Oncotarget: Paradox breaker BRAF inhibitors in BRAF mutant colorectal cancer
2020-08-25
Oncotarget Volume 11, Issue 34 features Figure 1, "BRAF inhibitor-induced changes in cell viability," by Pickles, et which reported that the BEACON CRC trial demonstrated a survival advantage over chemotherapy for a combination of targeted agents comprising the potent BRAF inhibitor encorafenib together with cetuximab and binimetinib.
Resistance to BRAF inhibition in CRC arises in part through the generation and activation of RAF dimers resulting in MEK-ERK pathway reactivation.
The Oncotarget authors analyzed whether paradox breakers reduce pathway reactivation and so have enhanced potency compared with encorafenib in BRAF mutant CRC.
However, dose-response curves for encorafenib and PLX8394 were similar and there were no significant differences in the degree of pathway reactivation.
To their knowledge, these data represent the first comparative data of encorafenib and paradox breaker inhibitors in BRAF mutant CRC.
Dr. Gary W. Middleton from The Institute of Immunology and Immunotherapy at The University of Birmingham said, "Around 10% of patients with metastatic colorectal cancer (CRC) harbour a BRAF mutation."
Recently results of the BEACON CRC trial demonstrated an enhanced survival for chemo-refractory BRAF mutant CRC patients for the combination of the BRAF inhibitor encorafenib together with the EGFR inhibitor cetuximab and the MEK inhibitor binimetinib compared with the control group of cetuximab and irinotecan-based therapy.
The addition of EGFR and MEK inhibition to the BRAF inhibitor backbone is predicated on the activation of RAS observed following BRAF inhibition.
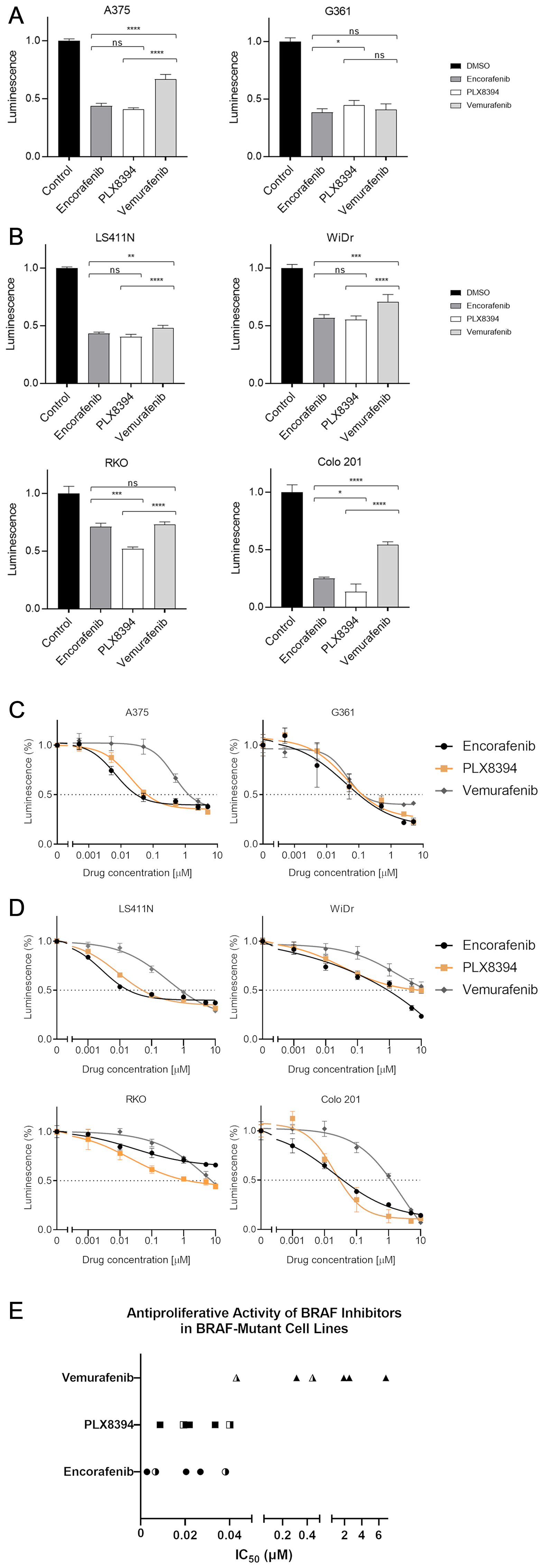
Figure 1: BRAF inhibitor-induced changes in cell viability. BRAF-mutant melanoma (A) and colorectal cancer (B) cell lines were treated with respective inhibitors at 1 μM for 48 hours prior to measuring luminescence. Changes in viability were measured using RealTime-Glo™ MT Cell Viability Assay and reported relative to vehicle-treated control. Mean values with standard deviations plotted from 5 replicates. Significance levels legend: Not significant (NS) P > 0.05; *P ≤ 0.05; **P ≤ 0.01; ***P ≤ 0.001; ****P ≤ 0.0001. N.B. Statistics for all drugs vs control not shown for ease of display and interpretation, all 3 compounds highly significant (P < 0.0001). Drug dose response curves. Sensitivity to respective BRAF inhibitors was evaluated in melanoma (C) and colorectal (D) cell lines. Cells were treated with 10,000-fold dilution series (0.001 μM to 10 μM) of respective BRAF inhibitors for 48 hours. Cell viability was assessed using RealTime-Glo™ MT Cell Viability Assay and reported relative to vehicle-treated control. The x-axis represents the log transformed inhibitor dose concentration. Mean values with standard deviation plotted from five replicates. (E) Derived IC50 values of BRAF inhibitors in melanoma and CRC cell lines (half-filled and filled symbols, respectively).
Encorafenib is a group 1 BRAF inhibitor that selectively inhibits active BRAF monomers.
This phenomenon causes pathway reactivation and resistance to BRAF inhibition in BRAF mutant cells and paradoxical pathway activation in BRAF wild-type cells.
PLX8394 is a paradox-breaker BRAF inhibitor that inhibits BRAF dimerization and which does not result in paradoxical activation in BRAF wild-type cells.
The Middleton Research Team concluded in their Oncotarget Research paper that they have shown that the strategy of using a paradox breaker BRAF inhibitor such as PLX8394 in order to reduce pathway reactivation through reduced RAF dimerization in BRAF mutant CRC is as effective as optimal group 1 inhibitors such as encorafenib.
The degree of pathway reactivation is similar likely due to the inability of PLX8394 to inhibit CRAF homodimer formation and the activation by PLX8394 of such dimers.
As with the continued clinical development of BRAF inhibition in BRAF mutant cancers, the activity of PLX8394 should be investigated as part of a combination with other drugs that limit pathway reactivation such as MEK and EGFR inhibitors.
However, the general strategy of targeting RAF dimerization in RAS/RAF mutant colorectal cancers is unlikely to qualitatively transform the outcomes with targeted therapies without appropriate attention to the unique biology of BRAF and KRAS mutant CRC.
The lack of confirmed objective responses in BRAF mutant CRC, in contradistinction to melanoma, to the RAF dimer inhibitor lifirafenib which inhibits all RAF isoforms as well as EGFR and KRAS supports this hypothesis.
Sign up for free Altmetric alerts about this article
DOI - https://doi.org/10.18632/oncotarget.27681
Full text - https://www.oncotarget.com/article/27681/text/
Correspondence to - Gary W. Middleton - [email protected]
Keywords - colorectal cancer, BRAF, paradox breaker, encorafenib, PLX8394
About Oncotarget
Oncotarget is a biweekly, peer-reviewed, open access biomedical journal covering research on all aspects of oncology.
To learn more about Oncotarget, please visit https://www.oncotarget.com or connect with:
SoundCloud - https://soundcloud.com/oncotarget
Facebook - https://www.facebook.com/Oncotarget/
Twitter - https://twitter.com/oncotarget
LinkedIn - https://www.linkedin.com/company/oncotarget
Pinterest - https://www.pinterest.com/oncotarget/
Reddit - https://www.reddit.com/user/Oncotarget/
Oncotarget is published by Impact Journals, LLC please visit http://www.ImpactJournals.com or connect with @ImpactJrnls
Media Contact
[email protected]
18009220957x105
Copyright © 2026 Rapamycin Press LLC dba Impact Journals
Oncotarget ® is a registered trademark of Rapamycin Press LLC
Impact Journals ® is a registered trademark of Rapamycin Press LLC
RAPAMYCIN PRESS ® is a registered trademark of Rapamycin Press LLC




