Corrections:
Correction: A composite polymer nanoparticle overcomes multidrug resistance and ameliorates doxorubicin-associated cardiomyopathy
Metrics: PDF 142 views
1The Sol Goldman Pancreatic Cancer Research Center, Johns Hopkins University School of Medicine, Baltimore, Maryland 2Department of Pathology, Johns Hopkins University School of Medicine, Baltimore, Maryland 3Department of Molecular and Comparative Pathobiology, Johns Hopkins University School of Medicine, Baltimore, Maryland 4Department of Oncology, Johns Hopkins University School of Medicine, Baltimore, Maryland 5Department of Internal Medicine 3, Center of Integrated Oncology Cologne-Bonn, University of Bonn, Germany 6Senior Scientist, Indian National Science Academy, New Delhi, India. π Deceased *Constitutes equal contribution
Published: April 24, 2026
This article has been corrected:This article has been corrected: It was noted that the immunofluorescence image for ‘NanoDox’ (ND) in Figure 2C was incorrectly selected, resulting in identical images being shown for both the vehicle (Veh) and ND post-treatment levels of MDR1 expression in RPMI8226/Dox xenografts.
The authors have provided a corrected Figure 2C using the original image for the ND post-treatment level of MDR1 expression. The replacement of this image does not alter the study’s conclusions. The authors sincerely apologize for any inconvenience this may cause to readers.
Original article: Oncotarget. 2012; 3:640-650. DOI: https://doi.org/10.18632/oncotarget.543.
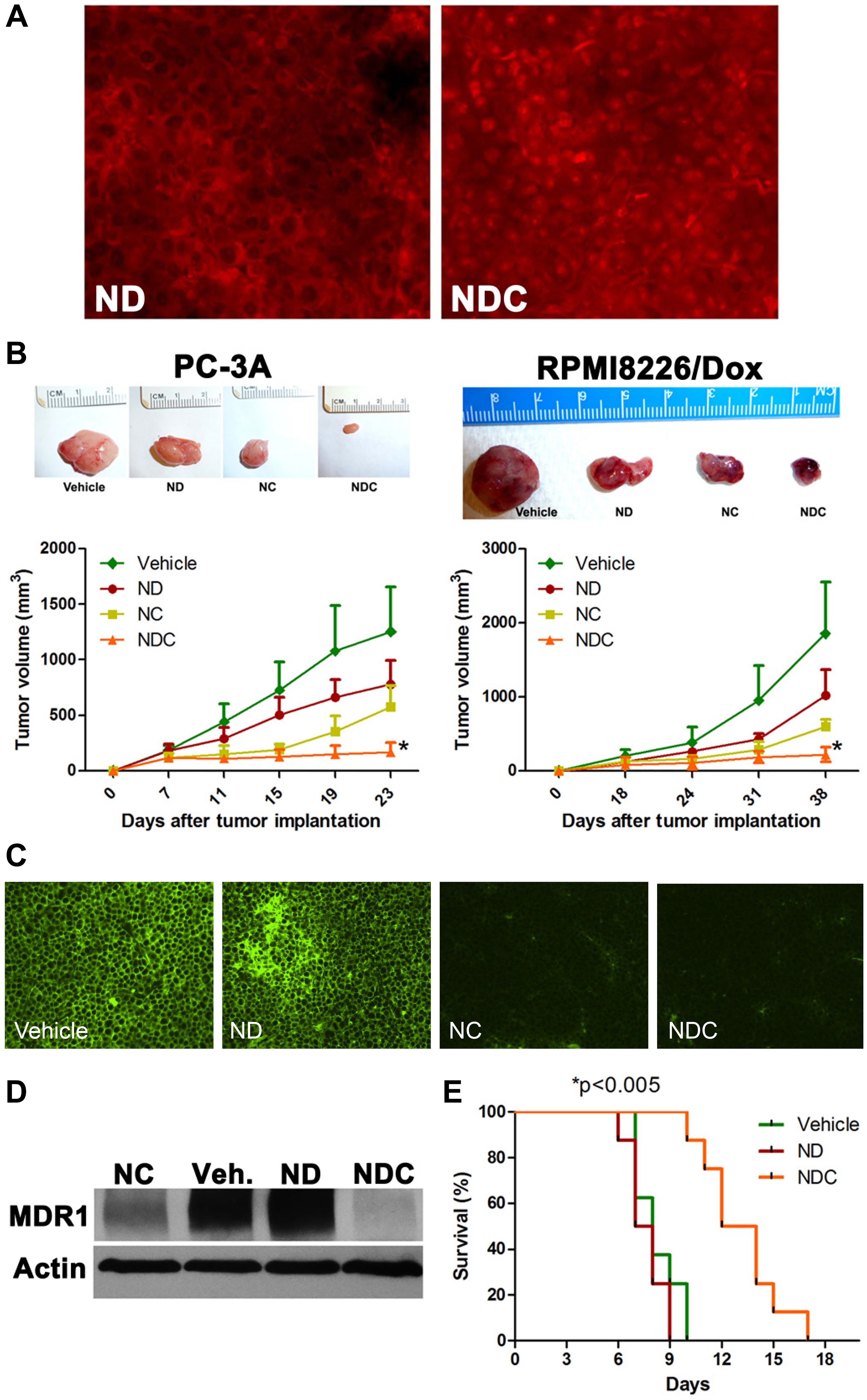
Figure 2: NDC overcomes DOX resistance in vivo. (A) Representative tumor sections from RPMI8226/Dox xenografts were examined by fluorescence microscopy for nuclear accumulation of DOX by doxorubicin fluorescence. (B) NDC significantly inhibits the growth of subcutaneous DOX-resistant cancer xenografts PC-3A and RPMI8226/Dox. Representative excised xenograft tumors from each of the four arms are illustrated. NDC significantly blocked tumor growth compared to either ND or NC (N = 5, *p < 0.005). Post treatment levels of MDR1 expression were measured by (C) immunofluorescence and (D) western blot in RPMI8226/Dox xenografts. (E) BDF1 mice bearing P388/ADR DOX-resistant ascites were treated with vehicle, ND, or NDC. A greater than 50% increase in survival was observed in NDC treated mice compared to ND or vehicle treated mice (N = 8, *p < 0.005).

