Outcome analysis of Phase I trial patients with metastatic KRAS and/or TP53 mutant non-small cell lung cancer
2020-01-20
About 10%, 18%, 36%, and 36% of the patients had metastatic KRAS+/TP53+, KRAS+/TP53-,KRAS-/TP53+, and KRAS-/TP53- NSCLC, respectively. Introduction of the evolutionary action score system of TP53 missense mutations enabled the research team to identify a subgroup of NSCLC patients with low-risk mutant p53 proteins having a median OS duration of 64.5 months after initial diagnosis of metastasis. These data suggested that patients with metastatic dual KRAS+/TP53+ hotspot-mutant NSCLC had poor clinical outcomes.
Dr. Siqing Fu from the Department of Investigational Cancer Therapeutics, The University of Texas MD Anderson Cancer Center, Houston, TX, USA said, "Non-small cell lung cancer (NSCLC), constituting more than 80% of all lung cancers, is the leading cause of cancer morbidity and mortality worldwide."
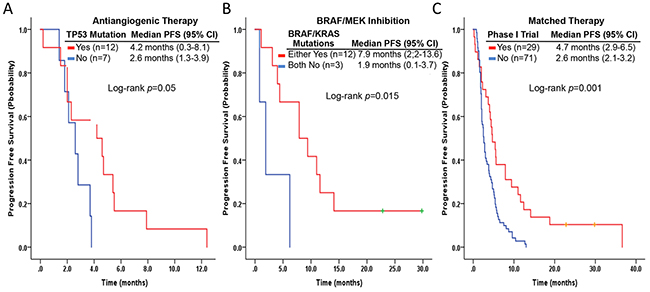
Figure 4: Kaplan-Meier curves of progression-free survivals in patients with metastatic NSCLC who received antiangiogenic phase 1 trial therapy according to TP53 hotspot mutation status (A), BRAF/MEK inhibitor-based phase 1 trial therapy according to BRAF or KRAS hotspot mutation status (B), and matched phase 1 trial therapy versus those who did not (C).
Mutations of KRAS, a member of the RAS family, are among the most common oncogene mutations in NSCLC patients, identified in up to 30% of NSCLC cases; are most frequently activating point mutations at codons G12, G13, and Q61; occur most often in patients with adenocarcinoma, who are white, and who are current or former smokers; and are mutually exclusive of epidermal growth factor receptor mutations and ALK and ROS1 rearrangements. Reported incidence rates for TP53 exon 5-8 mutations in NSCLC patients ranged from 31% to 79%, with mutations occurring most frequently in squamous cell carcinoma cases.
The Siqing Fu research team concluded, "KRAS hotspot mutations were more common in non-Asian patients than in Asian ones, previous and current smokers than in never-smokers, and patients without EGFR and BRAF mutations than in patients with EGFR and BRAF mutations; whereas TP53 hotspot mutations were more common in male patients than in female ones, patients with squamous cell carcinoma than in those with adenocarcinoma, and patients with poorly differentiated tumors than in well differentiated tumors. The association of improved clinical benefit and PFS with the antiangiogenic phase I trial therapy in patients with TP53 hotspot mutations provided additional evidence that antiangiogenic agent-based phase I trial therapy is appropriate for consideration as matched therapy in patients with TP53 mutant NSCLC."
Full text - https://doi.org/10.18632/oncotarget.25947
Correspondence to - Siqing Fu - [email protected]
Keywords - KRAS, TP53, Phase I trial, overall survival, non-small cell lung cancer
Copyright © 2026 Rapamycin Press LLC dba Impact Journals
Oncotarget ® is a registered trademark of Rapamycin Press LLC
Impact Journals ® is a registered trademark of Rapamycin Press LLC
RAPAMYCIN PRESS ® is a registered trademark of Rapamycin Press LLC




