.
3. Shariat SF, Karakiewicz PI, Palapattu GS, Lotan Y, Rogers CG, Amiel GE, Vazina A, Gupta A, Bastian PJ, Sagalowsky AI, Schoenberg MP and Lerner SP. Outcomes of radical cystectomy for transitional cell carcinoma of the bladder: a contemporary series from the Bladder Cancer Research Consortium. The Journal of urology. 2006; 176:2414-2422; discussion 2422.
4. Tilki D, Reich O, Karakiewicz PI, Novara G, Kassouf W, Ergun S, Fradet Y, Ficarra V, Sonpavde G, Stief CG, Skinner E, Svatek RS, Lotan Y, Sagalowsky AI and Shariat SF. Validation of the AJCC TNM substaging of pT2 bladder cancer: deep muscle invasion is associated with significantly worse outcome. European urology. 2010; 58:112-117.
5. Burger M, Oosterlinck W, Konety B, Chang S, Gudjonsson S, Pruthi R, Soloway M, Solsona E, Sved P, Babjuk M, Brausi MA, Cheng C, Comperat E, et al. ICUD-EAU International Consultation on Bladder Cancer 2012: Non-muscle-invasive urothelial carcinoma of the bladder. European urology. 2013; 63:36-44.
6. Lamm D, Persad R, Brausi M, Buckley R, Witjes JA, Palou J, Bohle A, Kamat AM, Colombel M and Soloway M. Defining progression in nonmuscle invasive bladder cancer: it is time for a new, standard definition. The Journal of urology. 2014; 191:20-27.
7. van Rhijn BW, Burger M, Lotan Y, Solsona E, Stief CG, Sylvester RJ, Witjes JA and Zlotta AR. Recurrence and progression of disease in non-muscle-invasive bladder cancer: from epidemiology to treatment strategy. European urology. 2009; 56:430-442.
8. Cancer Genome Atlas Research N. Comprehensive molecular characterization of urothelial bladder carcinoma. Nature. 2014; 507:315-322.
9. Choi W, Porten S, Kim S, Willis D, Plimack ER, Hoffman-Censits J, Roth B, Cheng T, Tran M, Lee IL, Melquist J, Bondaruk J, Majewski T, et al. Identification of distinct basal and luminal subtypes of muscle-invasive bladder cancer with different sensitivities to frontline chemotherapy. Cancer cell. 2014; 25:152-165.
10. Sjodahl G, Lauss M, Lovgren K, Chebil G, Gudjonsson S, Veerla S, Patschan O, Aine M, Ferno M, Ringner M, Mansson W, Liedberg F, Lindgren D and Hoglund M. A molecular taxonomy for urothelial carcinoma. Clinical cancer research. 2012; 18:3377-3386.
11. Volkmer JP, Sahoo D, Chin RK, Ho PL, Tang C, Kurtova AV, Willingham SB, Pazhanisamy SK, Contreras-Trujillo H, Storm TA, Lotan Y, Beck AH, Chung BI, et al. Three differentiation states risk-stratify bladder cancer into distinct subtypes. Proceedings of the National Academy of Sciences of the United States of America. 2012; 109:2078-2083.
12. van Oers JM, Wild PJ, Burger M, Denzinger S, Stoehr R, Rosskopf E, Hofstaedter F, Steyerberg EW, Klinkhammer-Schalke M, Zwarthoff EC, van der Kwast TH and Hartmann A. FGFR3 mutations and a normal CK20 staining pattern define low-grade noninvasive urothelial bladder tumours. European urology. 2007; 52:760-768.
13. van Rhijn BW, Lurkin I, Radvanyi F, Kirkels WJ, van der Kwast TH and Zwarthoff EC. The fibroblast growth factor receptor 3 (FGFR3) mutation is a strong indicator of superficial bladder cancer with low recurrence rate. Cancer research. 2001; 61:1265-1268.
14. van Rhijn BW, Zuiverloon TC, Vis AN, Radvanyi F, van Leenders GJ, Ooms BC, Kirkels WJ, Lockwood GA, Boeve ER, Jobsis AC, Zwarthoff EC and van der Kwast TH. Molecular grade (FGFR3/MIB-1) and EORTC risk scores are predictive in primary non-muscle-invasive bladder cancer. European urology. 2010; 58:433-441.
15. Bertz S, Otto W, Denzinger S, Wieland WF, Burger M, Stohr R, Link S, Hofstadter F and Hartmann A. Combination of CK20 and Ki-67 immunostaining analysis predicts recurrence, progression, and cancer-specific survival in pT1 urothelial bladder cancer. European urology. 2014; 65:218-226.
16. Harnden P, Mahmood N and Southgate J. Expression of cytokeratin 20 redefines urothelial papillomas of the bladder. Lancet. 1999; 353:974-977.
17. Beukers W, Kandimalla R, Masius RG, Vermeij M, Kranse R, van Leenders GJ and Zwarthoff EC. Stratification based on methylation of TBX2 and TBX3 into three molecular grades predicts progression in patients with pTa-bladder cancer. Mod Pathol. 2015; 28:515-522.
18. Lu P, Weaver VM and Werb Z. The extracellular matrix: a dynamic niche in cancer progression. The Journal of cell biology. 2012; 196:395-406.
19. Aitken KJ and Bagli DJ. The bladder extracellular matrix. Part I: architecture, development and disease. Nature reviews Urology. 2009; 6:596-611.
20. Chen X, Nadiarynkh O, Plotnikov S and Campagnola PJ. Second harmonic generation microscopy for quantitative analysis of collagen fibrillar structure. Nature protocols. 2012; 7:654-669.
21. Levental KR, Yu H, Kass L, Lakins JN, Egeblad M, Erler JT, Fong SF, Csiszar K, Giaccia A, Weninger W, Yamauchi M, Gasser DL and Weaver VM. Matrix crosslinking forces tumor progression by enhancing integrin signaling. Cell. 2009; 139:891-906.
22. Egeblad M, Rasch MG and Weaver VM. Dynamic interplay between the collagen scaffold and tumor evolution. Current opinion in cell biology. 2010; 22:697-706.
23. Brabletz T, Spaderna S, Kolb J, Hlubek F, Faller G, Bruns CJ, Jung A, Nentwich J, Duluc I, Domon-Dell C, Kirchner T and Freund JN. Down-regulation of the homeodomain factor Cdx2 in colorectal cancer by collagen type I: an active role for the tumor environment in malignant tumor progression. Cancer research. 2004; 64:6973-6977.
24. Segal R, Yafi FA, Brimo F, Tanguay S, Aprikian A and Kassouf W. Prognostic factors and outcome in patients with T1 high-grade bladder cancer: can we identify patients for early cystectomy? BJU international. 2012; 109:1026-1030.
25. Provenzano PP, Eliceiri KW, Campbell JM, Inman DR, White JG and Keely PJ. Collagen reorganization at the tumor-stromal interface facilitates local invasion. BMC medicine. 2006; 4:38.
26. Provenzano PP, Inman DR, Eliceiri KW, Knittel JG, Yan L, Rueden CT, White JG and Keely PJ. Collagen density promotes mammary tumor initiation and progression. BMC medicine. 2008; 6:11.
27. Zhang K, Corsa CA, Ponik SM, Prior JL, Piwnica-Worms D, Eliceiri KW, Keely PJ and Longmore GD. The collagen receptor discoidin domain receptor 2 stabilizes SNAIL1 to facilitate breast cancer metastasis. Nat Cell Biol. 2013; 15:677-687.
28. Conklin MW, Eickhoff JC, Riching KM, Pehlke CA, Eliceiri KW, Provenzano PP, Friedl A and Keely PJ. Aligned collagen is a prognostic signature for survival in human breast carcinoma. Am J Pathol. 2011; 178:1221-1232.
29. Dyrskjot L, Reinert T, Novoradovsky A, Zuiverloon TC, Beukers W, Zwarthoff E, Malats N, Real FX, Segersten U, Malmstrom PU, Knowles M, Hurst C, Sorge J, et al. Analysis of molecular intra-patient variation and delineation of a prognostic 12-gene signature in non-muscle invasive bladder cancer; technology transfer from microarrays to PCR. Br J Cancer. 2012; 107:1392-1398.
30. Shin K, Lee J, Guo N, Kim J, Lim A, Qu L, Mysorekar IU and Beachy PA. Hedgehog/Wnt feedback supports regenerative proliferation of epithelial stem cells in bladder. Nature. 2011; 472:110-114.
31. Shin K, Lim A, Zhao C, Sahoo D, Pan Y, Spiekerkoetter E, Liao JC and Beachy PA. Hedgehog signaling restrains bladder cancer progression by eliciting stromal production of urothelial differentiation factors. Cancer cell. 2014; 26:521-533.
32. Kirkland SC and Ying H. Alpha2beta1 integrin regulates lineage commitment in multipotent human colorectal cancer cells. J Biol Chem. 2008; 283:27612-27619.
33. Oku Y, Shimoji T, Takifuji K, Hotta T, Yokoyama S, Matsuda K, Higashiguchi T, Tominaga T, Nasu T, Tamura K, Matsuura M, Miyata S, Kato Y, Yamaue H, et al. Identification of the molecular mechanisms for dedifferentiation at the invasion front of colorectal cancer by a gene expression analysis. Clinical cancer research : an official journal of the American Association for Cancer Research. 2008; 14:7215-7222.
34. Kirkland SC. Type I collagen inhibits differentiation and promotes a stem cell-like phenotype in human colorectal carcinoma cells. Br J Cancer. 2009; 101:320-326.
35. Chan KS, Espinosa I, Chao M, Wong D, Ailles L, Diehn M, Gill H, Presti J, Jr., Chang HY, van de Rijn M, Shortliffe L and Weissman IL. Identification, molecular characterization, clinical prognosis, and therapeutic targeting of human bladder tumor-initiating cells. Proceedings of the National Academy of Sciences of the United States of America. 2009; 106:14016-14021.
36. Ho PL, Kurtova A and Chan KS. Normal and neoplastic urothelial stem cells: getting to the root of the problem. Nature reviews Urology. 2012; 9:583-594.
37. Hedegaard J, Lamy P, Nordentoft I, Algaba F, Hoyer S, Ulhoi BP, Vang S, Reinert T, Hermann GG, Mogensen K, Thomsen MB, Nielsen MM, Marquez M, et al. Comprehensive Transcriptional Analysis of Early-Stage Urothelial Carcinoma. Cancer cell. 2016; 30:27-42.
38. Kurtova AV, Xiao J, Mo Q, Pazhanisamy S, Krasnow R, Lerner SP, Chen F, Roh TT, Lay E, Ho PL and Chan KS. Blocking PGE2-induced tumour repopulation abrogates bladder cancer chemoresistance. Nature. 2015; 517:209-213.
39. Kluth LA, Black PC, Bochner BH, Catto J, Lerner SP, Stenzl A, Sylvester R, Vickers AJ, Xylinas E and Shariat SF. Prognostic and Prediction Tools in Bladder Cancer: A Comprehensive Review of the Literature. European urology. 2015; 68:238-253.
40. Shariat SF, Zippe C, Ludecke G, Boman H, Sanchez-Carbayo M, Casella R, Mian C, Friedrich MG, Eissa S, Akaza H, Sawczuk I, Serretta V, Huland H, et al. Nomograms including nuclear matrix protein 22 for prediction of disease recurrence and progression in patients with Ta, T1 or CIS transitional cell carcinoma of the bladder. The Journal of urology. 2005; 173:1518-1525.
41. Dyrskjot L, Zieger K, Real FX, Malats N, Carrato A, Hurst C, Kotwal S, Knowles M, Malmstrom PU, de la Torre M, Wester K, Allory Y, Vordos D, et al. Gene expression signatures predict outcome in non-muscle-invasive bladder carcinoma: a multicenter validation study. Clinical cancer research : an official journal of the American Association for Cancer Research. 2007; 13:3545-3551.
42. Dalbagni G, Vora K, Kaag M, Cronin A, Bochner B, Donat SM and Herr HW. Clinical outcome in a contemporary series of restaged patients with clinical T1 bladder cancer. European urology. 2009; 56:903-910.
43. Gendy R, Delprado W, Brenner P, Brooks A, Coombes G, Cozzi P, Nash P and Patel MI. Repeat transurethral resection for non-muscle-invasive bladder cancer: a contemporary series. BJU international. 2016; 117 Suppl 4:54-59.
44. Herr HW. The value of a second transurethral resection in evaluating patients with bladder tumors. The Journal of urology. 1999; 162:74-76.

